Table of Contents
Introduction
Naproxen is a nonsteroidal anti-inflammatory drug (NSAID) widely used for its analgesic, anti-inflammatory, and antipyretic effects. It is commonly prescribed in conditions such as arthritis, musculoskeletal pain, dysmenorrhea, and fever. Naproxen works by inhibiting the synthesis of prostaglandins, which are key mediators of inflammation and pain.
Mechanism of Action (Step-wise)
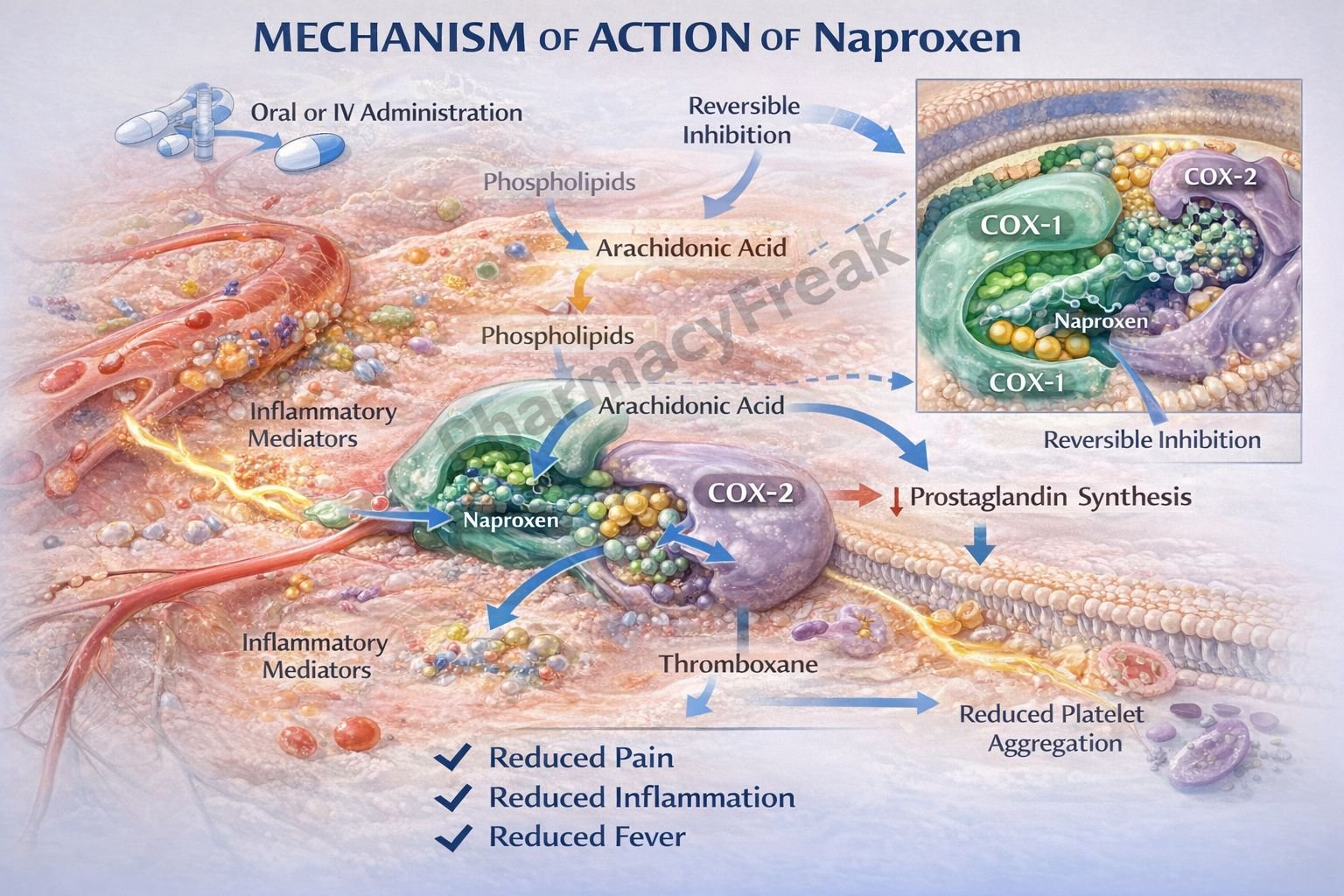
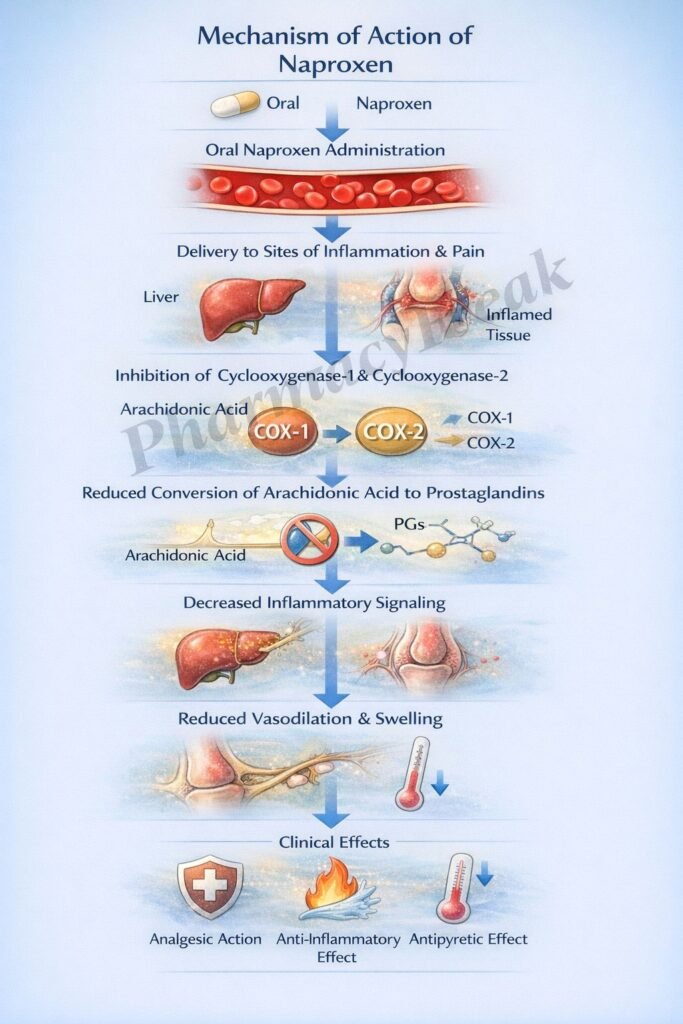
- Naproxen inhibits cyclooxygenase (COX) enzymes, including COX-1 and COX-2.
- These enzymes convert arachidonic acid into prostaglandins and thromboxanes.
- By inhibiting COX enzymes, naproxen reduces prostaglandin synthesis.
- Prostaglandins are responsible for pain, inflammation, and fever.
- Reduced prostaglandins decrease sensitization of nociceptors, leading to analgesia.
- Decreased prostaglandins also reduce vasodilation and edema, lowering inflammation.
- In the hypothalamus, reduced prostaglandins help lower body temperature (antipyretic effect).
- Inhibition of COX-1 reduces thromboxane A2 production, affecting platelet aggregation.
- The overall effect is reduced pain, inflammation, and fever.
A key exam point is that naproxen is a non-selective COX inhibitor that reduces prostaglandin synthesis.
Pharmacokinetics
Naproxen is administered orally and is well absorbed from the gastrointestinal tract. It has a relatively long half-life compared to many NSAIDs, allowing less frequent dosing. It is highly protein-bound and metabolized in the liver. It is excreted mainly via the kidneys. Its long duration makes it suitable for chronic inflammatory conditions.
Clinical Uses
Naproxen is used in the treatment of rheumatoid arthritis, osteoarthritis, ankylosing spondylitis, and acute musculoskeletal pain. It is also effective in dysmenorrhea and migraine. Its anti-inflammatory properties make it useful in chronic inflammatory disorders.
Adverse Effects
Common adverse effects include gastrointestinal irritation, nausea, and dyspepsia. More serious effects include gastric ulceration and bleeding due to COX-1 inhibition. Renal impairment may occur with prolonged use. It may also increase cardiovascular risk. Platelet inhibition can increase bleeding tendency.
Comparative Analysis
| Feature | Naproxen | Ibuprofen | Celecoxib |
|---|---|---|---|
| COX selectivity | Non-selective | Non-selective | COX-2 selective |
| Duration | Long | Short | Moderate |
| GI side effects | Moderate–high | Moderate | Lower |
| Cardiovascular risk | Moderate | Low–moderate | Higher |
| Platelet effect | Yes | Yes | Minimal |
| Use | Pain, inflammation | Pain, fever | Inflammation |
Naproxen differs from ibuprofen by having a longer duration of action. Compared to celecoxib, it inhibits both COX-1 and COX-2, leading to more gastrointestinal side effects but less selective action.
MCQs
- Naproxen belongs to which class?
a) Opioids
b) NSAIDs
c) Antidepressants
d) Antibiotics
Answer: b) NSAIDs
- Naproxen inhibits which enzyme?
a) DNA polymerase
b) Cyclooxygenase
c) RNA polymerase
d) ATP synthase
Answer: b) Cyclooxygenase
- COX enzymes produce:
a) Proteins
b) Prostaglandins
c) Lipids
d) Hormones
Answer: b) Prostaglandins
- Naproxen reduces:
a) Insulin
b) Prostaglandins
c) Calcium
d) Sodium
Answer: b) Prostaglandins
- Analgesic effect is due to:
a) Increased prostaglandins
b) Decreased nociceptor sensitization
c) Increased calcium
d) Increased sodium
Answer: b) Decreased nociceptor sensitization
- Naproxen acts as:
a) Antipyretic
b) Antidepressant
c) Antidiabetic
d) Anticoagulant
Answer: a) Antipyretic
- Naproxen affects platelet aggregation by reducing:
a) Thromboxane A2
b) Serotonin
c) Dopamine
d) Histamine
Answer: a) Thromboxane A2
- A common adverse effect is:
a) Hypoglycemia
b) Gastric irritation
c) Hypercalcemia
d) Bradycardia
Answer: b) Gastric irritation
- Naproxen is metabolized in the:
a) Kidney
b) Liver
c) Lung
d) Brain
Answer: b) Liver
- Naproxen is excreted via:
a) Liver
b) Kidney
c) Lung
d) Skin
Answer: b) Kidney
- Compared to ibuprofen, naproxen has:
a) Shorter duration
b) Longer duration
c) Same duration
d) No effect
Answer: b) Longer duration
- Naproxen increases risk of:
a) Hypotension
b) GI bleeding
c) Hypoglycemia
d) Anemia
Answer: b) GI bleeding
FAQs
What is the mechanism of action of naproxen?
It inhibits COX enzymes, reducing prostaglandin synthesis and inflammation.
Is naproxen selective for COX-2?
No, it is a non-selective COX inhibitor.
Why does naproxen cause gastric irritation?
Due to inhibition of COX-1, which protects the gastric mucosa.
What is the main use of naproxen?
Pain and inflammatory conditions such as arthritis.
Does naproxen affect platelets?
Yes, it reduces thromboxane A2 and affects platelet aggregation.
Why is naproxen dosed less frequently?
Because of its long half-life.
References
Goodman & Gilman’s The Pharmacological Basis of Therapeutics – NSAIDs
https://accessmedicine.mhmedical.com/book.aspx?bookid=3191
Katzung: Basic and Clinical Pharmacology – NSAIDs
https://accessmedicine.mhmedical.com/content.aspx?bookid=3382
Tripathi: Essentials of Medical Pharmacology – NSAIDs
https://www.jaypeedigital.com
Harrison’s Principles of Internal Medicine – Pain and Inflammation
https://accessmedicine.mhmedical.com