Table of Contents
Introduction
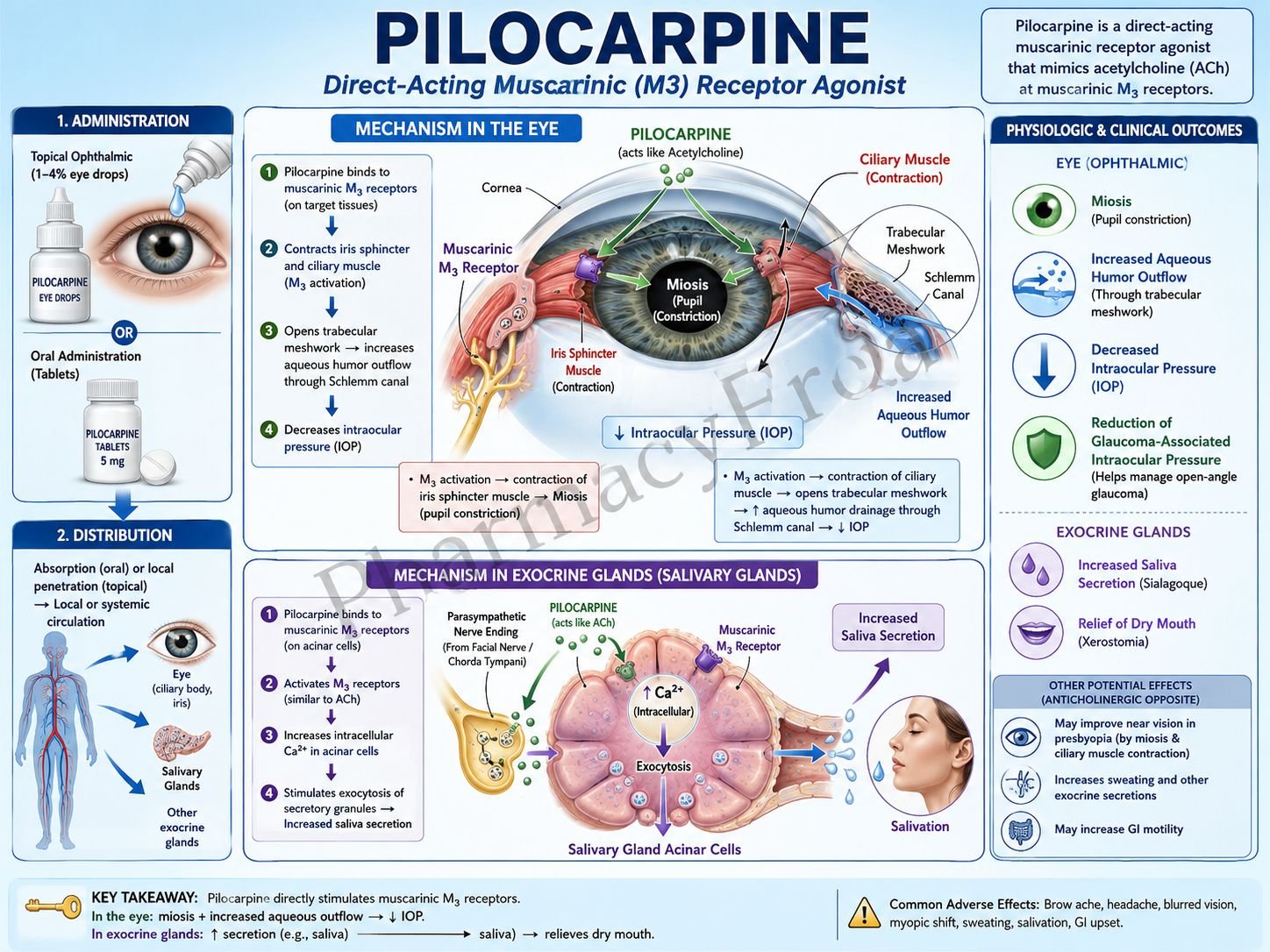
Pilocarpine is a direct-acting muscarinic receptor agonist used primarily in glaucoma and xerostomia. It mimics the action of acetylcholine at muscarinic receptors, producing parasympathetic effects. In ophthalmology, pilocarpine lowers intraocular pressure by increasing aqueous humor outflow. It is also used to stimulate salivary secretion in conditions such as Sjögren syndrome.
Mechanism of Action (Step-wise)
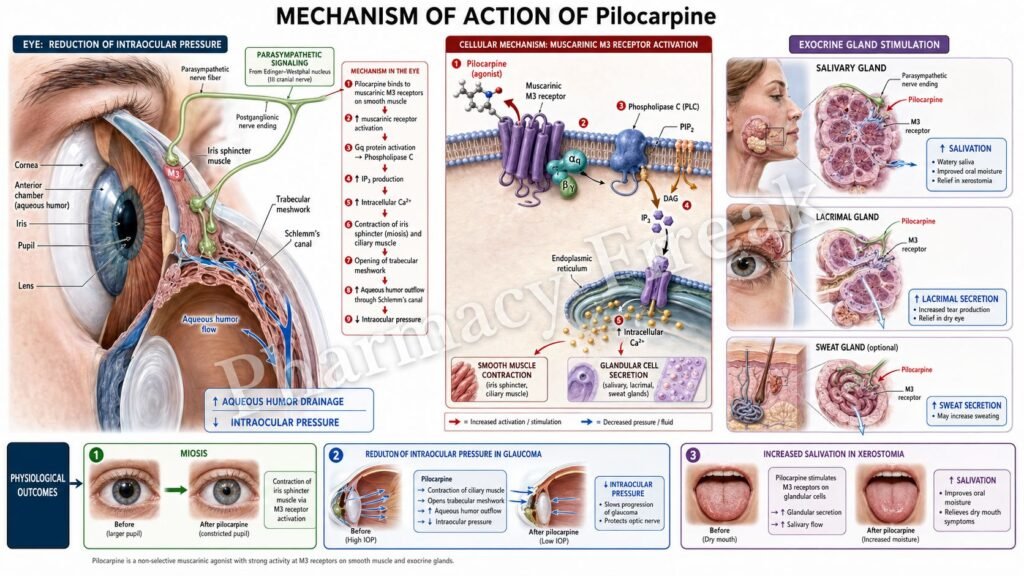
- Pilocarpine directly stimulates muscarinic cholinergic receptors.
- It has predominant activity at M3 muscarinic receptors.
- M3 receptors are coupled to Gq proteins.
- Activation of Gq stimulates phospholipase C (PLC).
- PLC converts PIP2 into IP3 and DAG.
- IP3 increases intracellular calcium release.
- Increased calcium causes contraction of smooth muscles and glandular secretion.
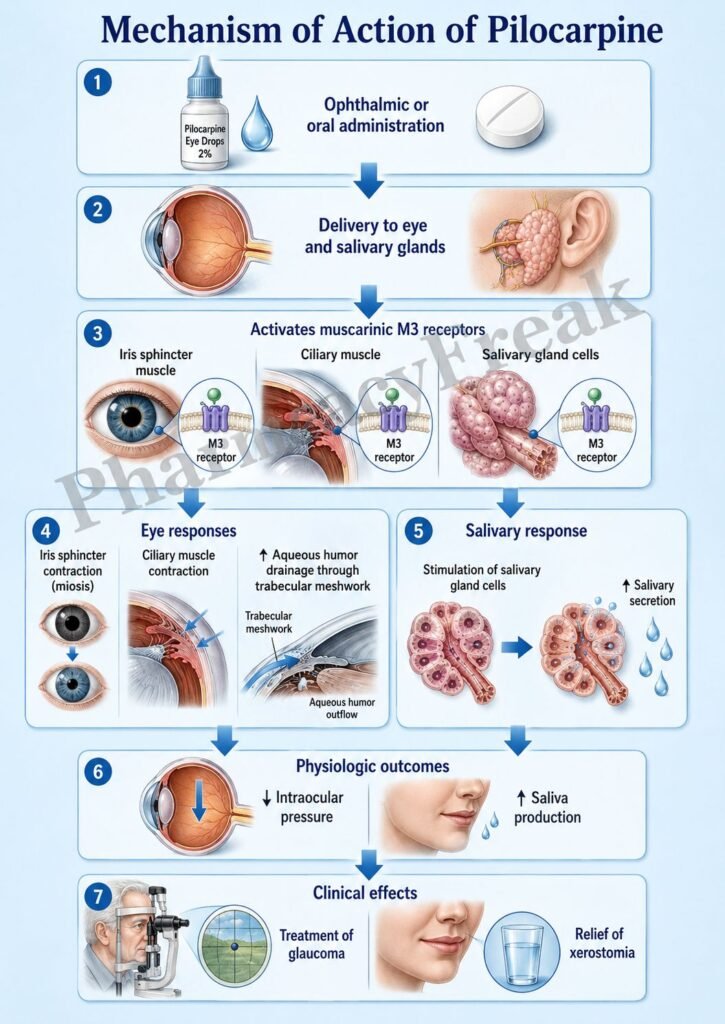
- In the eye, pilocarpine contracts the sphincter pupillae muscle causing miosis.
- It also contracts the ciliary muscle.
- Ciliary muscle contraction opens the trabecular meshwork.
- This increases aqueous humor outflow through the canal of Schlemm.
- Increased outflow lowers intraocular pressure.
- In salivary glands, M3 activation increases saliva secretion.
- The overall effect is enhanced parasympathetic activity.
A key exam point is that pilocarpine is a direct muscarinic agonist that causes miosis and increases aqueous humor drainage.
Pharmacokinetics
Pilocarpine can be administered topically as eye drops or orally for xerostomia. It is well absorbed and distributed. The duration of action depends on the route of administration. It is metabolized in the liver and excreted via the kidneys.
Clinical Uses
Pilocarpine is used in glaucoma to reduce intraocular pressure. It is also used in xerostomia associated with Sjögren syndrome or radiation therapy. In ophthalmology, it may be used to induce miosis during certain procedures.
Adverse Effects
Common adverse effects include sweating, salivation, bronchospasm, abdominal cramps, and bradycardia due to muscarinic stimulation. Ophthalmic use may cause blurred vision and difficulty seeing in low light because of miosis.
Comparative Analysis
| Feature | Pilocarpine | Physostigmine | Atropine |
|---|---|---|---|
| Mechanism | Direct muscarinic agonist | AChE inhibition | Muscarinic antagonist |
| Effect on pupil | Miosis | Miosis | Mydriasis |
| Glaucoma use | Yes | Sometimes | No |
| Salivary secretion | Increased | Increased indirectly | Decreased |
| CNS penetration | Minimal | Yes | Yes |
| Parasympathetic effect | Direct stimulation | Increased ACh | Blockade |
Pilocarpine differs from physostigmine because it directly stimulates muscarinic receptors instead of inhibiting acetylcholinesterase. Compared to atropine, it produces opposite parasympathetic effects.
MCQs
- Pilocarpine primarily stimulates which receptor?
a) Nicotinic receptor
b) Muscarinic receptor
c) Dopamine receptor
d) Histamine receptor
Answer: b) Muscarinic receptor
- Pilocarpine mainly acts on which muscarinic subtype?
a) M1
b) M2
c) M3
d) M4
Answer: c) M3
- M3 receptors are coupled to:
a) Gi proteins
b) Gq proteins
c) Gs proteins
d) None
Answer: b) Gq proteins
- Activation of M3 receptors increases:
a) cAMP
b) IP3 and DAG
c) ATP
d) ADP
Answer: b) IP3 and DAG
- Pilocarpine causes:
a) Mydriasis
b) Miosis
c) Cycloplegia
d) Tachycardia
Answer: b) Miosis
- Pilocarpine lowers intraocular pressure by:
a) Reducing aqueous production
b) Increasing aqueous outflow
c) Blocking β receptors
d) Inhibiting carbonic anhydrase
Answer: b) Increasing aqueous outflow
- Pilocarpine is used in:
a) Asthma
b) Glaucoma
c) Diabetes
d) Hypertension
Answer: b) Glaucoma
- Pilocarpine increases:
a) Salivation
b) Blood glucose
c) Heart rate
d) Sodium levels
Answer: a) Salivation
- A common adverse effect is:
a) Dry mouth
b) Sweating
c) Hyperglycemia
d) Mydriasis
Answer: b) Sweating
- Pilocarpine contracts which ocular muscle?
a) Dilator pupillae
b) Sphincter pupillae
c) Extraocular muscle
d) Levator palpebrae
Answer: b) Sphincter pupillae
- Compared to atropine, pilocarpine causes:
a) Opposite parasympathetic effects
b) Same effects
c) No ocular effect
d) CNS depression only
Answer: a) Opposite parasympathetic effects
- Pilocarpine increases aqueous humor drainage through:
a) Vitreous body
b) Trabecular meshwork
c) Retina
d) Lens
Answer: b) Trabecular meshwork
FAQs
What is the mechanism of action of pilocarpine?
It directly stimulates muscarinic receptors, especially M3 receptors.
How does pilocarpine lower intraocular pressure?
By increasing aqueous humor outflow through the trabecular meshwork.
Why does pilocarpine cause miosis?
Due to contraction of the sphincter pupillae muscle.
What is its role in xerostomia?
It stimulates salivary gland secretion.
What are common side effects?
Sweating, salivation, bronchospasm, and blurred vision.
How does pilocarpine differ from atropine?
Pilocarpine stimulates muscarinic receptors, while atropine blocks them.
References
Goodman & Gilman’s The Pharmacological Basis of Therapeutics – Cholinergic Drugs
https://accessmedicine.mhmedical.com/book.aspx?bookid=3191
Katzung: Basic and Clinical Pharmacology – Cholinomimetic Drugs
https://accessmedicine.mhmedical.com/content.aspx?bookid=3382
Tripathi: Essentials of Medical Pharmacology – Cholinergic Drugs
https://www.jaypeedigital.com
Harrison’s Principles of Internal Medicine – Glaucoma
https://accessmedicine.mhmedical.com