Table of Contents
Introduction
Loratadine is a second-generation antihistamine widely used in the treatment of allergic conditions such as allergic rhinitis and urticaria. It selectively antagonizes peripheral histamine H1 receptors, thereby reducing allergic symptoms without causing significant sedation. Compared to first-generation antihistamines, loratadine has minimal penetration into the central nervous system, making it a preferred choice for daytime use.
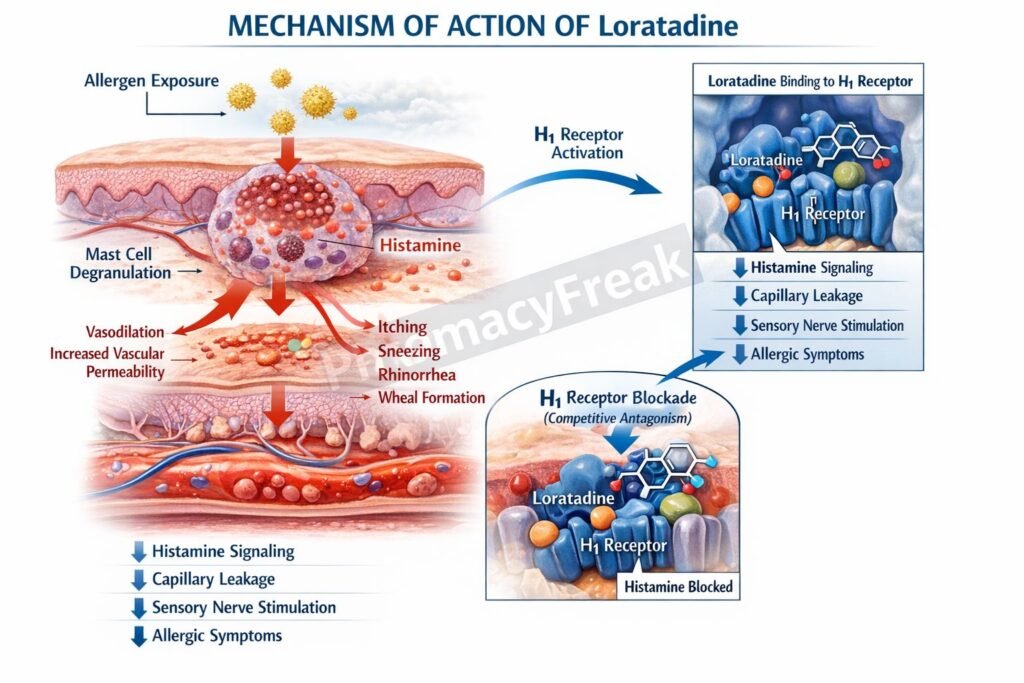
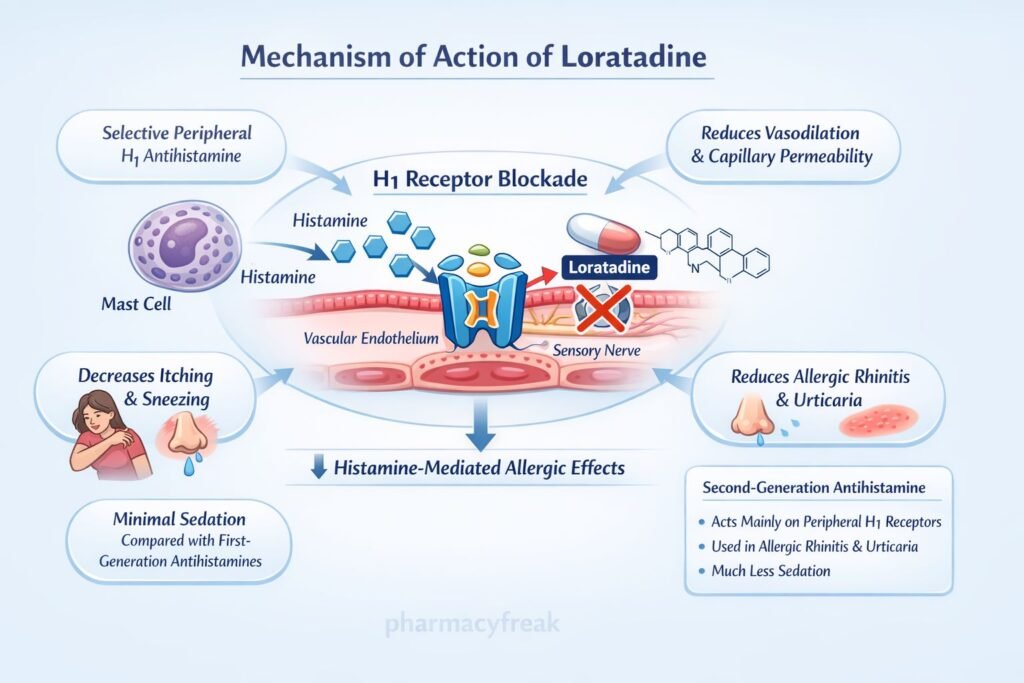

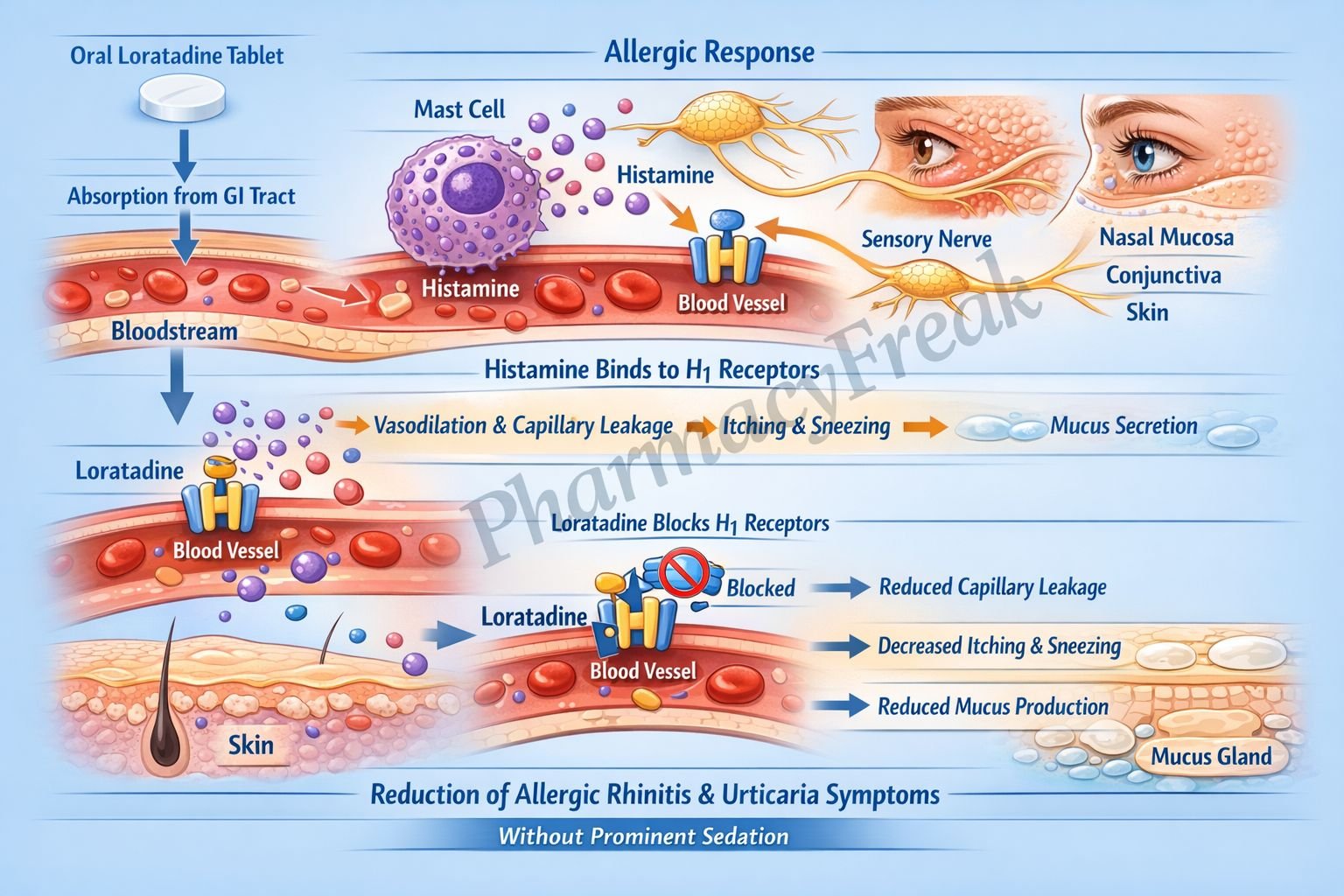
Mechanism of Action (Step-wise)
- Loratadine acts as a selective antagonist of peripheral H1 histamine receptors.
- It binds to H1 receptors on target cells such as vascular endothelium, smooth muscle, and sensory nerves.
- By blocking histamine binding, it prevents histamine-mediated effects such as vasodilation and increased vascular permeability.
- This reduces edema formation and tissue swelling associated with allergic reactions.
- It inhibits stimulation of sensory nerve endings, thereby reducing itching and sneezing.
- Loratadine also decreases mucus secretion in the respiratory tract.
- It does not significantly cross the blood-brain barrier due to its low lipophilicity and P-glycoprotein efflux.
- Therefore, central sedation is minimal compared to first-generation antihistamines.
A key exam point is that loratadine is a peripheral H1 receptor blocker with minimal sedative effect.
Pharmacokinetics
Loratadine is administered orally and is well absorbed from the gastrointestinal tract. It undergoes first-pass metabolism in the liver via cytochrome P450 enzymes, primarily CYP3A4 and CYP2D6, to form its active metabolite, desloratadine. Peak plasma levels occur within 1 to 3 hours for loratadine and slightly later for its metabolite. It is highly protein-bound and has a relatively long duration of action, allowing once-daily dosing. Elimination occurs through both urine and feces.
Clinical Uses
Loratadine is primarily used in allergic conditions. It is effective in allergic rhinitis, where it reduces sneezing, rhinorrhea, and nasal itching. It is also used in chronic urticaria to reduce itching and wheal formation. It is preferred in patients who require antihistamine therapy without sedation, such as students or individuals operating machinery. It may also be used in other mild allergic conditions such as conjunctivitis.
Adverse Effects
Loratadine is generally well tolerated. Common adverse effects include headache, dry mouth, and fatigue, although sedation is minimal compared to first-generation antihistamines. Rare adverse effects include tachycardia and gastrointestinal discomfort. Because it is metabolized in the liver, caution is required in patients with hepatic impairment. Drug interactions may occur with CYP3A4 inhibitors, potentially increasing loratadine levels.
Comparative Analysis
| Feature | Loratadine | Diphenhydramine | Cetirizine |
|---|---|---|---|
| Generation | Second | First | Second |
| CNS penetration | Minimal | High | Moderate |
| Sedation | Minimal | High | Mild |
| Anticholinergic effects | Minimal | Significant | Minimal |
| Duration | Long (once daily) | Short | Long |
| Use in allergy | Yes | Yes | Yes |
Loratadine differs from diphenhydramine in having minimal CNS penetration and therefore less sedation and fewer anticholinergic effects. Compared to cetirizine, loratadine is generally less sedating, making it more suitable for daytime use in sensitive individuals.
MCQs
- Loratadine belongs to which class of drugs?
a) Beta blockers
b) H1 antihistamines
c) Corticosteroids
d) Leukotriene antagonists
Answer: b) H1 antihistamines
- Loratadine primarily acts by blocking:
a) H2 receptors
b) H1 receptors
c) Dopamine receptors
d) Serotonin receptors
Answer: b) H1 receptors
- Loratadine is classified as:
a) First-generation antihistamine
b) Second-generation antihistamine
c) Third-generation antihistamine
d) Anti-IgE agent
Answer: b) Second-generation antihistamine
- The reduced sedation of loratadine is due to:
a) High lipid solubility
b) Increased CNS penetration
c) Poor blood-brain barrier penetration
d) Strong CNS binding
Answer: c) Poor blood-brain barrier penetration
- Loratadine is metabolized to:
a) Cetirizine
b) Desloratadine
c) Fexofenadine
d) Chlorpheniramine
Answer: b) Desloratadine
- Loratadine is commonly used in:
a) Hypertension
b) Asthma
c) Allergic rhinitis
d) Diabetes
Answer: c) Allergic rhinitis
- Which symptom is reduced by loratadine?
a) Hyperglycemia
b) Sneezing
c) Bradycardia
d) Muscle weakness
Answer: b) Sneezing
- Compared to diphenhydramine, loratadine causes:
a) More sedation
b) Equal sedation
c) Less sedation
d) No effect
Answer: c) Less sedation
- A common adverse effect of loratadine is:
a) Severe sedation
b) Headache
c) Renal failure
d) Hypoglycemia
Answer: b) Headache
- Loratadine blocks histamine-induced:
a) Vasoconstriction
b) Vasodilation
c) Insulin release
d) Calcium influx
Answer: b) Vasodilation
- Loratadine is preferred because it:
a) Causes strong CNS depression
b) Has minimal anticholinergic effects
c) Causes severe hypotension
d) Is short acting
Answer: b) Has minimal anticholinergic effects
- Which enzyme system metabolizes loratadine?
a) CYP3A4 and CYP2D6
b) CYP1A2 only
c) Monoamine oxidase
d) Aldehyde oxidase
Answer: a) CYP3A4 and CYP2D6
FAQs
What is the mechanism of action of loratadine?
It blocks peripheral H1 histamine receptors, preventing allergic responses such as vasodilation, itching, and mucus secretion.
Why does loratadine cause less sedation?
It has poor penetration across the blood-brain barrier.
What is the active metabolite of loratadine?
Desloratadine.
Is loratadine safe for long-term use?
Yes, it is commonly used for chronic allergic conditions with a good safety profile.
Can loratadine be used in children?
Yes, it is approved for use in pediatric patients for allergic conditions.
Does loratadine have anticholinergic effects?
Minimal compared to first-generation antihistamines.
References
Goodman & Gilman’s The Pharmacological Basis of Therapeutics – Antihistamines
https://accessmedicine.mhmedical.com/book.aspx?bookid=3191
Katzung: Basic and Clinical Pharmacology – Antihistamines
https://accessmedicine.mhmedical.com/content.aspx?bookid=3382
Tripathi: Essentials of Medical Pharmacology – Antihistamines
https://www.jaypeedigital.com
Harrison’s Principles of Internal Medicine – Allergic Disorders
https://accessmedicine.mhmedical.com