Table of Contents
Introduction
Nebivolol is a third-generation, highly selective β1-adrenergic receptor blocker with additional vasodilatory properties. It is primarily used in the management of hypertension and heart failure. Unlike traditional beta-blockers, nebivolol uniquely enhances nitric oxide (NO) release, contributing to improved vascular function and reduced peripheral resistance.
Mechanism of Action (Step-wise)
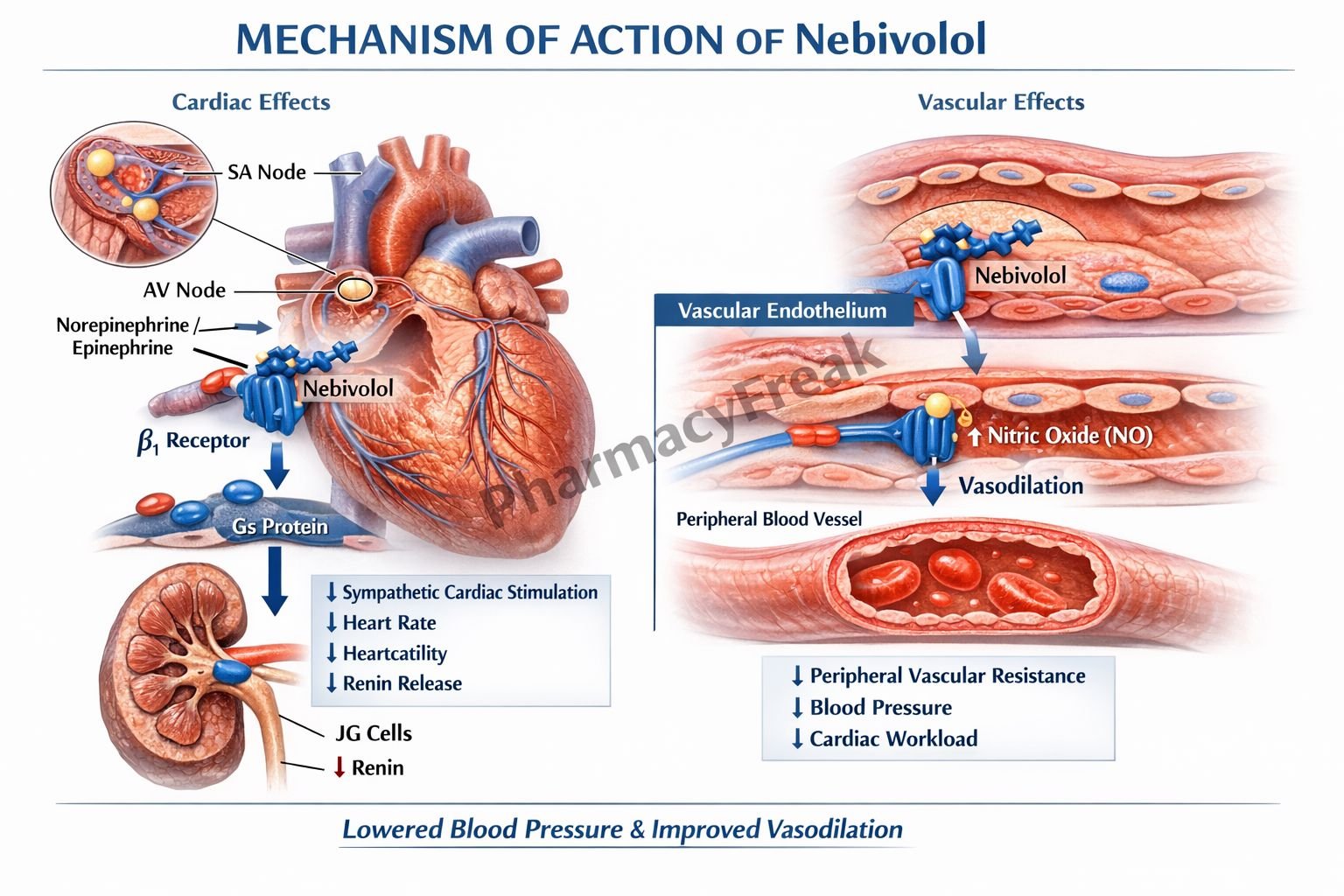
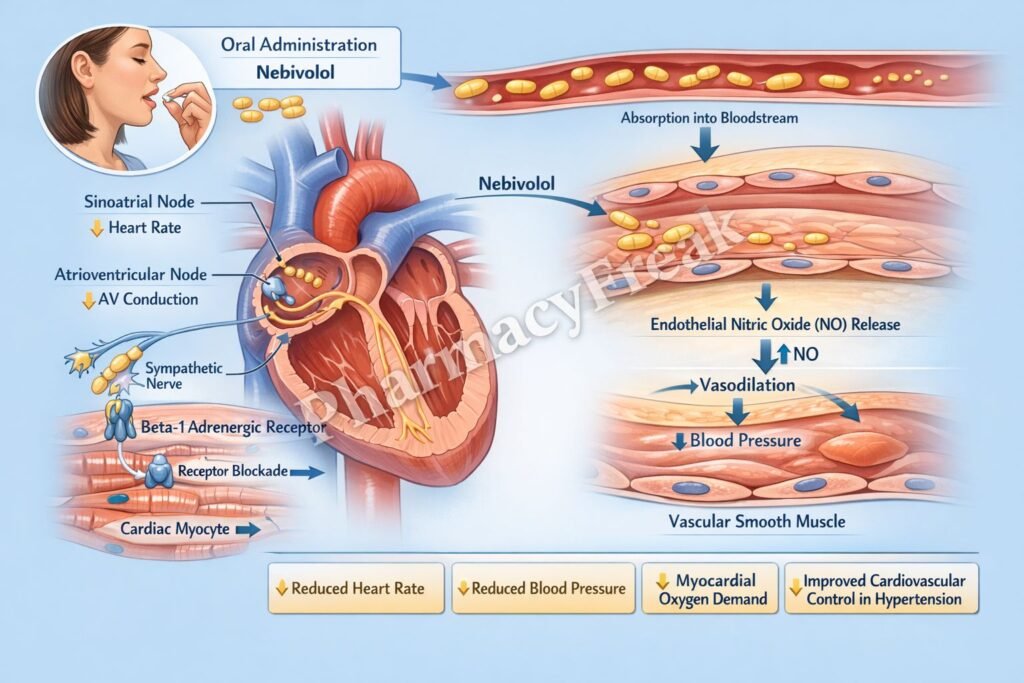
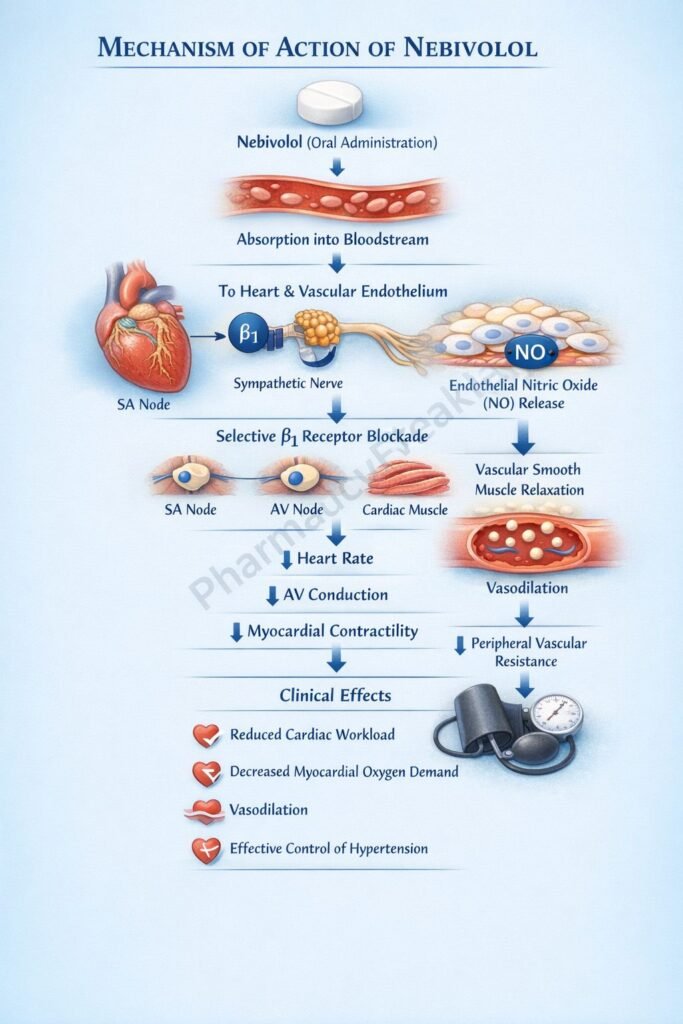
- Nebivolol selectively blocks β1-adrenergic receptors in the heart.
- β1 receptors normally respond to catecholamines such as norepinephrine.
- Blockade reduces activation of adenylate cyclase.
- This decreases cyclic AMP (cAMP) levels in cardiac cells.
- Reduced cAMP lowers calcium influx through voltage-gated calcium channels.
- This leads to decreased heart rate (negative chronotropic effect).
- It also reduces myocardial contractility (negative inotropic effect).
- Nebivolol stimulates endothelial nitric oxide synthase (eNOS).
- This increases nitric oxide (NO) production in blood vessels.
- NO activates guanylate cyclase, increasing cyclic GMP (cGMP).
- Increased cGMP causes smooth muscle relaxation and vasodilation.
- The combined effects reduce cardiac output and peripheral vascular resistance.
A key exam point is that nebivolol is a β1-selective blocker with additional nitric oxide–mediated vasodilation.
Pharmacokinetics
Nebivolol is administered orally and is well absorbed. It undergoes extensive hepatic metabolism, primarily via CYP2D6. It has a relatively long half-life, allowing once-daily dosing. It is highly protein-bound and excreted via both renal and hepatic routes. Genetic variation in CYP2D6 metabolism can affect its pharmacokinetics.
Clinical Uses
Nebivolol is used in the treatment of hypertension, where it lowers blood pressure through both cardiac and vascular mechanisms. It is also used in heart failure to reduce cardiac workload and improve outcomes. Its vasodilatory effect may provide additional benefits in patients with endothelial dysfunction.
Adverse Effects
Common adverse effects include bradycardia, fatigue, dizziness, and hypotension. Compared to non-selective beta-blockers, it has a lower risk of bronchoconstriction. It may still mask symptoms of hypoglycemia in diabetic patients. Due to its vasodilatory effect, it may cause headache or flushing.
Comparative Analysis
| Feature | Nebivolol | Metoprolol | Propranolol |
|---|---|---|---|
| Selectivity | β1 selective | β1 selective | Non-selective |
| Vasodilation | Yes (NO-mediated) | No | No |
| CNS penetration | Moderate | High | High |
| Effect on lungs | Minimal | Minimal | Significant |
| Additional benefit | Endothelial function | None | None |
| Use | Hypertension, HF | Hypertension, HF | Hypertension, arrhythmias |
Nebivolol differs from metoprolol by having nitric oxide–mediated vasodilatory action. Compared to propranolol, it is more selective and has fewer respiratory side effects.
MCQs
- Nebivolol primarily blocks which receptor?
a) α1 receptor
b) β1 receptor
c) β2 receptor
d) Dopamine receptor
Answer: b) β1 receptor
- Nebivolol reduces cAMP by:
a) Activating adenylate cyclase
b) Inhibiting adenylate cyclase
c) Increasing ATP
d) Blocking DNA
Answer: b) Inhibiting adenylate cyclase
- Reduced cAMP leads to decreased:
a) Sodium
b) Calcium
c) Potassium
d) Chloride
Answer: b) Calcium
- Nebivolol causes vasodilation by increasing:
a) Serotonin
b) Nitric oxide
c) Dopamine
d) Histamine
Answer: b) Nitric oxide
- Nitric oxide increases:
a) cAMP
b) cGMP
c) ATP
d) ADP
Answer: b) cGMP
- Nebivolol decreases heart rate by acting on:
a) AV node only
b) SA node
c) Ventricles
d) Kidneys
Answer: b) SA node
- Nebivolol is used in:
a) Asthma
b) Hypertension
c) Diabetes
d) Anemia
Answer: b) Hypertension
- A common adverse effect is:
a) Tachycardia
b) Bradycardia
c) Hypercalcemia
d) Hypoglycemia
Answer: b) Bradycardia
- Nebivolol is metabolized by:
a) CYP3A4
b) CYP2D6
c) CYP2C9
d) CYP1A2
Answer: b) CYP2D6
- Compared to propranolol, nebivolol has:
a) More bronchoconstriction
b) Less bronchoconstriction
c) Same effect
d) No effect
Answer: b) Less bronchoconstriction
- Nebivolol reduces blood pressure by:
a) Increasing cardiac output
b) Decreasing cardiac output and vasodilation
c) Increasing sodium
d) Increasing heart rate
Answer: b) Decreasing cardiac output and vasodilation
- Nebivolol has which unique feature?
a) Dopamine release
b) Nitric oxide release
c) Histamine blockade
d) Calcium activation
Answer: b) Nitric oxide release
FAQs
What is the mechanism of action of nebivolol?
It blocks β1 receptors and increases nitric oxide release, reducing heart rate and causing vasodilation.
Why is nebivolol considered a third-generation beta-blocker?
Because of its additional vasodilatory effect via nitric oxide.
Does nebivolol affect the lungs?
It is β1 selective, so it has minimal effect on β2 receptors at therapeutic doses.
What is its role in hypertension?
It lowers blood pressure by reducing cardiac output and vascular resistance.
Why can nebivolol cause bradycardia?
Due to β1 receptor blockade in the heart.
How is nebivolol different from metoprolol?
It also causes nitric oxide–mediated vasodilation.
References
Goodman & Gilman’s The Pharmacological Basis of Therapeutics – Adrenergic Drugs
https://accessmedicine.mhmedical.com/book.aspx?bookid=3191
Katzung: Basic and Clinical Pharmacology – Beta Blockers
https://accessmedicine.mhmedical.com/content.aspx?bookid=3382
Tripathi: Essentials of Medical Pharmacology – Adrenergic Drugs
https://www.jaypeedigital.com
Harrison’s Principles of Internal Medicine – Hypertension
https://accessmedicine.mhmedical.com