Table of Contents
Introduction
Noradrenaline (norepinephrine) is an endogenous catecholamine that functions as both a neurotransmitter and a hormone. It is widely used clinically as a vasopressor in conditions such as septic shock and acute hypotension. Noradrenaline primarily acts on α-adrenergic receptors with additional β1 receptor activity, leading to potent vasoconstriction and increased blood pressure.
Mechanism of Action (Step-wise)
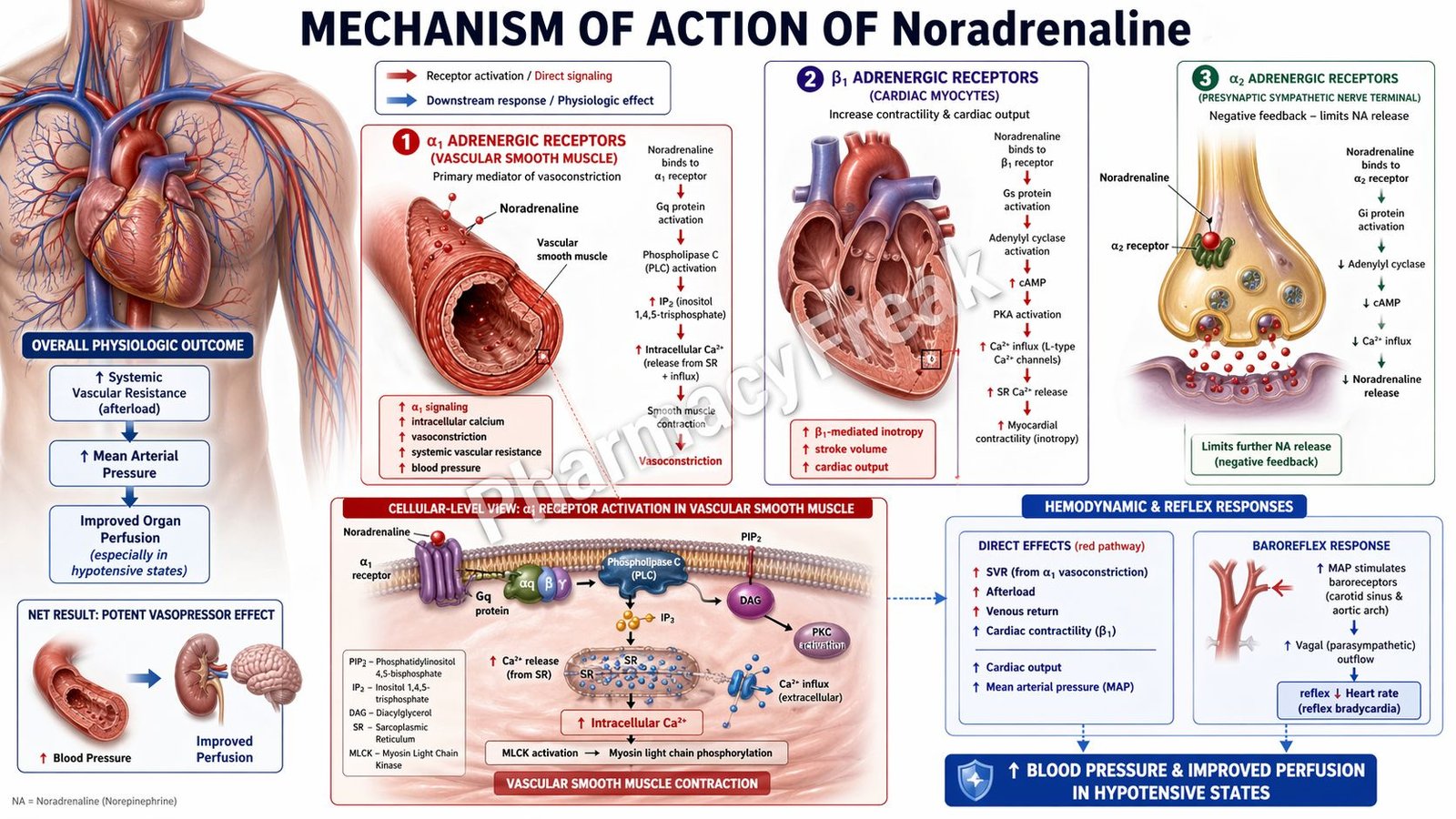
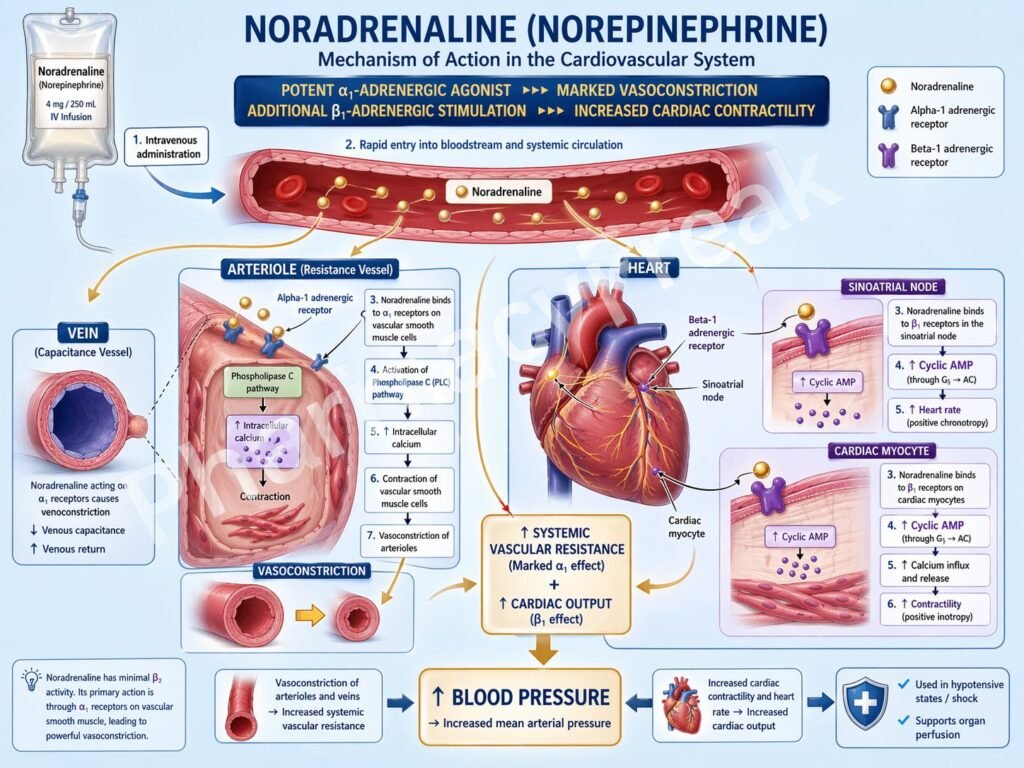
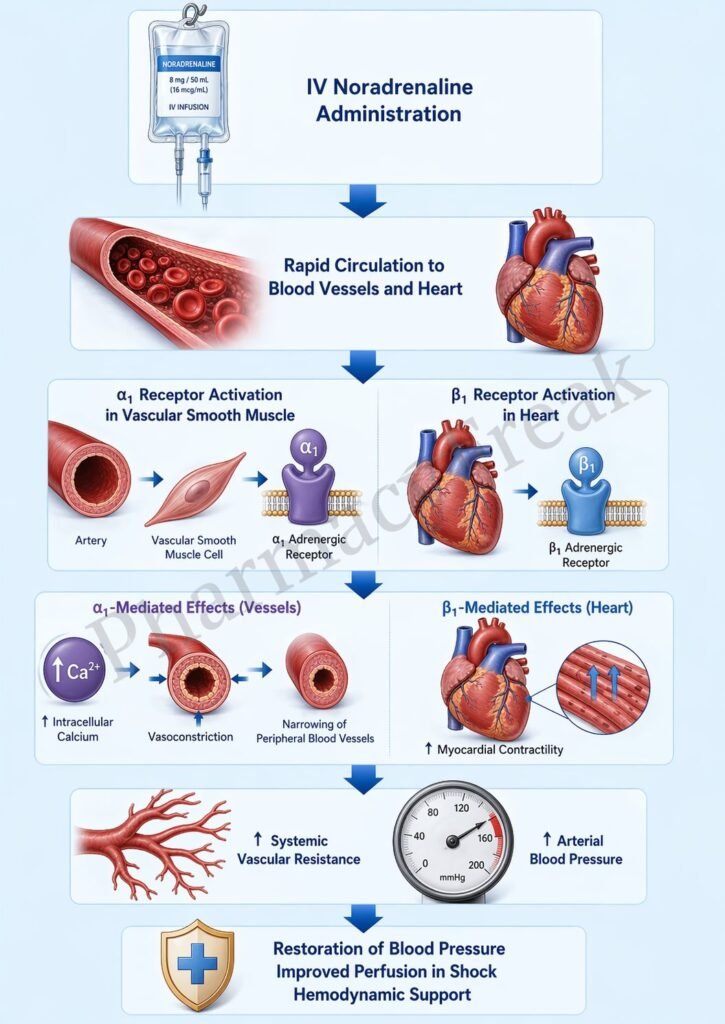
- Noradrenaline binds to α1-adrenergic receptors on vascular smooth muscle.
- These receptors are coupled to Gq proteins.
- Activation of Gq stimulates phospholipase C (PLC).
- PLC converts PIP2 into IP3 and DAG.
- IP3 increases intracellular calcium release from the sarcoplasmic reticulum.
- Increased calcium leads to smooth muscle contraction.
- This causes vasoconstriction of arterioles and veins.
- Vasoconstriction increases systemic vascular resistance (SVR).
- Noradrenaline also stimulates β1-adrenergic receptors in the heart.
- β1 receptor activation increases cAMP via Gs protein activation.
- Increased cAMP enhances calcium influx in cardiac cells.
- This increases myocardial contractility (positive inotropic effect).
- Reflex vagal stimulation may reduce heart rate (reflex bradycardia).
- The overall effect is a marked increase in blood pressure.
A key exam point is that noradrenaline primarily acts on α1 receptors causing vasoconstriction, with additional β1-mediated cardiac effects.
Pharmacokinetics
Noradrenaline is administered intravenously due to rapid metabolism and poor oral bioavailability. It has a very short half-life because it is rapidly metabolized by monoamine oxidase (MAO) and catechol-O-methyltransferase (COMT). It is inactivated in the liver and other tissues, and metabolites are excreted in urine.
Clinical Uses
Noradrenaline is used as a first-line vasopressor in septic shock to restore blood pressure. It is also used in acute hypotension and during anesthesia-related hypotensive states. Its potent vasoconstrictive action makes it effective in maintaining organ perfusion in critically ill patients.
Adverse Effects
Common adverse effects include hypertension, arrhythmias, and tissue ischemia due to excessive vasoconstriction. Extravasation can cause local tissue necrosis. Reflex bradycardia may occur due to increased blood pressure. Careful monitoring is essential during administration.
Comparative Analysis
| Feature | Noradrenaline | Adrenaline | Dopamine |
|---|---|---|---|
| Receptor activity | α1, β1 | α1, β1, β2 | D1, β1, α1 (dose-dependent) |
| Vasoconstriction | Strong | Moderate | Variable |
| Cardiac effect | Moderate ↑ contractility | Strong ↑ HR and contractility | Dose-dependent |
| Effect on BP | Marked increase | Increase | Variable |
| Use | Septic shock | Anaphylaxis, cardiac arrest | Shock, HF |
| Reflex bradycardia | Common | Less common | Rare |
Noradrenaline differs from adrenaline by lacking significant β2 activity, resulting in stronger vasoconstriction and less bronchodilation. Compared to dopamine, its effects are more predictable and primarily vasoconstrictive.
MCQs
- Noradrenaline primarily acts on which receptor?
a) β2 receptor
b) α1 receptor
c) Dopamine receptor
d) Histamine receptor
Answer: b) α1 receptor
- α1 receptor activation leads to:
a) cAMP increase
b) IP3 and DAG formation
c) Sodium influx
d) Potassium efflux
Answer: b) IP3 and DAG formation
- IP3 increases:
a) Sodium
b) Calcium
c) Potassium
d) Chloride
Answer: b) Calcium
- Noradrenaline causes:
a) Vasodilation
b) Vasoconstriction
c) No vascular effect
d) Capillary leakage
Answer: b) Vasoconstriction
- β1 receptor activation increases:
a) cGMP
b) cAMP
c) ATP
d) ADP
Answer: b) cAMP
- Noradrenaline is used in:
a) Asthma
b) Septic shock
c) Diabetes
d) Anemia
Answer: b) Septic shock
- A common cardiac effect is:
a) Decreased contractility
b) Increased contractility
c) No change
d) Decreased calcium
Answer: b) Increased contractility
- Reflex bradycardia occurs due to:
a) Direct β2 stimulation
b) Increased blood pressure
c) Decreased calcium
d) Sodium influx
Answer: b) Increased blood pressure
- Noradrenaline is administered:
a) Orally
b) Intravenously
c) Intramuscularly
d) Sublingually
Answer: b) Intravenously
- Noradrenaline is metabolized by:
a) CYP enzymes
b) MAO and COMT
c) Renal enzymes
d) Pancreatic enzymes
Answer: b) MAO and COMT
- Extravasation of noradrenaline may cause:
a) Edema
b) Tissue necrosis
c) Hyperglycemia
d) Hypocalcemia
Answer: b) Tissue necrosis
- Compared to adrenaline, noradrenaline has:
a) More β2 activity
b) Less β2 activity
c) Same effect
d) No effect
Answer: b) Less β2 activity
FAQs
What is the mechanism of action of noradrenaline?
It stimulates α1 receptors causing vasoconstriction and β1 receptors increasing cardiac contractility.
Why does noradrenaline cause reflex bradycardia?
Due to increased blood pressure activating baroreceptors.
What is its primary clinical use?
Septic shock and acute hypotension.
How is noradrenaline administered?
Intravenously due to rapid metabolism.
What is a serious adverse effect?
Tissue necrosis from extravasation.
How does it differ from adrenaline?
It has minimal β2 activity and stronger vasoconstriction.
References
Goodman & Gilman’s The Pharmacological Basis of Therapeutics – Adrenergic Drugs
https://accessmedicine.mhmedical.com/book.aspx?bookid=3191
Katzung: Basic and Clinical Pharmacology – Sympathomimetics
https://accessmedicine.mhmedical.com/content.aspx?bookid=3382
Tripathi: Essentials of Medical Pharmacology – Adrenergic Drugs
https://www.jaypeedigital.com
Harrison’s Principles of Internal Medicine – Shock
https://accessmedicine.mhmedical.com