Table of Contents
Introduction
Ipratropium bromide is a short-acting anticholinergic (antimuscarinic) bronchodilator primarily used in the management of chronic obstructive pulmonary disease (COPD) and, in some cases, asthma. It is a quaternary ammonium compound derived from atropine, designed for inhalational use with minimal systemic absorption. Its main action is to reduce bronchoconstriction mediated by the parasympathetic nervous system.
Mechanism of Action (Step-wise)
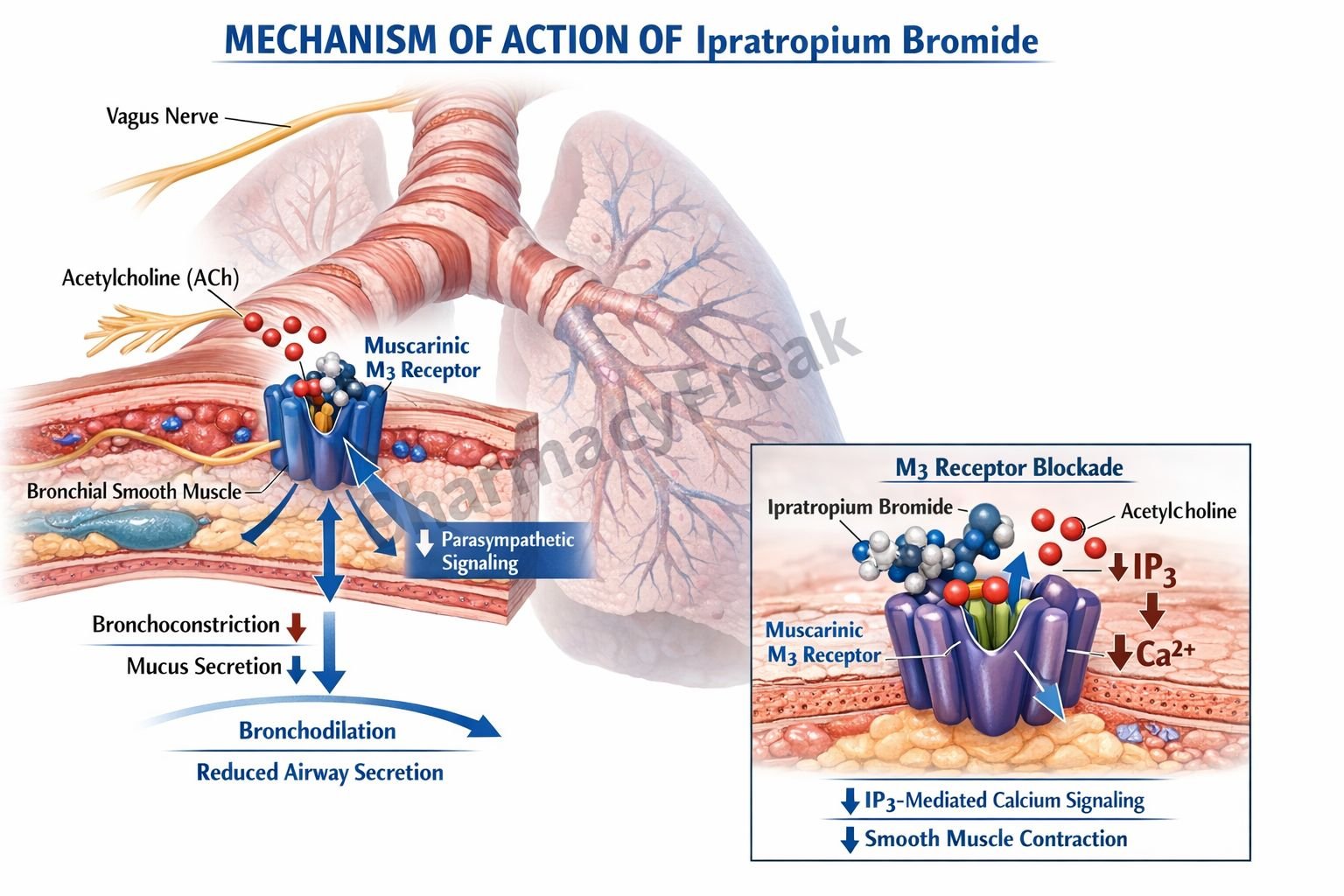
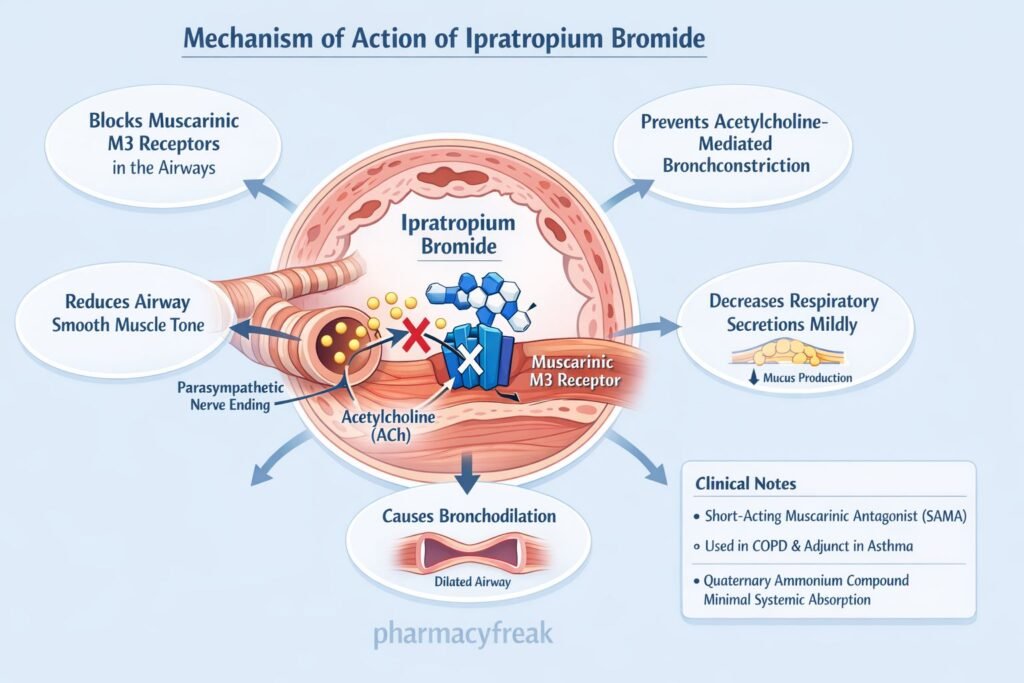
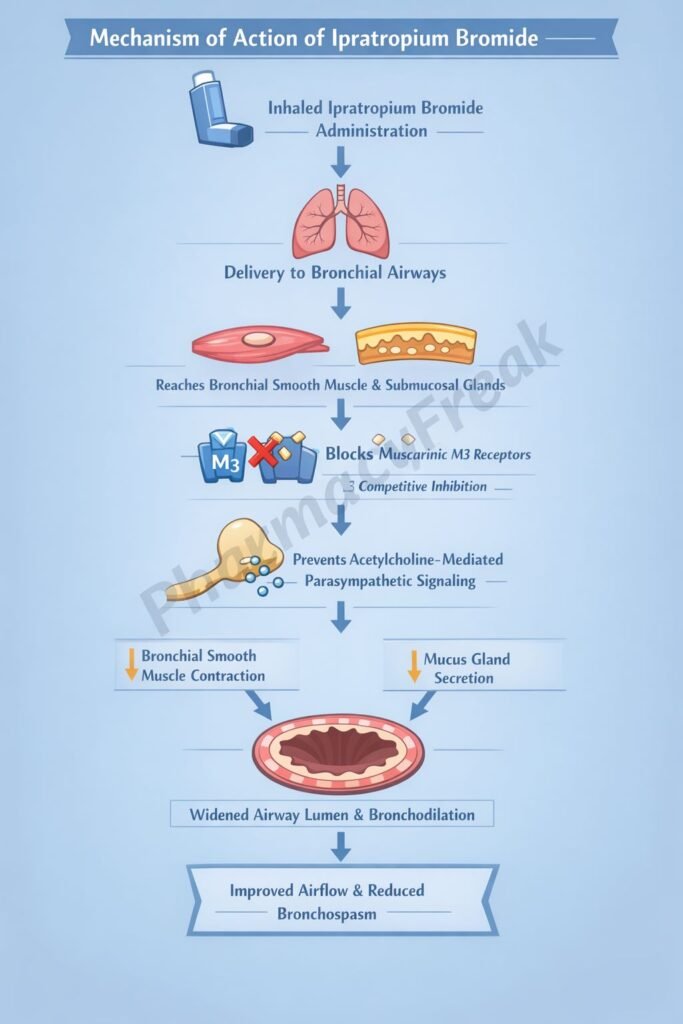
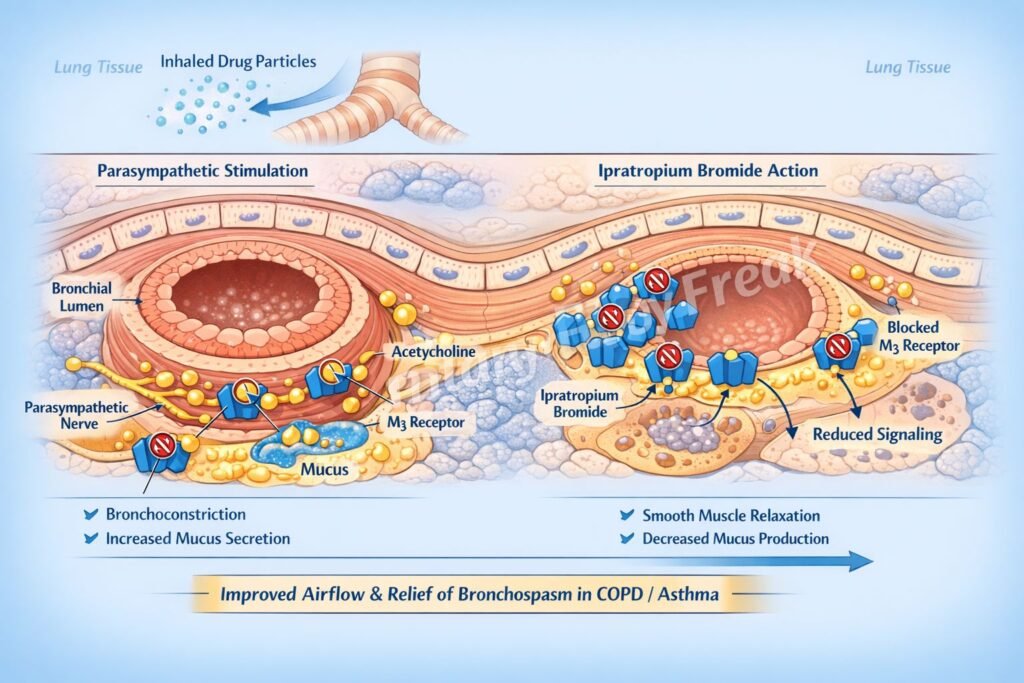
- Blockade of Muscarinic Receptors (M3)
Ipratropium competitively inhibits muscarinic M3 receptors on bronchial smooth muscle. - Inhibition of Parasympathetic Activity
Normally, acetylcholine released from vagal nerve endings binds to M3 receptors causing bronchoconstriction. Ipratropium blocks this action. - Bronchodilation
By preventing acetylcholine-mediated contraction, it leads to relaxation of bronchial smooth muscle and airway dilation. - Reduction of Airway Secretions
It inhibits muscarinic receptors in submucosal glands, decreasing mucus secretion. - Minimal Systemic Effects
Due to its quaternary structure, it poorly crosses lipid membranes, limiting systemic absorption and CNS effects. - Local Action in Airways
Its effect is mainly localized to the respiratory tract when administered via inhalation.
Pharmacokinetics
- Route: Inhalation
- Absorption: Minimal systemic absorption
- Onset of action: 15–30 minutes
- Duration of action: 4–6 hours
- Distribution: Limited CNS penetration
- Excretion: Primarily renal
Clinical Uses
- Chronic obstructive pulmonary disease (COPD)
- Adjunct therapy in asthma
- Acute bronchospasm (in combination with beta-agonists)
- Allergic and non-allergic rhinitis (nasal formulation)
Adverse Effects
- Dry mouth
- Throat irritation
- Cough
- Blurred vision (if aerosol contacts eyes)
- Rare systemic anticholinergic effects
Comparative Analysis
| Feature | Ipratropium | Tiotropium | Salbutamol |
|---|---|---|---|
| Class | SAMA | LAMA | SABA |
| Mechanism | M3 receptor blockade | M3 selective blockade (long-acting) | β2 agonist |
| Onset | Slow | Slow | Rapid |
| Duration | 4–6 hours | >24 hours | 4–6 hours |
| Use | COPD, adjunct asthma | Maintenance COPD | Acute asthma relief |
| CNS effects | Minimal | Minimal | None |
Ipratropium is a short-acting muscarinic antagonist (SAMA) used mainly for symptom control in COPD. Compared to tiotropium, it has a shorter duration of action. Unlike salbutamol, which acts via β2 receptor stimulation, ipratropium works by blocking cholinergic bronchoconstriction.
MCQs
- Ipratropium primarily blocks which receptor?
a) β2 receptor
b) M3 receptor
c) H1 receptor
d) α1 receptor
Answer: b) M3 receptor - Main effect of ipratropium:
a) Bronchoconstriction
b) Bronchodilation
c) Vasoconstriction
d) Sedation
Answer: b) Bronchodilation - Ipratropium is classified as:
a) β2 agonist
b) Anticholinergic
c) Steroid
d) Antibiotic
Answer: b) Anticholinergic - Route of administration:
a) Oral
b) IV
c) Inhalation
d) IM
Answer: c) Inhalation - Duration of action:
a) 1 hour
b) 2 hours
c) 4–6 hours
d) 24 hours
Answer: c) 4–6 hours - Compared to atropine, ipratropium:
a) Crosses BBB easily
b) Has more CNS effects
c) Has minimal systemic effects
d) Is more toxic
Answer: c) Has minimal systemic effects - Used primarily in:
a) Hypertension
b) COPD
c) Diabetes
d) Epilepsy
Answer: b) COPD - Side effect commonly seen:
a) Diarrhea
b) Dry mouth
c) Hypoglycemia
d) Rash
Answer: b) Dry mouth - Ipratropium reduces:
a) Bronchial tone
b) Heart rate
c) Blood glucose
d) Platelets
Answer: a) Bronchial tone - Combination therapy often includes:
a) ACE inhibitors
b) β2 agonists
c) Diuretics
d) Anticoagulants
Answer: b) β2 agonists
FAQs
- What is the mechanism of action of ipratropium bromide?
It blocks M3 muscarinic receptors, preventing acetylcholine-induced bronchoconstriction. - Why is ipratropium preferred for COPD?
It reduces vagal-mediated bronchoconstriction, which is prominent in COPD. - Does ipratropium act quickly?
It has a slower onset compared to β2 agonists. - Can ipratropium cross the blood-brain barrier?
No, due to its quaternary ammonium structure. - What is the difference between ipratropium and tiotropium?
Tiotropium is long-acting, while ipratropium is short-acting. - Can it be used in asthma?
Yes, as an adjunct therapy.