Table of Contents
Introduction
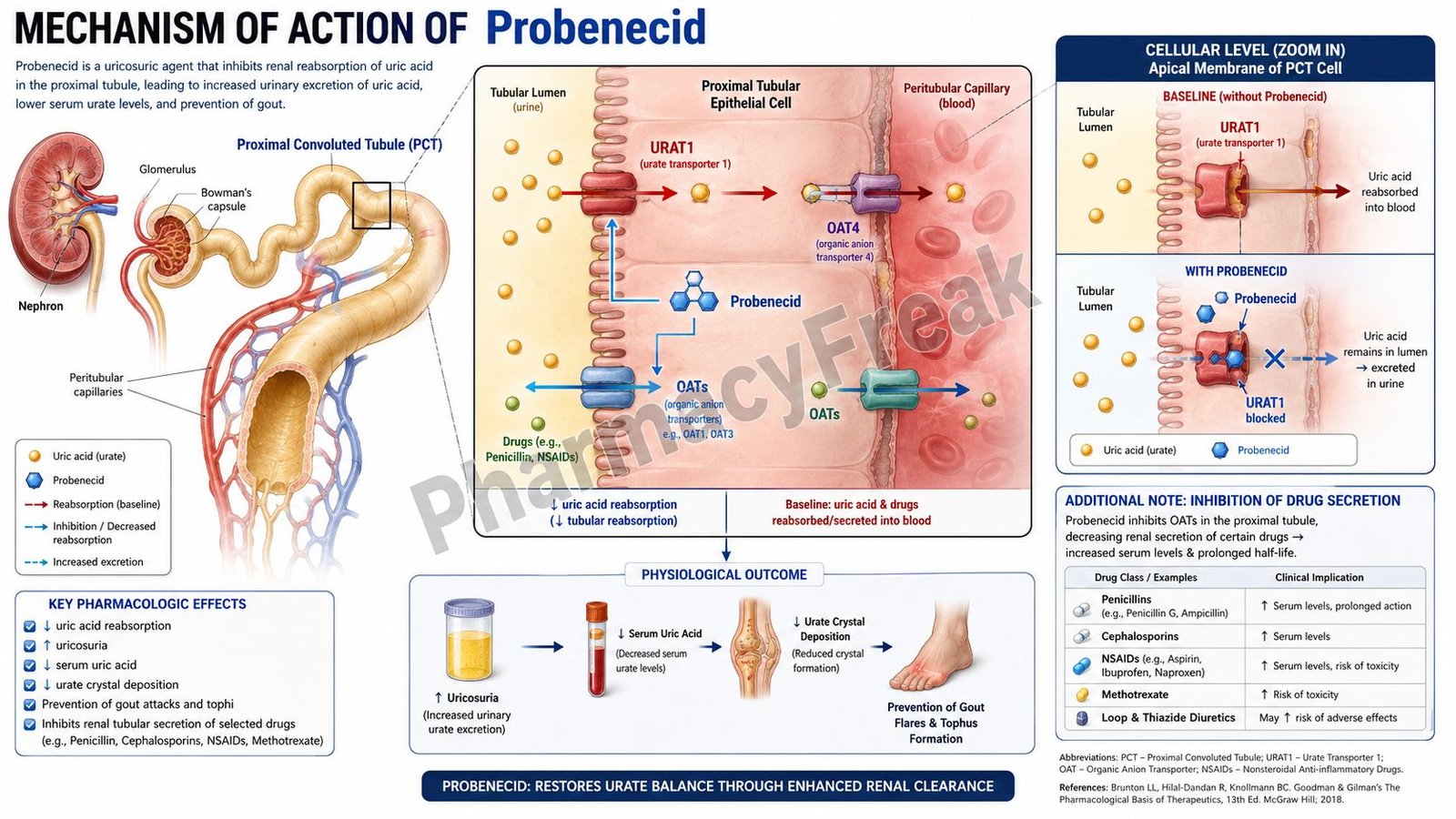
Probenecid is a uricosuric drug used primarily in the treatment of chronic gout and hyperuricemia. It lowers serum uric acid levels by increasing renal excretion of uric acid. Probenecid also affects renal tubular transport of various drugs, including penicillins, by inhibiting organic anion transporters in the kidney.
Mechanism of Action (Step-wise)
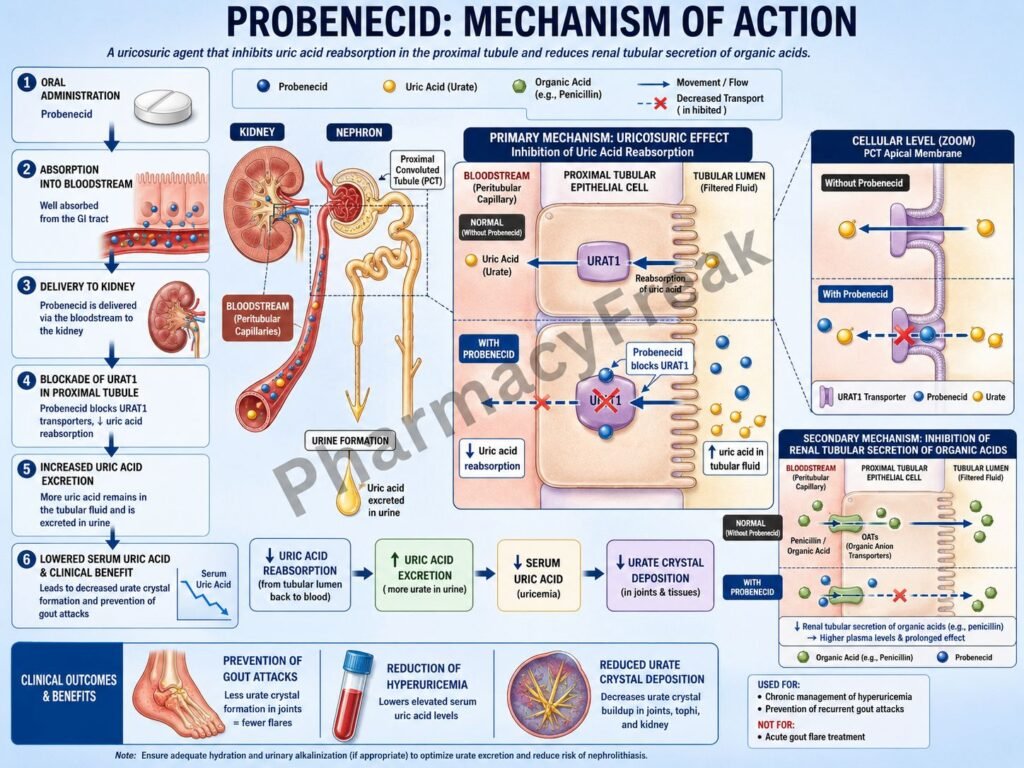
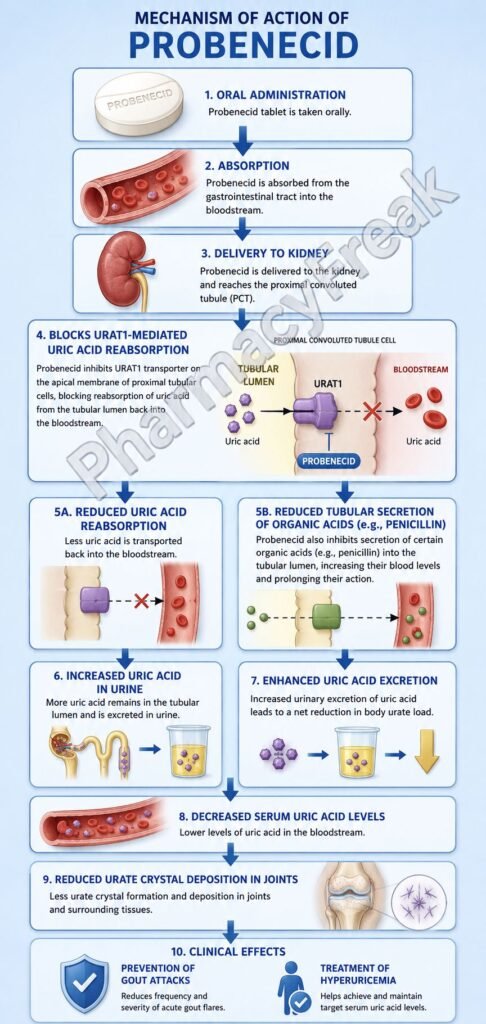
- Probenecid acts mainly in the proximal convoluted tubule of the nephron.
- It inhibits urate transporter 1 (URAT1) located on the apical membrane of proximal tubular cells.
- URAT1 normally reabsorbs filtered uric acid from the tubular lumen back into the bloodstream.
- Inhibition of URAT1 decreases uric acid reabsorption.
- This increases urinary excretion of uric acid (uricosuria).
- Increased uric acid excretion lowers serum urate concentration.
- Reduced serum uric acid decreases urate crystal deposition in joints and tissues.
- Probenecid also inhibits organic anion transporters (OATs).
- OAT inhibition decreases renal tubular secretion of certain drugs such as penicillin.
- This prolongs plasma concentrations of affected drugs.
- The overall effect is reduced hyperuricemia and increased uric acid elimination.
A key exam point is that probenecid inhibits URAT1 in the proximal tubule to increase uric acid excretion.
Pharmacokinetics
Probenecid is administered orally and is well absorbed. It is highly protein bound and undergoes hepatic metabolism. The drug and its metabolites are excreted mainly through the kidneys. Adequate renal function is necessary for effectiveness because the drug depends on renal uric acid excretion.
Clinical Uses
Probenecid is used in chronic gout and hyperuricemia associated with urate overproduction or underexcretion. It may also be used to prolong plasma concentrations of penicillin and certain antibiotics by reducing renal tubular secretion.
Adverse Effects
Common adverse effects include gastrointestinal irritation, rash, and headache. Increased urinary uric acid can lead to uric acid kidney stones. Adequate hydration is important during therapy. It is not recommended during acute gout attacks or severe renal impairment.
Comparative Analysis
| Feature | Probenecid | Allopurinol | Febuxostat |
|---|---|---|---|
| Main mechanism | ↑ Uric acid excretion | Xanthine oxidase inhibition | Xanthine oxidase inhibition |
| Site of action | Renal proximal tubule | Purine metabolism | Purine metabolism |
| Effect on uric acid | Uricosuric | ↓ Production | ↓ Production |
| Use | Chronic gout | Chronic gout | Chronic gout |
| Kidney stone risk | Increased | Lower | Lower |
| Renal function requirement | Good renal function needed | Can be used cautiously | Can be used cautiously |
Probenecid differs from allopurinol and febuxostat because it increases uric acid excretion rather than decreasing uric acid production. It is most effective in patients with underexcretion of uric acid.
MCQs
- Probenecid primarily acts in the:
a) Loop of Henle
b) Proximal convoluted tubule
c) Distal tubule
d) Collecting duct
Answer: b) Proximal convoluted tubule
- Probenecid inhibits which transporter?
a) ENaC
b) URAT1
c) Na⁺/K⁺ ATPase
d) GLUT4
Answer: b) URAT1
- URAT1 normally:
a) Secretes sodium
b) Reabsorbs uric acid
c) Produces uric acid
d) Filters glucose
Answer: b) Reabsorbs uric acid
- Probenecid increases:
a) Uric acid reabsorption
b) Uric acid excretion
c) Calcium excretion only
d) Glucose reabsorption
Answer: b) Uric acid excretion
- Probenecid lowers:
a) Serum uric acid
b) Blood glucose
c) Serum calcium
d) Sodium levels
Answer: a) Serum uric acid
- Probenecid is mainly used in:
a) Asthma
b) Chronic gout
c) Diabetes mellitus
d) Heart failure
Answer: b) Chronic gout
- Probenecid also inhibits:
a) Histamine receptors
b) Organic anion transporters
c) Dopamine receptors
d) Calcium channels
Answer: b) Organic anion transporters
- OAT inhibition by probenecid can prolong action of:
a) Insulin
b) Penicillin
c) Digoxin
d) Warfarin only
Answer: b) Penicillin
- A major complication of therapy is:
a) Hyperglycemia
b) Kidney stones
c) Bradycardia
d) Hypercalcemia
Answer: b) Kidney stones
- Adequate hydration is important to prevent:
a) Hypertension
b) Uric acid stones
c) Hypoglycemia
d) Hypernatremia
Answer: b) Uric acid stones
- Compared with allopurinol, probenecid:
a) Decreases uric acid production
b) Increases uric acid excretion
c) Blocks xanthine oxidase
d) Inhibits cyclooxygenase
Answer: b) Increases uric acid excretion
- Probenecid effectiveness requires:
a) Severe renal failure
b) Adequate renal function
c) Liver failure
d) Hypercalcemia
Answer: b) Adequate renal function
FAQs
What is the mechanism of action of probenecid?
It inhibits URAT1 in the proximal tubule, increasing uric acid excretion.
Why is probenecid called a uricosuric drug?
Because it increases urinary excretion of uric acid.
What is its main clinical use?
Chronic gout and hyperuricemia.
Why should hydration be maintained during therapy?
To reduce the risk of uric acid kidney stones.
How does probenecid affect penicillin?
It decreases renal tubular secretion, prolonging penicillin levels.
How does probenecid differ from allopurinol?
Probenecid increases uric acid excretion, while allopurinol decreases uric acid production.
References
Goodman & Gilman’s The Pharmacological Basis of Therapeutics – Drugs Used in Gout
https://accessmedicine.mhmedical.com/book.aspx?bookid=3191
Katzung: Basic and Clinical Pharmacology – Antigout Drugs
https://accessmedicine.mhmedical.com/content.aspx?bookid=3382
Tripathi: Essentials of Medical Pharmacology – Antigout Drugs
https://www.jaypeedigital.com
Harrison’s Principles of Internal Medicine – Gout and Hyperuricemia
https://accessmedicine.mhmedical.com