Table of Contents
Introduction
Phenytoin is a first-generation anticonvulsant and hydantoin derivative widely utilized for the management of generalized tonic-clonic seizures, complex partial seizures, and status epilepticus. It also has historical use in certain cardiac arrhythmias. Known for its narrow therapeutic index, phenytoin requires careful dosing and monitoring, yet remains a mainstay in epilepsy therapy due to its efficacy and long-standing clinical experience.
Mechanism of Action (Step-wise)
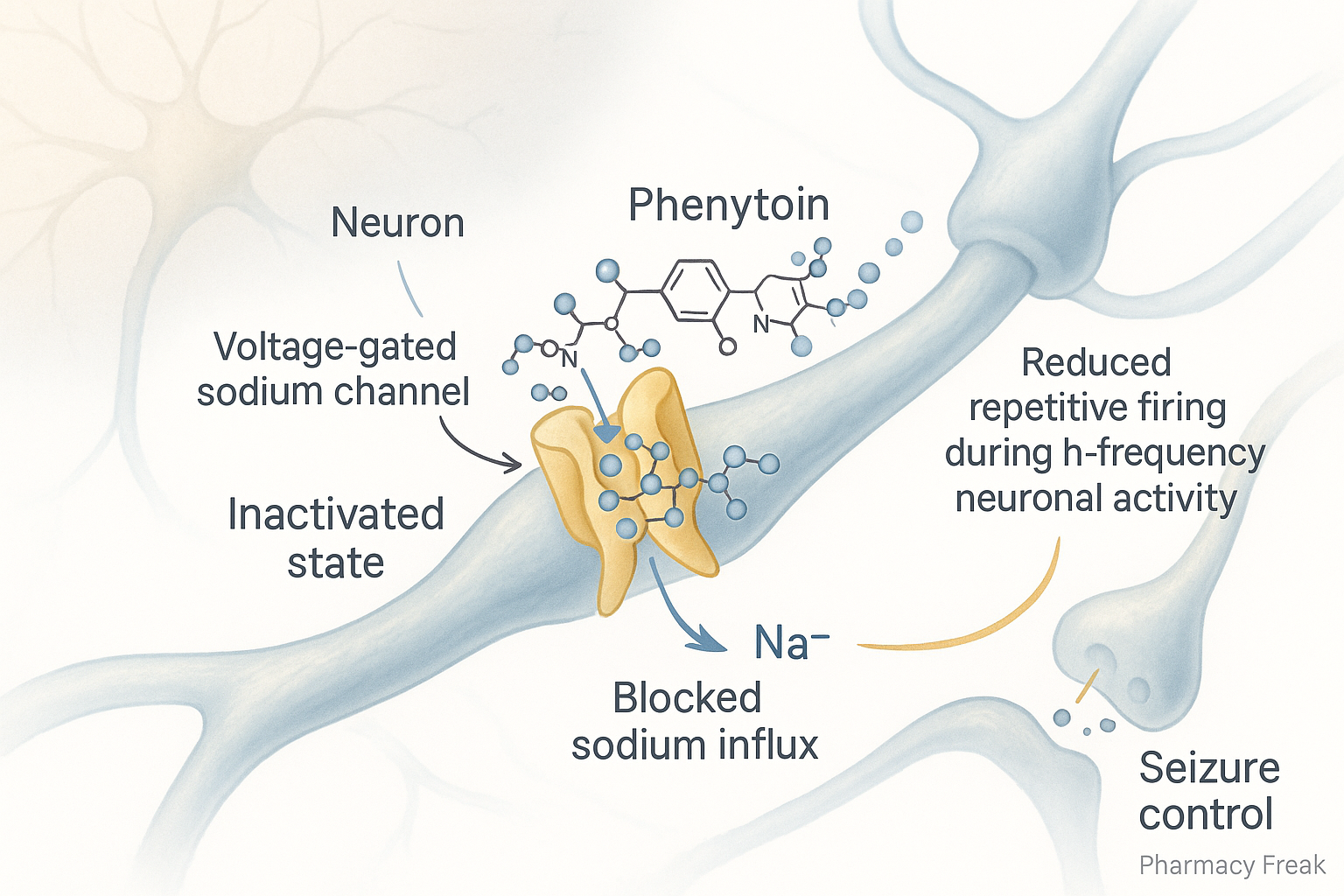
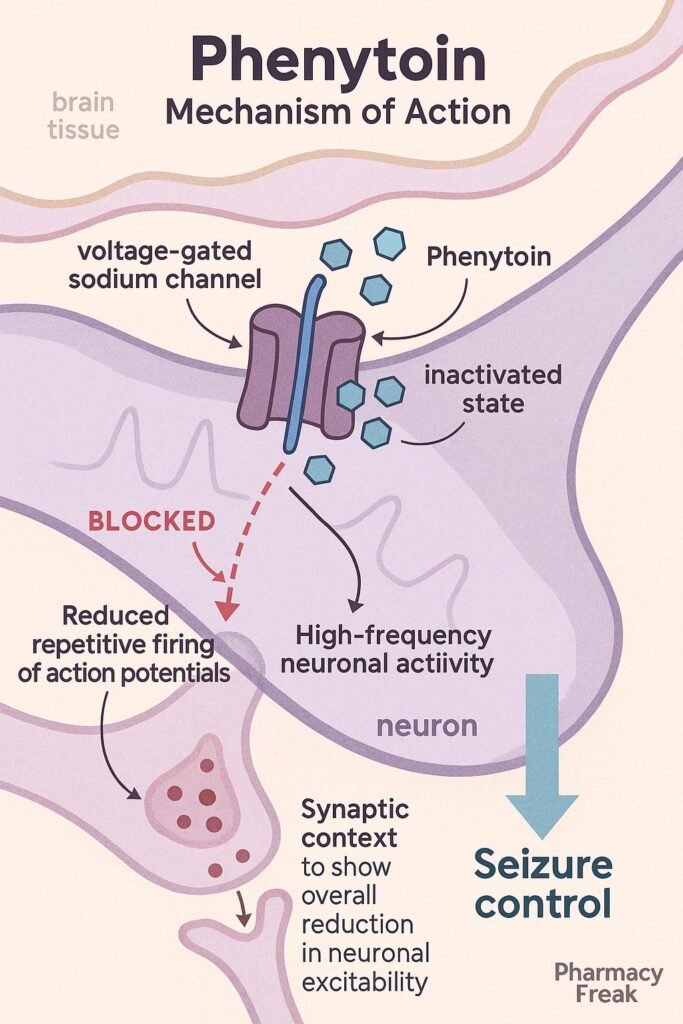
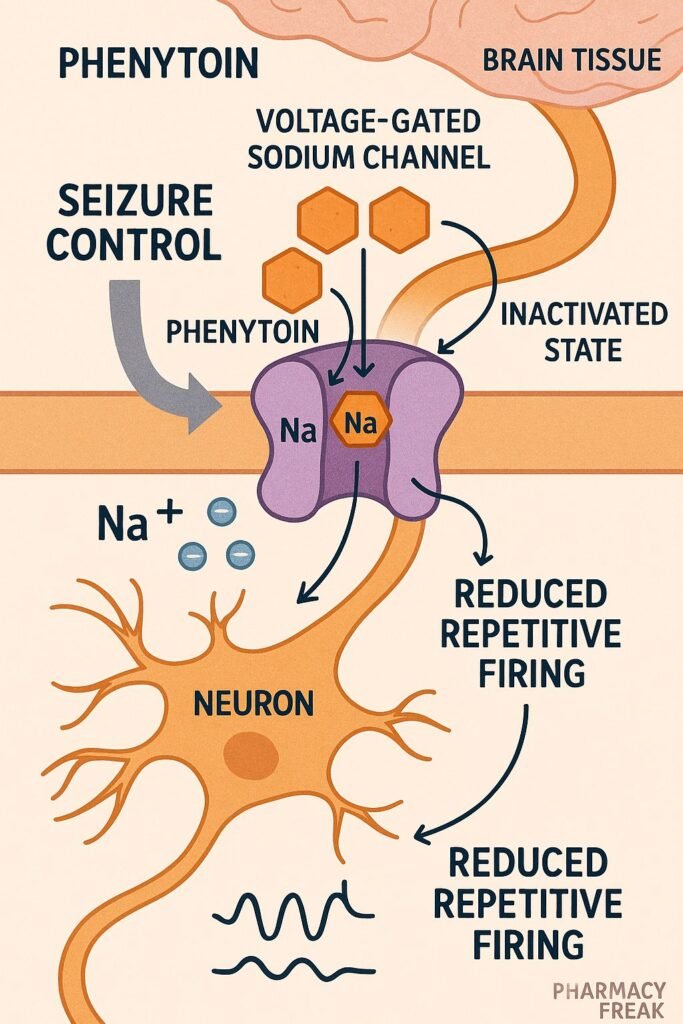
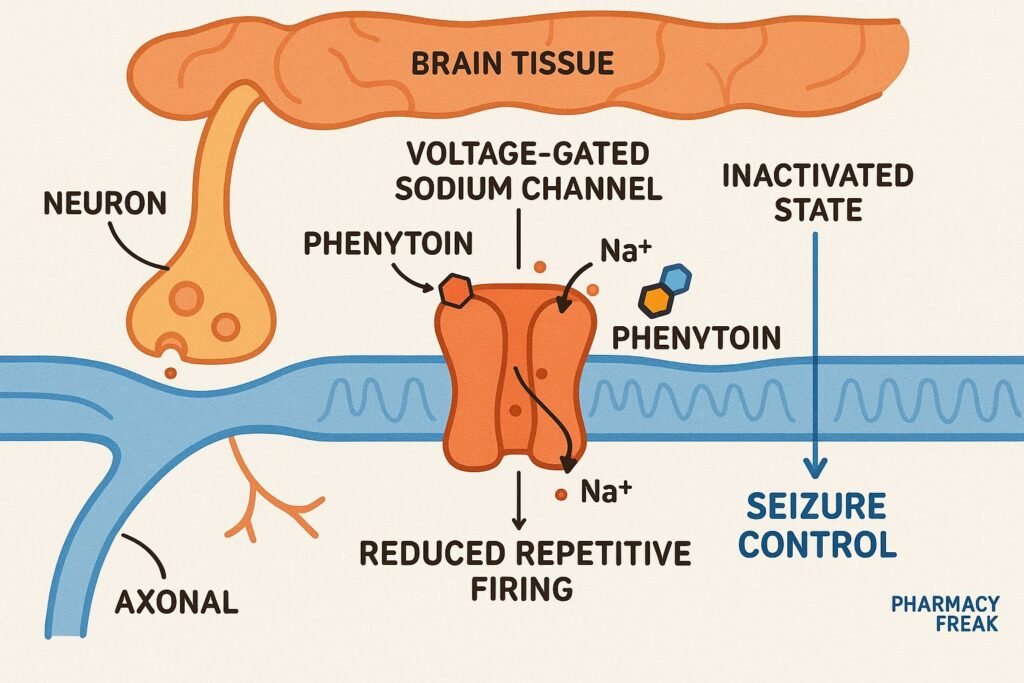
1. Voltage-Gated Sodium Channel Blockade
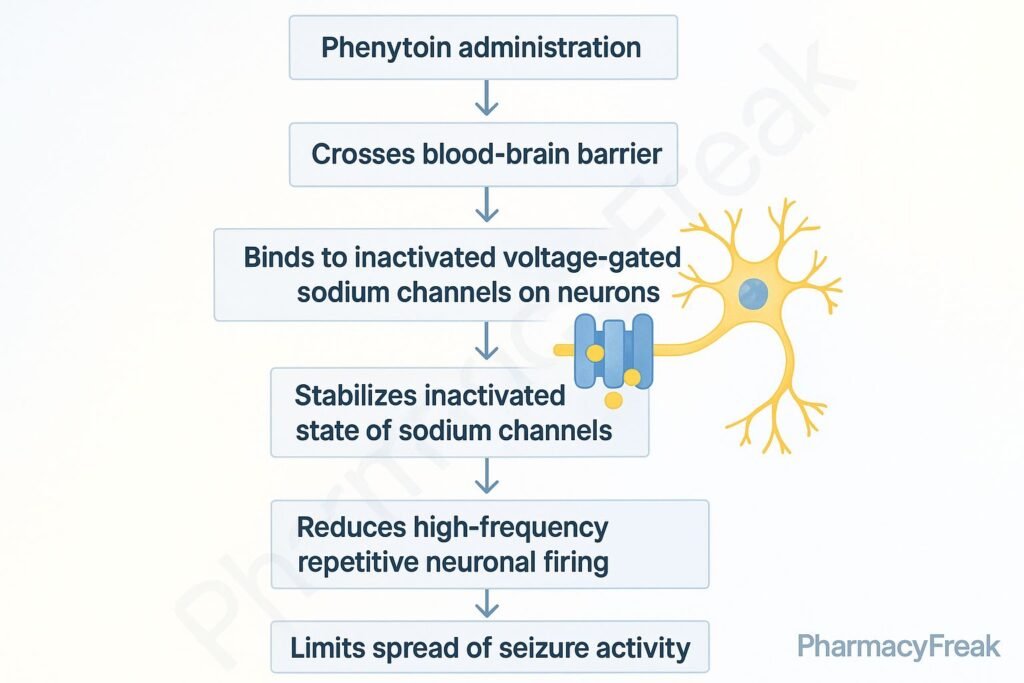
Phenytoin stabilizes the inactive state of voltage-gated sodium channels in neuronal membranes, thereby preventing repetitive high-frequency firing—a common feature in seizure activity.
2. Prolongation of Refractory Period
By slowing recovery from inactivation, phenytoin extends the refractory period of neurons, limiting their ability to fire again immediately. This interrupts seizure propagation across neural circuits.
3. Selective Action in Motor Cortex and Brainstem
Phenytoin demonstrates its anticonvulsant effects predominantly in the motor cortex—curbing spread of focal seizure activity—and in brainstem centers responsible for seizure generalization.
4. Minimal Calcium Channel and Secondary Messenger Modulation
At higher concentrations, phenytoin may inhibit L-type calcium channels and affect various signal transduction pathways, but these actions are secondary and less clinically significant.

Pharmacokinetics
- Absorption: Oral bioavailability ranges from 70% to 100%, with peak levels between 4–12 hours.
- Distribution: Phenytoin is highly protein-bound (approximately 90–95%), with the free fraction being pharmacologically active.
- Metabolism: Primarily hepatic via CYP2C9 and CYP2C19. Exhibits mixed-order elimination—initially first-order at low concentrations, shifting to zero-order as metabolic pathways saturate.
- Half-life: Approximately 10–22 hours, but may significantly prolong at higher concentrations or with saturation.
- Excretion: Approximately 1–5% excreted unchanged in urine; the rest is metabolized.
Clinical Uses
- Generalized tonic-clonic seizures
- Complex partial seizures
- Status epilepticus (via intravenous fosphenytoin, a prodrug)
- Historical or occasional use in certain arrhythmias
Adverse Effects
- Neurological: Ataxia, nystagmus, dizziness, cerebellar degeneration with long-term use
- Gingival Hyperplasia and Hirsutism
- Bone Effects: Osteoporosis via vitamin D metabolism
- Dermatologic: Rash, Stevens–Johnson syndrome, toxic epidermal necrolysis
- Hematologic: Megaloblastic anemia, agranulocytosis
- Cardiovascular: Purple glove syndrome following IV use
Comparative Analysis
| Feature | Phenytoin | Newer AEDs (e.g., Lamotrigine) |
|---|---|---|
| Mechanism | Use-dependent Na⁺ channel blockade | Multi-mechanistic |
| Elimination Kinetics | Mixed-order (nonlinear) | Linear metabolism |
| Therapeutic Monitoring | Required | Often not required |
| Side Effects | Frequent and serious | Generally more tolerable |
| Drug Interactions | High (enzyme induction) | Variable |
Multiple Choice Questions (MCQs)
1. Phenytoin primarily acts by inhibiting which channel?
a) Calcium channel
b) Potassium channel
c) Voltage-gated sodium channel
d) GABA receptor
Answer: c) Voltage-gated sodium channel
2. Phenytoin prolongs which neuronal period?
a) Depolarization
b) Refractory period
c) Repolarization
d) Plateau phase
Answer: b) Refractory period
3. What is the pharmacokinetic elimination characteristic of phenytoin at high doses?
a) First-order kinetics
b) Zero-order kinetics
c) Mixed-order kinetics
d) Non-linear receptor-mediated clearance
Answer: c) Mixed-order kinetics
4. Which enzyme primarily metabolizes phenytoin?
a) CYP3A4
b) CYP2D6
c) CYP2C9
d) CYP1A2
Answer: c) CYP2C9
5. Which adverse effect is characteristic of long-term phenytoin use?
a) Tremor only
b) Gingival hyperplasia
c) Sedation
d) Hypertension
Answer: b) Gingival hyperplasia
FAQs
Q1. Does phenytoin require blood level monitoring?
Yes, due to its narrow therapeutic index and nonlinear pharmacokinetics.
Q2. Is phenytoin safe in pregnancy?
It has significant teratogenic risk but may still be used if seizure control outweighs risks.
Q3. Why does small dose increases cause disproportionate serum level rises?
Because of saturation of metabolic enzymes, shifting elimination from first-order to zero-order.
References
- Goodman & Gilman’s The Pharmacological Basis of Therapeutics, 12th Edition
- KD Tripathi, Essentials of Medical Pharmacology, 7th Edition
- Standard Antiepileptic Drug Guidelines
- Clinical Pharmacokinetics of Anticonvulsants
- FDA Drug Monograph for Phenytoin