Table of Contents
Introduction
Lidocaine is a widely used local anesthetic and class IB antiarrhythmic drug. It is commonly used for local and regional anesthesia as well as in the management of ventricular arrhythmias. Lidocaine works by blocking nerve conduction and stabilizing cardiac membranes.
Mechanism of Action (Step-wise)
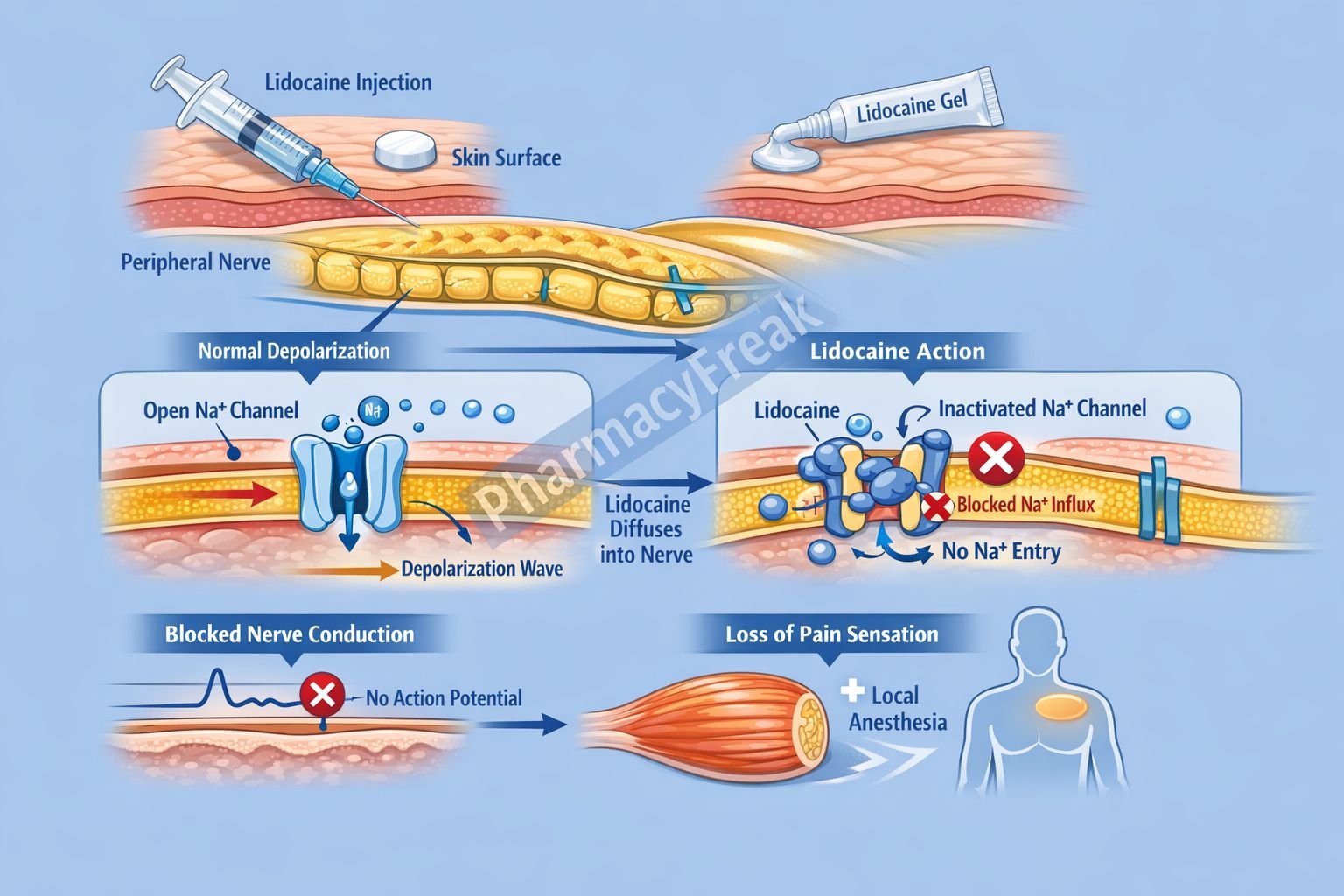
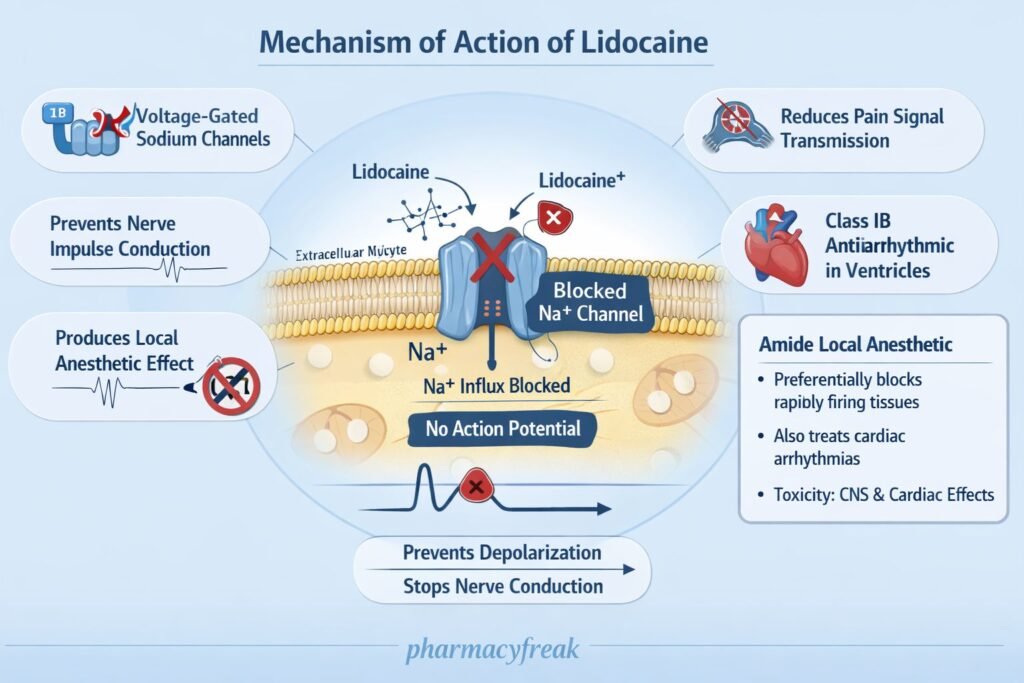
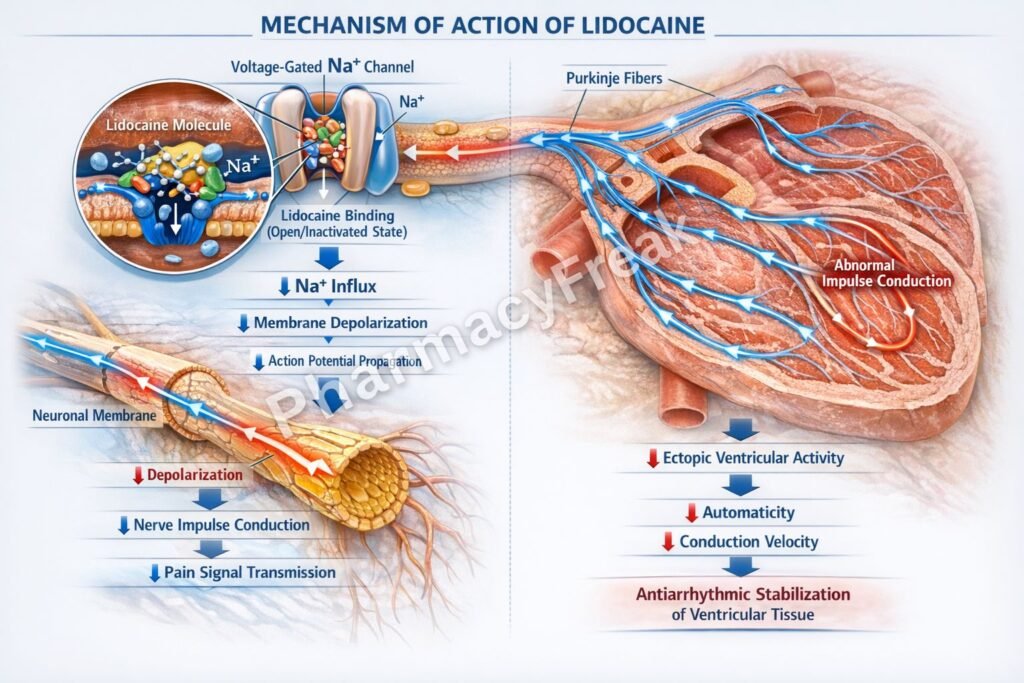
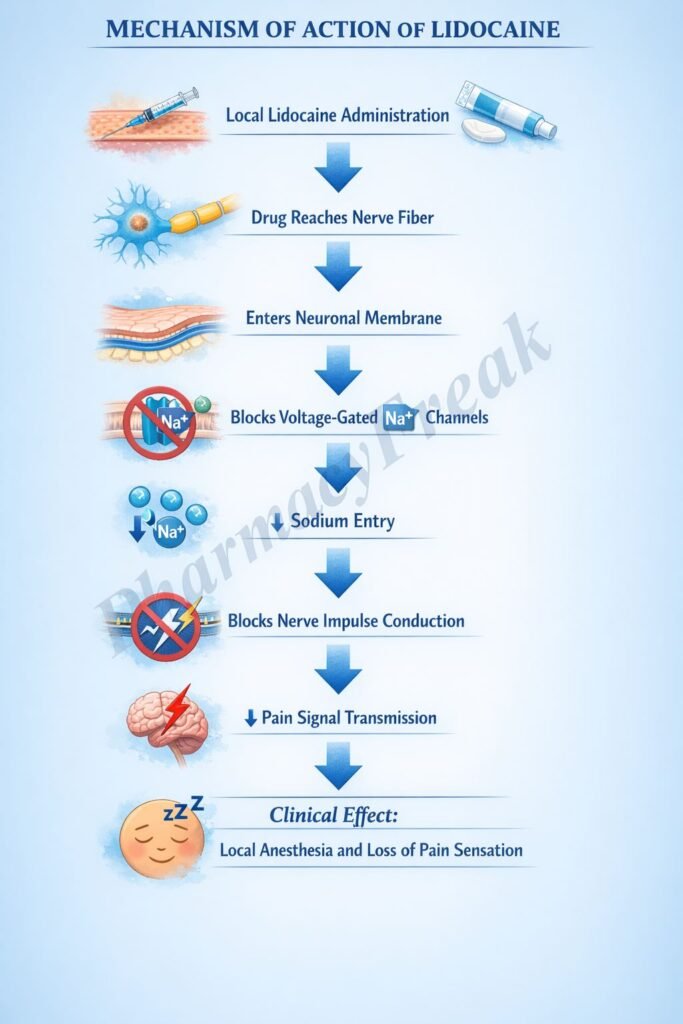
- Blockade of Voltage-Gated Sodium Channels (Na⁺ Channels)
Lidocaine binds to and blocks voltage-gated sodium channels in neuronal and cardiac cell membranes. - Preferential Binding to Active and Inactivated States
It has higher affinity for sodium channels in their open and inactivated states, especially in rapidly firing cells. - Inhibition of Sodium Influx
Blocking Na⁺ channels prevents sodium entry during depolarization. - Prevention of Action Potential Generation
This inhibits initiation and propagation of action potentials in nerve fibers. - Local Anesthetic Effect
Loss of nerve conduction results in reversible loss of sensation (pain, temperature, touch). - Cardiac Effects (Class IB Antiarrhythmic)
In cardiac tissue, lidocaine shortens action potential duration and suppresses abnormal automaticity, especially in ischemic tissue. - Use-Dependent Blockade
Lidocaine is more effective in rapidly depolarizing or damaged tissues (e.g., arrhythmias).
Pharmacokinetics
- Administration: Topical, infiltration, nerve block, intravenous
- Absorption: Rapid (depends on site)
- Protein Binding: Moderate
- Metabolism: Hepatic (extensive first-pass metabolism)
- Half-life: ~1.5–2 hours
- Excretion: Renal (as metabolites)
Clinical Uses
- Local anesthesia (infiltration, nerve block, epidural)
- Ventricular arrhythmias (especially post-MI)
- Topical anesthesia (e.g., mucosal surfaces)
Adverse Effects
- CNS toxicity (tremors, seizures)
- Drowsiness
- Hypotension
- Bradycardia
- Cardiac depression (at high doses)
Comparative Analysis
| Feature | Lidocaine | Bupivacaine | Procainamide |
|---|---|---|---|
| Class | Local anesthetic, Class IB | Local anesthetic | Class IA antiarrhythmic |
| Duration | Intermediate | Long | Moderate |
| Cardiac use | Yes | No | Yes |
| CNS toxicity | Moderate | High | Moderate |
| Use | Anesthesia, arrhythmias | Long procedures | Arrhythmias |
Lidocaine is preferred for rapid onset anesthesia and ventricular arrhythmias. Compared to bupivacaine, it has a shorter duration but is safer in cardiac use. Unlike procainamide, it specifically targets ischemic cardiac tissue.
MCQs
- Lidocaine primarily blocks:
a) Calcium channels
b) Sodium channels
c) Potassium channels
d) Chloride channels
Answer: b) Sodium channels - Lidocaine belongs to which antiarrhythmic class?
a) Class I
b) Class IB
c) Class II
d) Class III
Answer: b) Class IB - Mechanism involves:
a) Increased Na⁺ influx
b) Decreased Na⁺ influx
c) Increased Ca²⁺ influx
d) Increased K⁺ efflux
Answer: b) Decreased Na⁺ influx - Lidocaine is used in:
a) Hypertension
b) Ventricular arrhythmias
c) Diabetes
d) Asthma
Answer: b) Ventricular arrhythmias - Preferred binding state:
a) Resting
b) Closed
c) Open/inactivated
d) All equally
Answer: c) Open/inactivated - Major toxicity:
a) Hepatotoxicity
b) CNS toxicity
c) Nephrotoxicity
d) Ototoxicity
Answer: b) CNS toxicity - Lidocaine shortens:
a) QT interval
b) PR interval
c) Action potential duration
d) RR interval
Answer: c) Action potential duration - Route NOT used:
a) IV
b) Topical
c) Oral
d) Nerve block
Answer: c) Oral - Lidocaine is metabolized in:
a) Kidney
b) Liver
c) Lung
d) Brain
Answer: b) Liver - Use-dependent blockade means:
a) Works at rest
b) Works better in active tissue
c) Works only in nerves
d) Works only in heart
Answer: b) Works better in active tissue
FAQs
- What is the mechanism of action of lidocaine?
It blocks voltage-gated sodium channels, preventing action potential propagation. - Why is lidocaine used in arrhythmias?
It suppresses abnormal electrical activity in ischemic cardiac tissue. - What type of anesthetic is lidocaine?
An amide-type local anesthetic. - Why is lidocaine not given orally?
Due to extensive first-pass metabolism. - What is use-dependent blockade?
Greater effect in rapidly firing or depolarized cells. - What is the main toxicity of lidocaine?
CNS toxicity such as seizures.