Table of Contents
Introduction
Mebeverine is an antispasmodic drug commonly used in the management of irritable bowel syndrome (IBS) and other functional gastrointestinal disorders. It acts directly on the smooth muscle of the gastrointestinal tract to relieve spasms without significantly affecting normal gut motility. Unlike anticholinergic agents, mebeverine does not produce significant systemic anticholinergic side effects, making it a preferred option for long-term symptomatic relief.
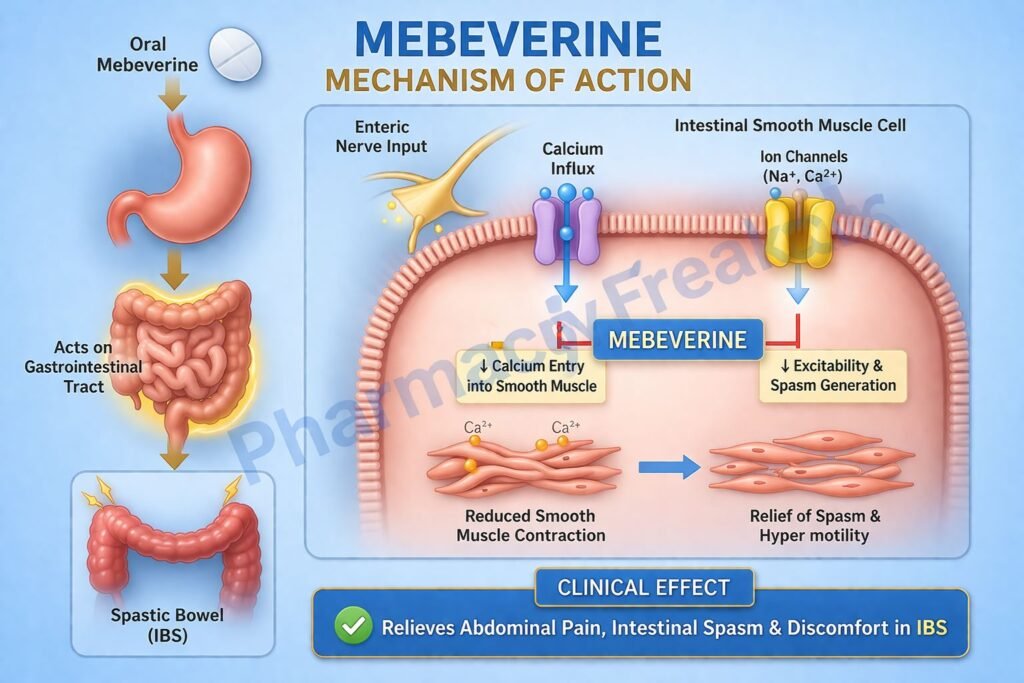
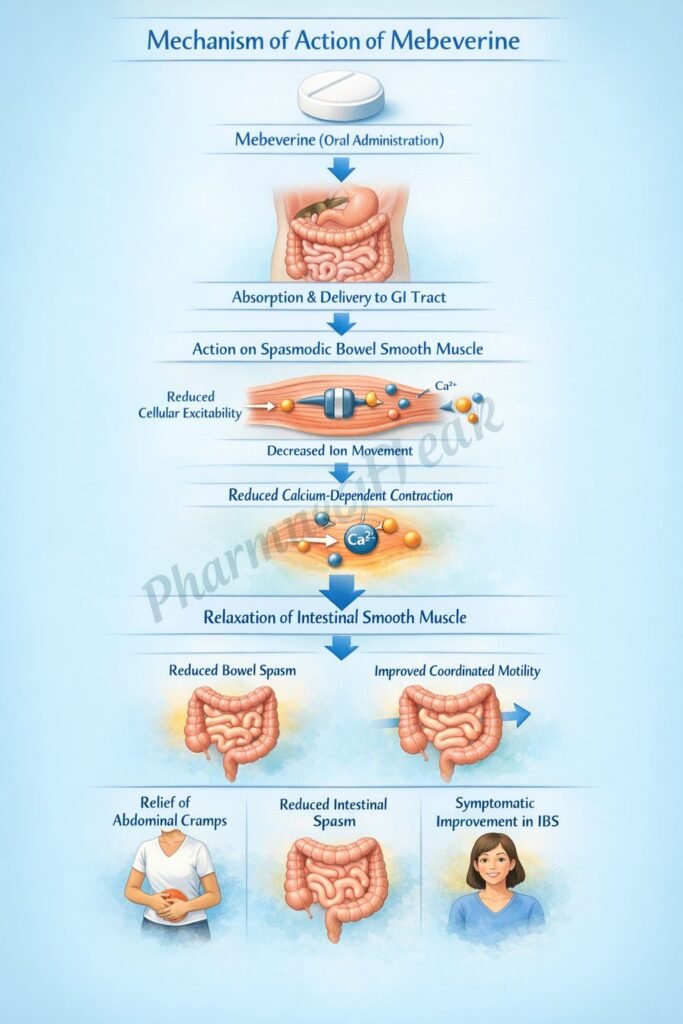
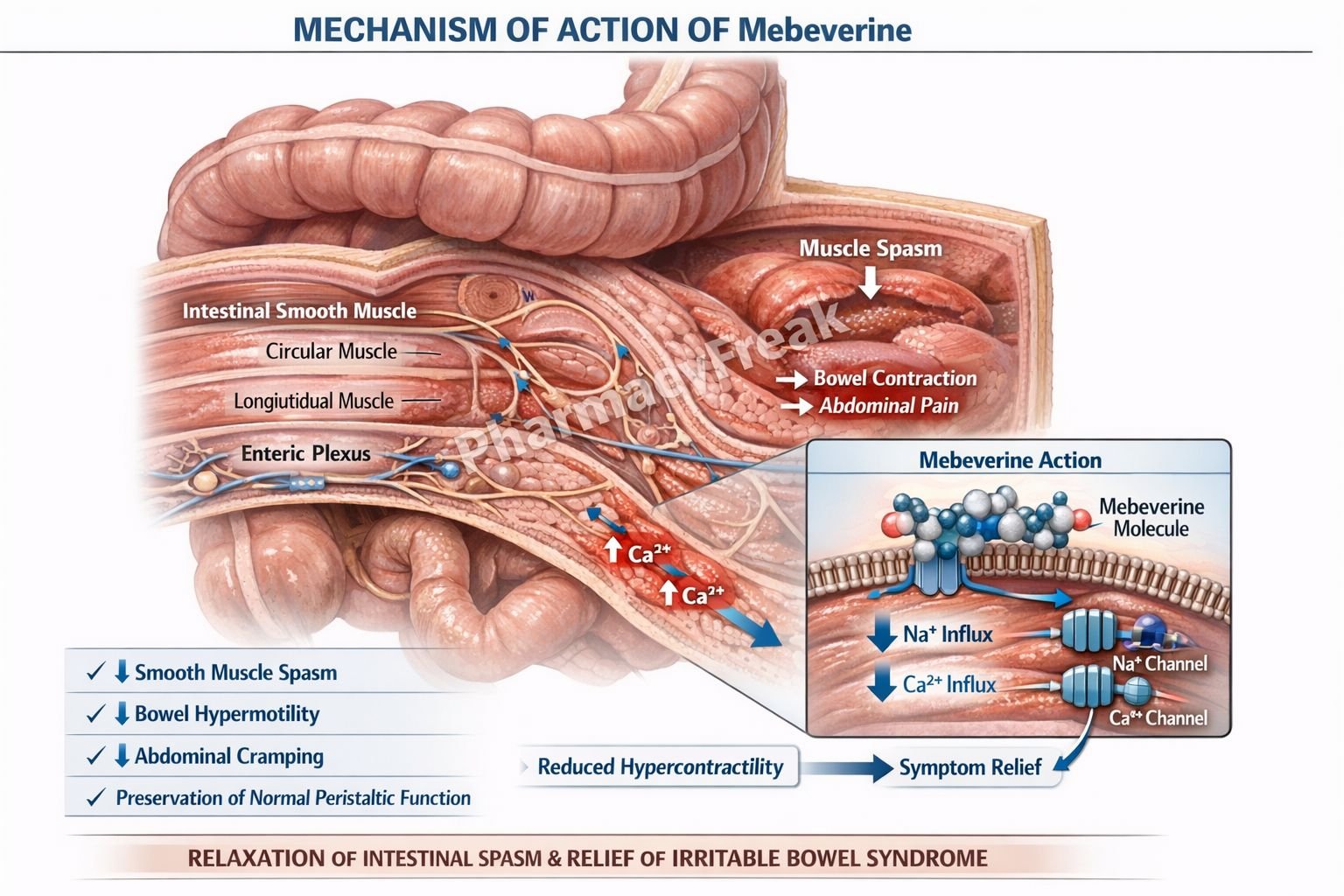
Mechanism of Action (Step-wise)
- Mebeverine acts directly on gastrointestinal smooth muscle cells.
- It blocks voltage-dependent sodium channels in smooth muscle membranes.
- This reduces sodium influx and decreases depolarization.
- Reduced depolarization leads to decreased calcium entry into smooth muscle cells.
- Lower intracellular calcium levels reduce muscle contraction.
- It also has a direct spasmolytic effect independent of autonomic innervation.
- Mebeverine may modulate potassium efflux, stabilizing membrane potential.
- The net effect is relaxation of intestinal smooth muscle and relief of spasms.
- It does not significantly affect normal peristalsis.
A key exam point is that mebeverine is a direct smooth muscle relaxant without significant anticholinergic activity.
Pharmacokinetics
Mebeverine is administered orally and undergoes extensive first-pass metabolism in the liver. It is rapidly hydrolyzed to active metabolites such as veratric acid and mebeverine alcohol. Peak plasma levels are achieved within a few hours. The drug and its metabolites are excreted mainly in urine. Because of rapid metabolism, plasma levels of the parent drug are low, and its effects are largely due to metabolites. It has a relatively short half-life but is effective with standard dosing due to its sustained smooth muscle effects.
Clinical Uses
Mebeverine is primarily used in the treatment of irritable bowel syndrome. It helps relieve abdominal pain, cramping, bloating, and discomfort associated with intestinal spasms. It is also used in other functional bowel disorders where smooth muscle spasm is a major feature. It improves patient quality of life by reducing symptoms without causing significant sedation or systemic effects.
Adverse Effects
Mebeverine is generally well tolerated. Adverse effects are uncommon and usually mild. They may include gastrointestinal discomfort, nausea, and allergic reactions such as rash or urticaria. Because it lacks significant anticholinergic activity, it does not typically cause dry mouth, blurred vision, or urinary retention, which are common with other antispasmodics.
Comparative Analysis
| Feature | Mebeverine | Dicycloverine (Dicyclomine) | Hyoscine |
|---|---|---|---|
| Class | Direct smooth muscle relaxant | Anticholinergic | Anticholinergic |
| Mechanism | Sodium channel blockade, direct action | Muscarinic receptor blockade | Muscarinic receptor blockade |
| Effect on CNS | Minimal | Moderate | Moderate |
| Anticholinergic effects | Absent | Present | Present |
| Use in IBS | Yes | Yes | Yes |
| Side effects | Minimal | Dry mouth, blurred vision | Dry mouth, tachycardia |
Mebeverine differs from anticholinergic agents like dicycloverine and hyoscine because it directly relaxes smooth muscle without blocking muscarinic receptors. This results in fewer systemic side effects and better tolerability, especially in long-term use.
MCQs
- Mebeverine belongs to which class?
a) Anticholinergic
b) Antispasmodic
c) Antibiotic
d) Proton pump inhibitor
Answer: b) Antispasmodic
- Mebeverine primarily acts on:
a) Central nervous system
b) Smooth muscle of GI tract
c) Cardiac muscle
d) Skeletal muscle
Answer: b) Smooth muscle of GI tract
- Mebeverine reduces smooth muscle contraction by decreasing:
a) Sodium influx
b) Potassium influx
c) Calcium efflux
d) Chloride influx
Answer: a) Sodium influx
- Reduced sodium entry leads to decreased:
a) Depolarization
b) Hyperpolarization
c) Protein synthesis
d) Oxygen consumption
Answer: a) Depolarization
- The main clinical use of mebeverine is:
a) Asthma
b) Hypertension
c) IBS
d) Diabetes
Answer: c) IBS
- Compared to anticholinergics, mebeverine causes:
a) More side effects
b) Less side effects
c) Equal side effects
d) Severe sedation
Answer: b) Less side effects
- Mebeverine does NOT significantly affect:
a) Muscle contraction
b) Normal peristalsis
c) Sodium channels
d) Calcium entry
Answer: b) Normal peristalsis
- Mebeverine is metabolized mainly in the:
a) Kidney
b) Liver
c) Lungs
d) Brain
Answer: b) Liver
- A common adverse effect is:
a) Severe hypotension
b) Mild GI discomfort
c) Hyperglycemia
d) Bradycardia
Answer: b) Mild GI discomfort
- Mebeverine acts independently of:
a) Hormones
b) Autonomic innervation
c) Electrolytes
d) Enzymes
Answer: b) Autonomic innervation
- Which of the following is NOT a feature of mebeverine?
a) Direct smooth muscle action
b) Anticholinergic effect
c) Relief of spasms
d) Minimal CNS effect
Answer: b) Anticholinergic effect
- Mebeverine is preferred because it:
a) Causes sedation
b) Has minimal systemic effects
c) Increases motility
d) Causes dry mouth
Answer: b) Has minimal systemic effects
FAQs
What is the mechanism of action of mebeverine?
It acts directly on gastrointestinal smooth muscle, reducing spasms by blocking sodium channels and decreasing calcium influx.
Why is mebeverine preferred over anticholinergics?
It has fewer side effects and lacks anticholinergic activity.
Does mebeverine affect normal gut motility?
No, it mainly relieves spasms without significantly altering normal peristalsis.
What condition is mebeverine mainly used for?
Irritable bowel syndrome.
Does mebeverine cause sedation?
No, it has minimal central nervous system effects.
Is mebeverine safe for long-term use?
Yes, it is generally well tolerated with minimal adverse effects.
References
Goodman & Gilman’s The Pharmacological Basis of Therapeutics – Gastrointestinal Drugs
https://accessmedicine.mhmedical.com/book.aspx?bookid=3191
Katzung: Basic and Clinical Pharmacology – GI Pharmacology
https://accessmedicine.mhmedical.com/content.aspx?bookid=3382
Tripathi: Essentials of Medical Pharmacology – Antispasmodics
https://www.jaypeedigital.com
Harrison’s Principles of Internal Medicine – Functional GI Disorders
https://accessmedicine.mhmedical.com