Table of Contents
Introduction
Ibuprofen is a widely used nonsteroidal anti-inflammatory drug (NSAID) belonging to the propionic acid class. It is commonly used for its analgesic, antipyretic, and anti-inflammatory properties. Ibuprofen is frequently prescribed in conditions such as pain, fever, and inflammatory disorders, making it a staple drug in both clinical and over-the-counter settings.
Mechanism of Action (Step-wise)
- Cyclooxygenase (COX) Enzyme Inhibition
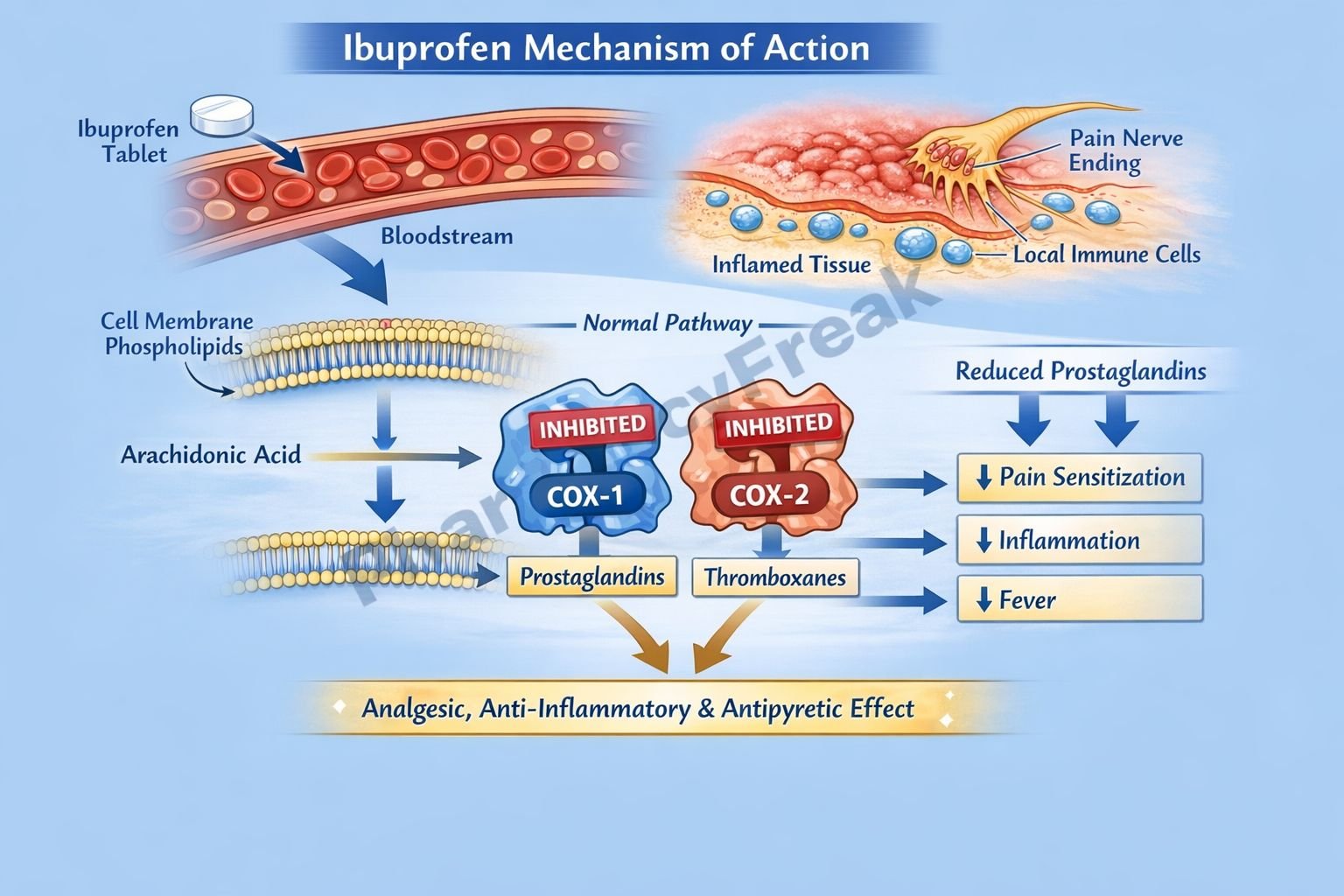
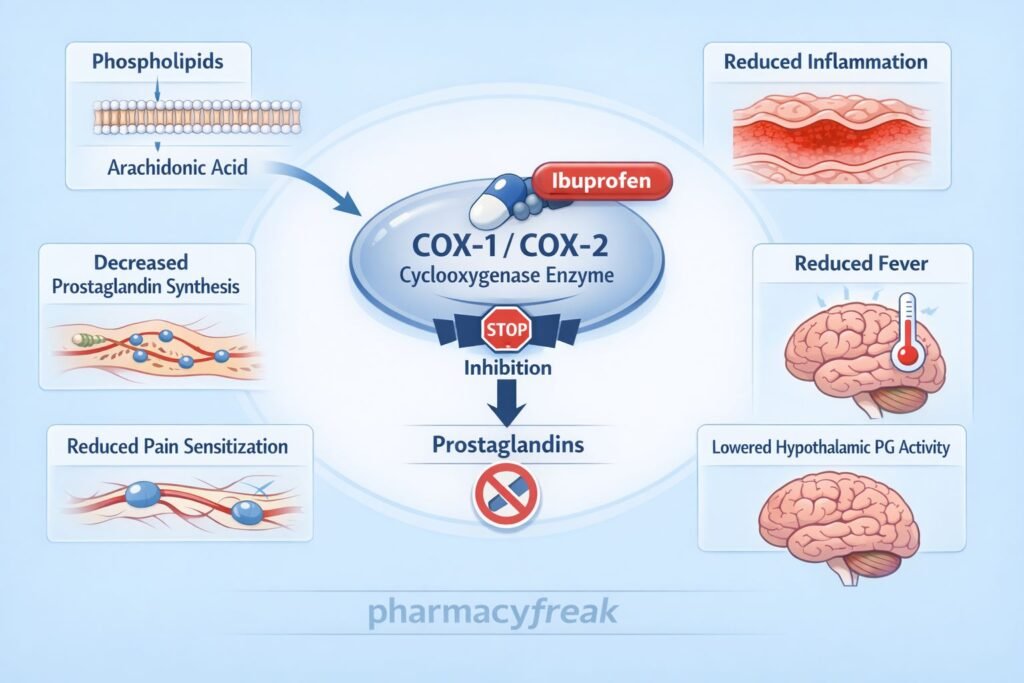
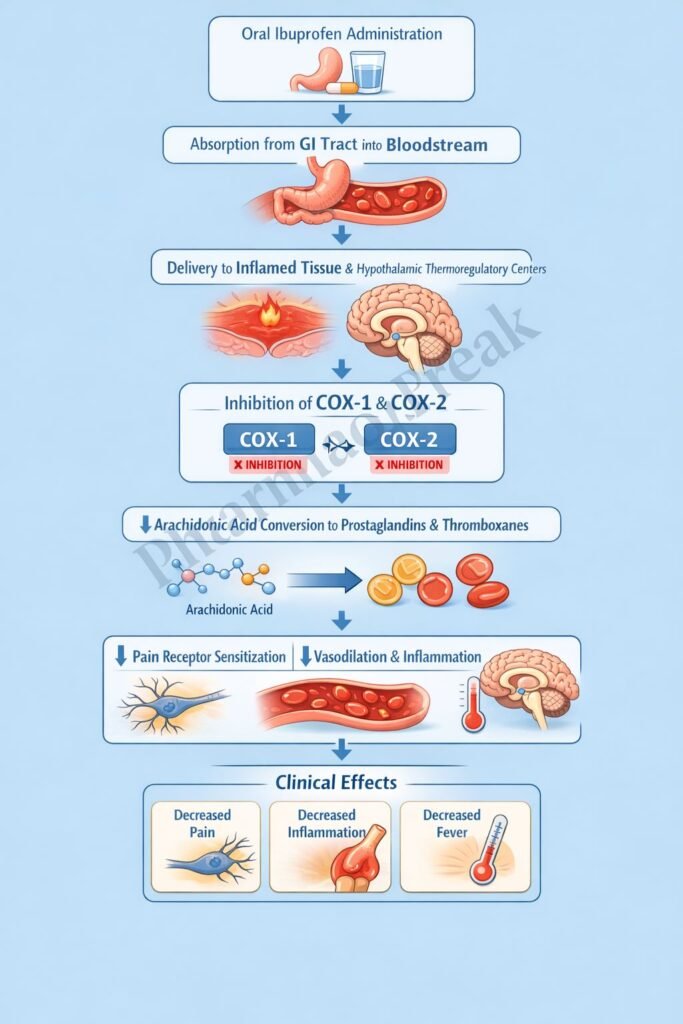
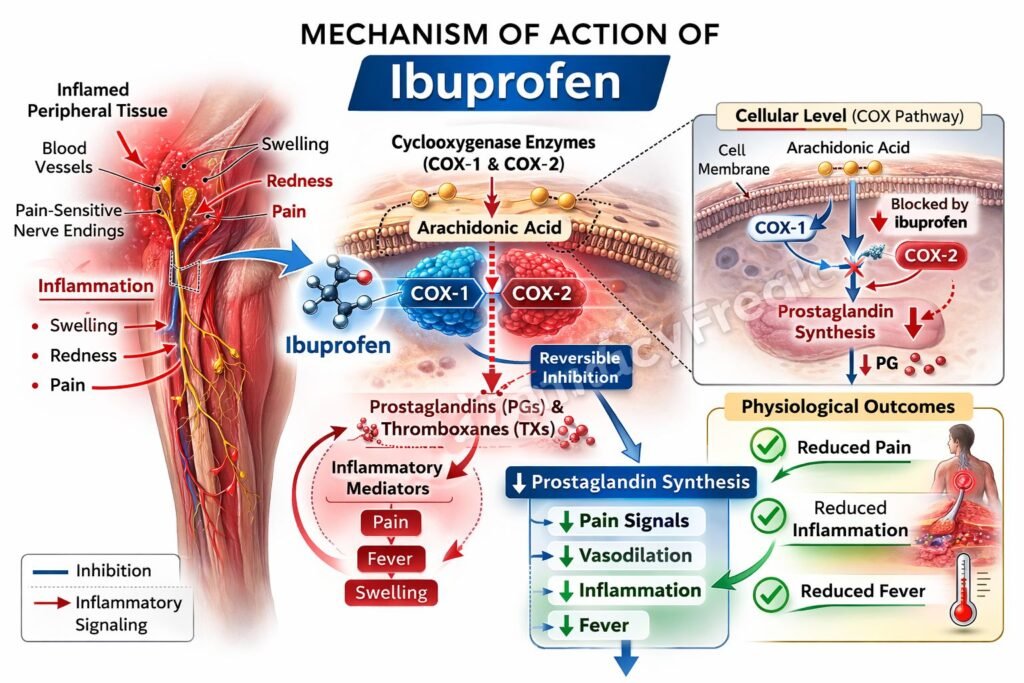
Ibuprofen non-selectively inhibits cyclooxygenase enzymes, namely COX-1 and COX-2. - Blockade of Arachidonic Acid Pathway
Normally, arachidonic acid is converted by COX enzymes into prostaglandins and thromboxanes. Ibuprofen inhibits this conversion. - Reduction in Prostaglandin Synthesis
By inhibiting COX enzymes, ibuprofen decreases the synthesis of prostaglandins (PGE2, PGI2), which are mediators of inflammation, pain, and fever. - Analgesic Effect
Reduced prostaglandins decrease sensitization of peripheral nociceptors, leading to pain relief. - Anti-inflammatory Effect
Lower prostaglandin levels reduce vasodilation, edema, and inflammatory cell recruitment. - Antipyretic Effect
In the hypothalamus, decreased prostaglandin E2 levels reset the thermoregulatory center, reducing fever. - Reversible Inhibition
Unlike aspirin, ibuprofen causes reversible inhibition of COX enzymes, allowing normal function to resume after drug clearance.
Pharmacokinetics
- Absorption: Rapidly absorbed from the gastrointestinal tract
- Bioavailability: Approximately 80–90%
- Protein Binding: Highly bound to plasma proteins (~99%)
- Metabolism: Hepatic metabolism via CYP enzymes (primarily CYP2C9)
- Half-life: Approximately 2 hours
- Excretion: Renal elimination as metabolites
Clinical Uses
- Mild to moderate pain (headache, dental pain, musculoskeletal pain)
- Fever reduction
- Inflammatory conditions (rheumatoid arthritis, osteoarthritis)
- Dysmenorrhea
- Postoperative pain management
Adverse Effects
- Gastrointestinal irritation (gastritis, ulcers)
- Risk of gastrointestinal bleeding
- Renal impairment with prolonged use
- Hypersensitivity reactions (rash, bronchospasm)
- Increased cardiovascular risk with long-term use
- Fluid retention and edema
Comparative Analysis
| Feature | Ibuprofen | Aspirin | Paracetamol |
|---|---|---|---|
| COX Inhibition | Non-selective, reversible | Non-selective, irreversible | Weak COX inhibition (central) |
| Anti-inflammatory | Yes | Yes | Minimal |
| Analgesic | Yes | Yes | Yes |
| Antipyretic | Yes | Yes | Yes |
| Platelet Effect | Mild, reversible | Strong, irreversible | None |
| GI Toxicity | Moderate | High | Low |
Ibuprofen provides a balanced profile with effective analgesic, antipyretic, and anti-inflammatory actions while having a lower risk of gastrointestinal toxicity compared to aspirin. However, unlike paracetamol, it carries a higher risk of GI and renal side effects.
MCQs
- Ibuprofen primarily inhibits which enzymes?
a) Lipoxygenase
b) Cyclooxygenase
c) Phospholipase A2
d) Adenylate cyclase
Answer: b) Cyclooxygenase - Which prostaglandin is mainly responsible for fever?
a) PGE2
b) PGF2α
c) TXA2
d) PGD2
Answer: a) PGE2 - Ibuprofen inhibition of COX is:
a) Irreversible
b) Competitive and reversible
c) Non-competitive
d) Permanent
Answer: b) Competitive and reversible - Which effect is NOT associated with ibuprofen?
a) Analgesic
b) Antipyretic
c) Anti-inflammatory
d) Antibacterial
Answer: d) Antibacterial - Ibuprofen reduces pain by:
a) Blocking sodium channels
b) Reducing prostaglandin synthesis
c) Increasing serotonin
d) Blocking NMDA receptors
Answer: b) Reducing prostaglandin synthesis - Site of antipyretic action of ibuprofen:
a) Liver
b) Kidney
c) Hypothalamus
d) Heart
Answer: c) Hypothalamus - Main pathway inhibited by ibuprofen:
a) Glycolysis
b) Arachidonic acid pathway
c) Urea cycle
d) Krebs cycle
Answer: b) Arachidonic acid pathway - Major adverse effect of ibuprofen:
a) Hepatotoxicity
b) GI irritation
c) Ototoxicity
d) Neurotoxicity
Answer: b) GI irritation - Ibuprofen is classified as:
a) Opioid
b) NSAID
c) Steroid
d) Antibiotic
Answer: b) NSAID - Ibuprofen metabolism occurs in:
a) Kidney
b) Liver
c) Lung
d) Intestine
Answer: b) Liver
FAQs
- What is the primary mechanism of action of ibuprofen?
Ibuprofen inhibits COX-1 and COX-2 enzymes, reducing prostaglandin synthesis. - Is ibuprofen a selective COX-2 inhibitor?
No, it is a non-selective COX inhibitor. - Why does ibuprofen cause gastric irritation?
It inhibits COX-1, reducing protective prostaglandins in the gastric mucosa. - Can ibuprofen reduce fever?
Yes, it lowers hypothalamic prostaglandin levels, reducing fever. - How is ibuprofen different from aspirin?
Ibuprofen inhibits COX reversibly, whereas aspirin causes irreversible inhibition. - Is ibuprofen safe for long-term use?
Long-term use increases risks of GI, renal, and cardiovascular complications.
References
- Goodman & Gilman’s The Pharmacological Basis of Therapeutics – NSAIDs Chapter
https://accessmedicine.mhmedical.com/content.aspx?bookid=2189§ionid=167381736 - Katzung: Basic and Clinical Pharmacology – Nonsteroidal Anti-inflammatory Drugs
https://accessmedicine.mhmedical.com/content.aspx?bookid=2249§ionid=175215145 - Tripathi: Essentials of Medical Pharmacology – NSAIDs Section
https://www.jaypeebrothers.com/pgDetails.aspx?cat=s&book_id=9789352706928 - Harrison’s Principles of Internal Medicine – Pain and Anti-inflammatory Therapy
https://accessmedicine.mhmedical.com/content.aspx?bookid=3095§ionid=263410339