Table of Contents
Introduction
Lovenox (enoxaparin) is a low molecular weight heparin (LMWH) widely used as an anticoagulant for the prevention and treatment of thromboembolic disorders. It is derived from unfractionated heparin but has more predictable pharmacokinetics and a more selective mechanism of action. Enoxaparin primarily enhances the activity of antithrombin III, leading to inhibition of key clotting factors and prevention of thrombus formation.
Mechanism of Action (Step-wise)
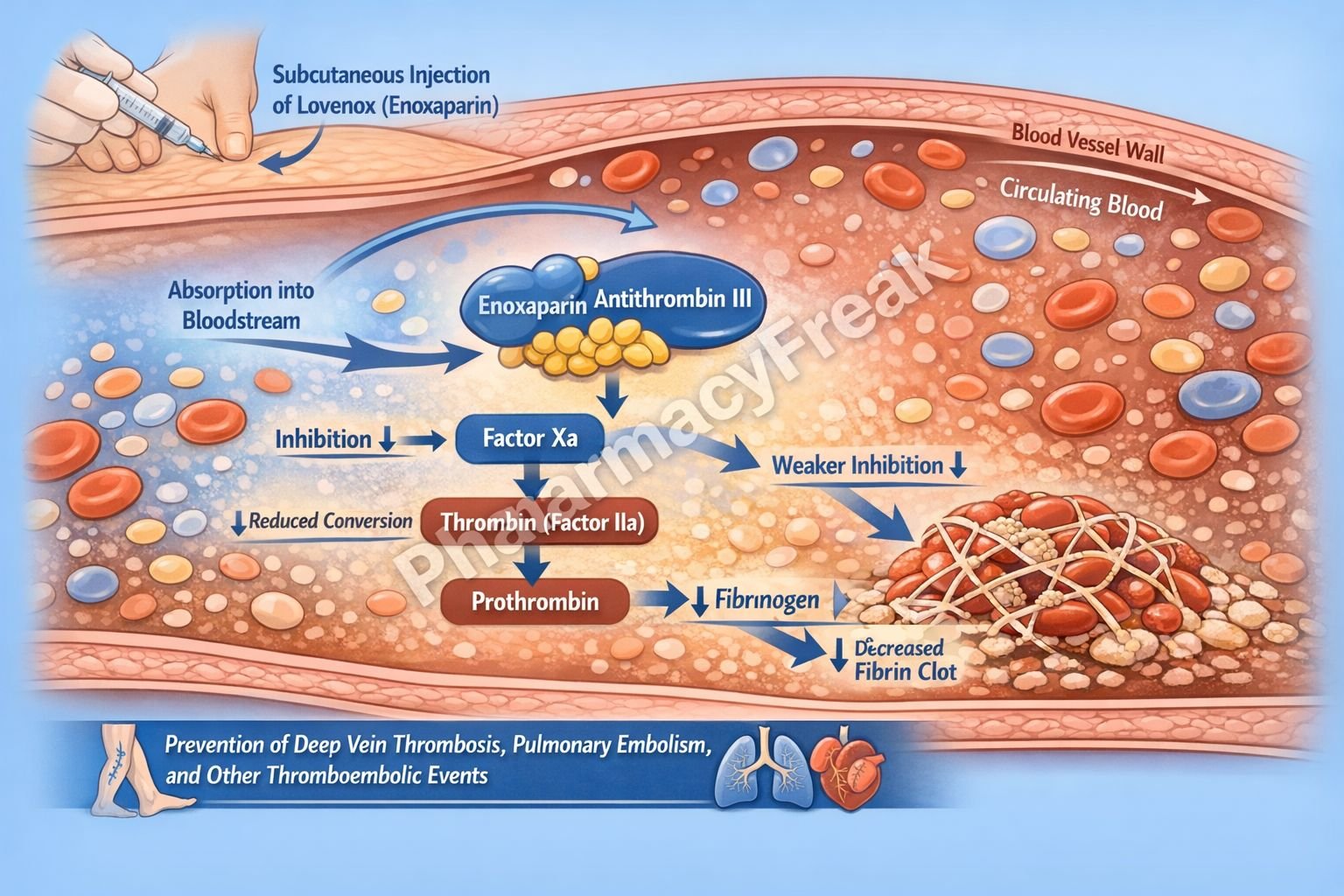
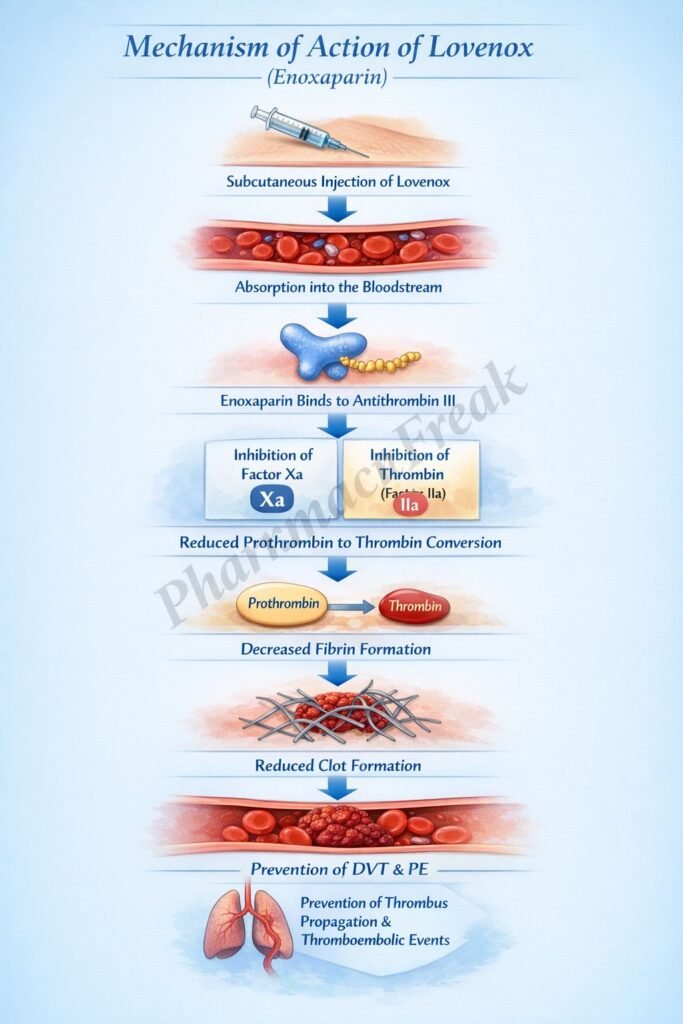
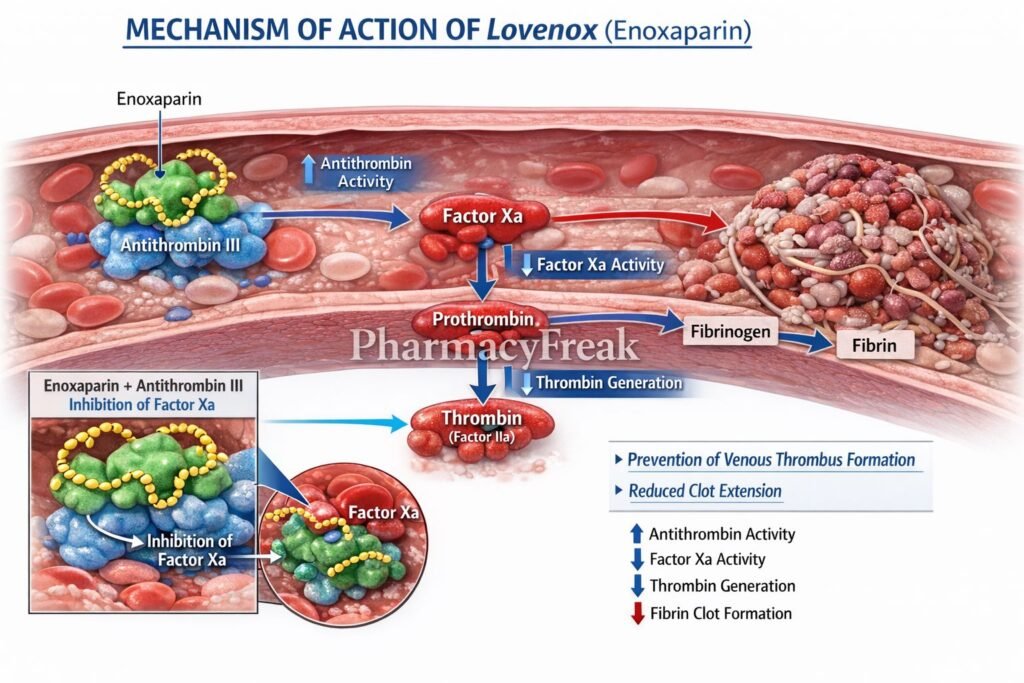
- Enoxaparin binds to antithrombin III (ATIII), a natural anticoagulant present in plasma.
- This binding induces a conformational change in ATIII, increasing its inhibitory activity.
- Activated ATIII selectively inhibits factor Xa.
- Inhibition of factor Xa prevents the conversion of prothrombin (factor II) to thrombin (factor IIa).
- Reduced thrombin levels decrease fibrin formation.
- This inhibits the formation and propagation of blood clots.
- Compared to unfractionated heparin, enoxaparin has a greater effect on factor Xa than on thrombin.
- It does not significantly affect existing clots but prevents their extension and formation of new clots.
A key exam concept is that LMWHs like enoxaparin predominantly inhibit factor Xa via antithrombin III activation.
Pharmacokinetics
Enoxaparin is administered subcutaneously and has high bioavailability compared to unfractionated heparin. It has a longer half-life, allowing once or twice daily dosing. Its anticoagulant response is more predictable, reducing the need for routine monitoring in most patients. It is primarily eliminated via the kidneys, so dose adjustment is required in renal impairment. Unlike unfractionated heparin, enoxaparin has limited binding to plasma proteins, contributing to its consistent effect.
Clinical Uses
Enoxaparin is used for the prevention and treatment of deep vein thrombosis (DVT) and pulmonary embolism (PE). It is also used in acute coronary syndromes, including unstable angina and myocardial infarction. Additionally, it is commonly used for thromboprophylaxis in surgical and immobilized patients. Its predictable effect and ease of administration make it a preferred anticoagulant in many clinical settings.
Adverse Effects
The most common adverse effect is bleeding, which can range from minor to severe. Heparin-induced thrombocytopenia (HIT) can occur but is less common than with unfractionated heparin. Injection site reactions such as pain and hematoma may occur. Long-term use may be associated with osteoporosis. Because it is renally cleared, accumulation and increased bleeding risk can occur in renal impairment.
Comparative Analysis
| Feature | Enoxaparin (LMWH) | Unfractionated Heparin | Warfarin |
|---|---|---|---|
| Mechanism | ATIII → inhibits factor Xa | ATIII → inhibits Xa and IIa | Inhibits vitamin K–dependent factors |
| Administration | Subcutaneous | IV or SC | Oral |
| Monitoring | Minimal | Requires aPTT monitoring | Requires INR monitoring |
| Half-life | Longer | Shorter | Long |
| HIT risk | Lower | Higher | None |
| Use | DVT, PE, ACS | Acute anticoagulation | Long-term anticoagulation |
Enoxaparin differs from unfractionated heparin in having more selective inhibition of factor Xa and more predictable pharmacokinetics. Compared to warfarin, it acts rapidly and does not require routine INR monitoring, making it useful in acute settings.
MCQs
- Lovenox (enoxaparin) belongs to which class?
a) Vitamin K antagonists
b) Low molecular weight heparins
c) Direct thrombin inhibitors
d) Antiplatelet agents
Answer: b) Low molecular weight heparins
- Enoxaparin acts primarily by enhancing:
a) Protein C
b) Antithrombin III
c) Platelet aggregation
d) Fibrinolysis
Answer: b) Antithrombin III
- The main clotting factor inhibited by enoxaparin is:
a) Factor IIa
b) Factor VII
c) Factor Xa
d) Factor XIII
Answer: c) Factor Xa
- Inhibition of factor Xa leads to decreased formation of:
a) Fibrinogen
b) Prothrombin
c) Thrombin
d) Platelets
Answer: c) Thrombin
- Enoxaparin is administered via:
a) Oral route
b) Intramuscular route
c) Subcutaneous route
d) Inhalation
Answer: c) Subcutaneous route
- Compared to unfractionated heparin, enoxaparin has:
a) Less predictable effect
b) More protein binding
c) More predictable pharmacokinetics
d) Shorter half-life
Answer: c) More predictable pharmacokinetics
- The most common adverse effect is:
a) Hypoglycemia
b) Bleeding
c) Hypertension
d) Constipation
Answer: b) Bleeding
- HIT is:
a) More common with LMWH
b) Less common with LMWH
c) Not associated
d) Always fatal
Answer: b) Less common with LMWH
- Enoxaparin is eliminated primarily by:
a) Liver
b) Kidney
c) Lungs
d) Skin
Answer: b) Kidney
- Enoxaparin is used in:
a) Asthma
b) DVT
c) Diabetes
d) Hyperthyroidism
Answer: b) DVT
- Enoxaparin has greater activity against:
a) Factor IIa
b) Factor Xa
c) Factor IX
d) Factor VIII
Answer: b) Factor Xa
- Compared to warfarin, enoxaparin:
a) Has delayed onset
b) Requires INR monitoring
c) Has rapid onset
d) Is less effective
Answer: c) Has rapid onset
FAQs
What is the mechanism of action of enoxaparin?
It enhances antithrombin III activity, leading to inhibition of factor Xa and reduced thrombin formation.
Why is enoxaparin preferred over unfractionated heparin?
It has more predictable pharmacokinetics and requires less monitoring.
Does enoxaparin dissolve existing clots?
No, it prevents clot formation and extension.
What is the main risk associated with enoxaparin?
Bleeding.
Is monitoring required for enoxaparin?
Routine monitoring is usually not required, except in special populations.
Can enoxaparin cause thrombocytopenia?
Yes, but less commonly than unfractionated heparin.
References
Goodman & Gilman’s The Pharmacological Basis of Therapeutics – Anticoagulants
https://accessmedicine.mhmedical.com/book.aspx?bookid=3191
Katzung: Basic and Clinical Pharmacology – Anticoagulants
https://accessmedicine.mhmedical.com/content.aspx?bookid=3382
Tripathi: Essentials of Medical Pharmacology – Anticoagulants
https://www.jaypeedigital.com
Harrison’s Principles of Internal Medicine – Thromboembolic Disorders
https://accessmedicine.mhmedical.com