Introduction
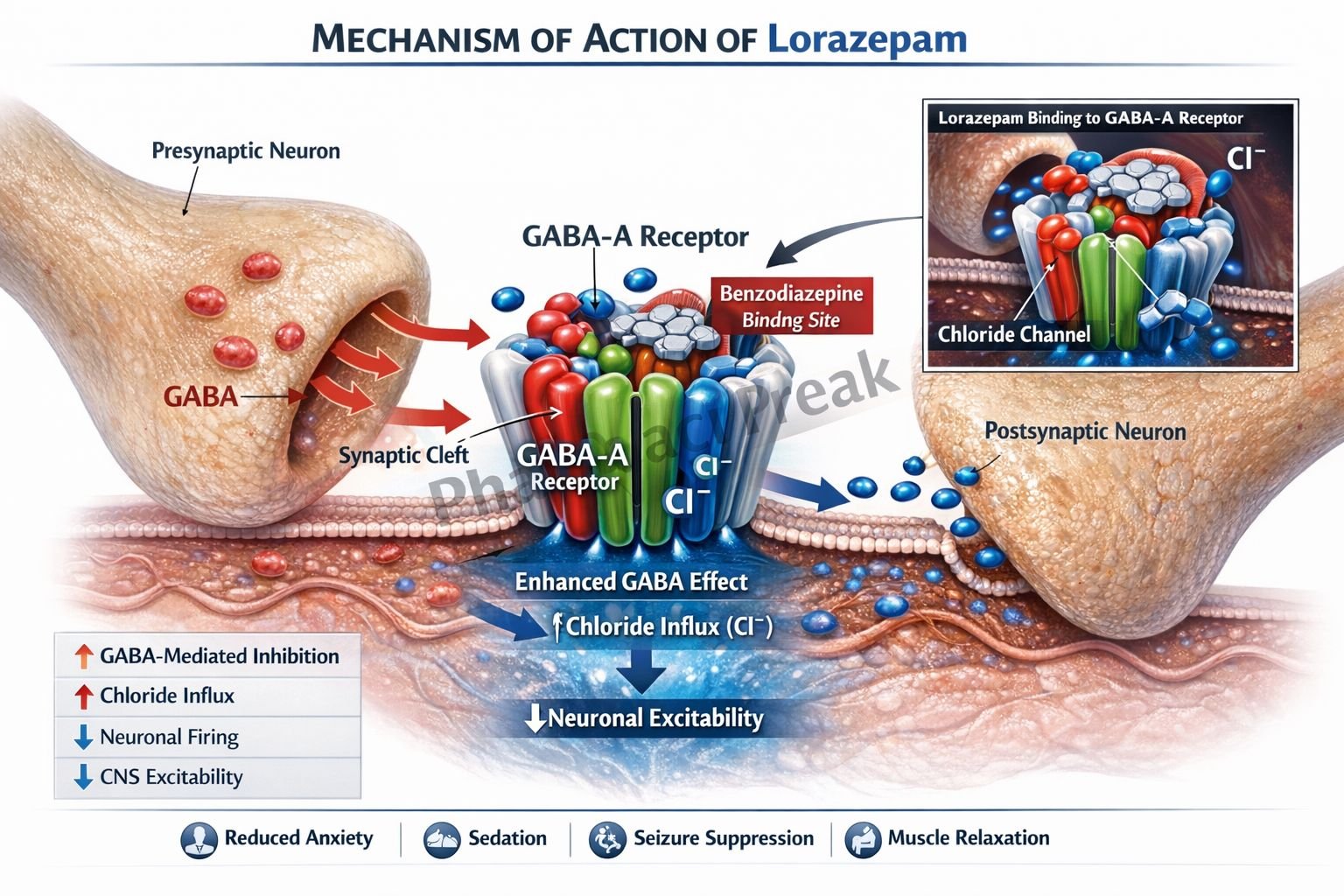
Lorazepam is a benzodiazepine widely used for its anxiolytic, sedative, anticonvulsant, and muscle relaxant properties. It is commonly prescribed in anxiety disorders, status epilepticus, and as a pre-anesthetic medication. Lorazepam acts by enhancing the inhibitory neurotransmitter gamma-aminobutyric acid (GABA) in the central nervous system, leading to decreased neuronal excitability.
Mechanism of Action (Step-wise)
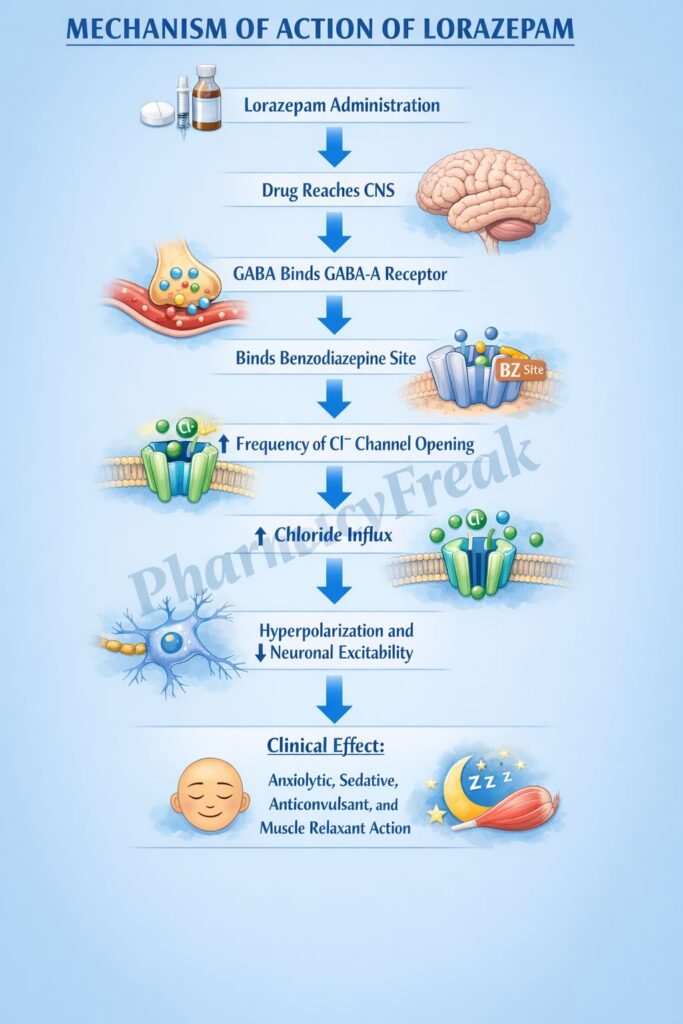
- Lorazepam binds to the benzodiazepine binding site on the GABA-A receptor complex in the central nervous system.
- This site is located between the α and γ subunits of the GABA-A receptor.
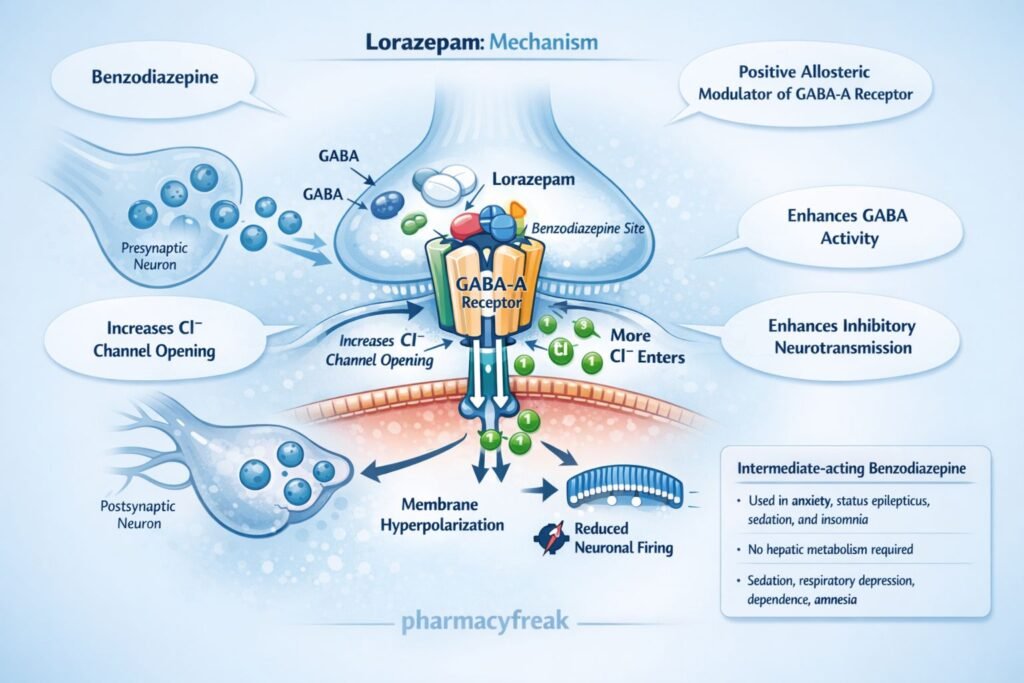
- Lorazepam does not directly activate the receptor but enhances the effect of GABA (positive allosteric modulation).
- It increases the frequency of chloride channel opening when GABA binds.
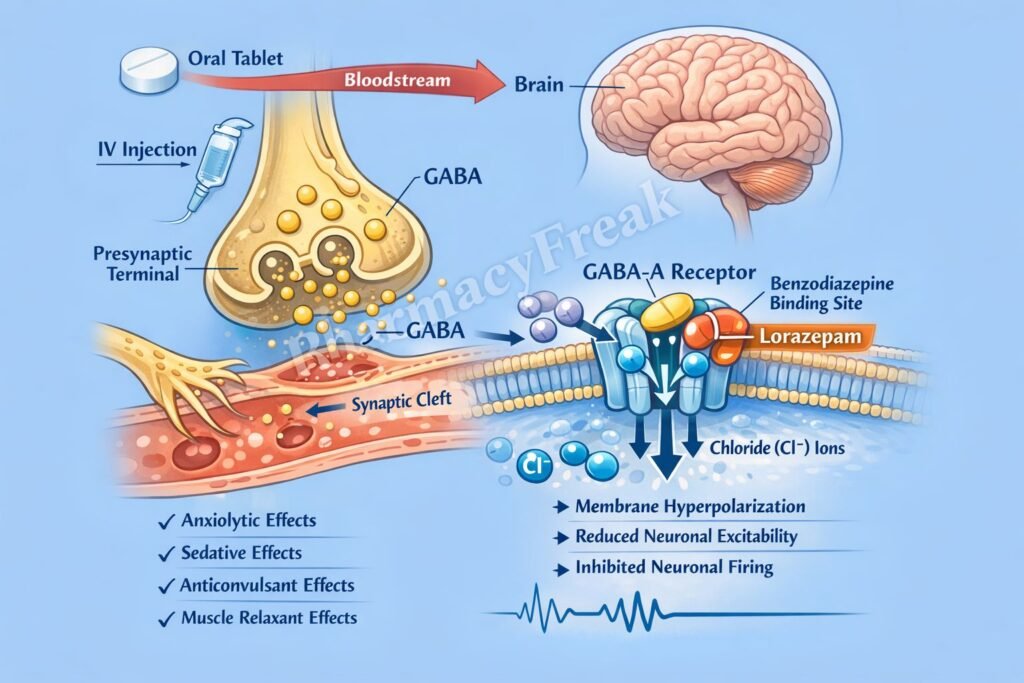
- Increased chloride influx leads to hyperpolarization of the neuronal membrane.
- Hyperpolarization decreases neuronal excitability.
- This results in anxiolytic, sedative, anticonvulsant, and muscle relaxant effects.
- The effect is dependent on the presence of GABA, which limits excessive CNS depression compared to direct agonists.
A key exam concept is that benzodiazepines increase the frequency of chloride channel opening, whereas barbiturates increase the duration.
Pharmacokinetics
Lorazepam is administered orally, intravenously, or intramuscularly. It is well absorbed and has intermediate onset and duration of action. Unlike many other benzodiazepines, lorazepam does not undergo oxidative metabolism; instead, it is directly conjugated in the liver to inactive metabolites. This makes it safer in patients with liver impairment compared to other benzodiazepines. It has moderate protein binding and is eliminated through the kidneys. Its relatively predictable pharmacokinetics make it useful in acute settings such as status epilepticus.
Clinical Uses
Lorazepam is widely used in clinical practice. It is indicated for anxiety disorders and acute anxiety episodes. It is a drug of choice for status epilepticus due to its rapid onset when given intravenously. It is also used for sedation before medical procedures, management of alcohol withdrawal symptoms, and as a short-term treatment for insomnia. Its reliable pharmacokinetics and efficacy make it a commonly used benzodiazepine in hospital settings.
Adverse Effects
Common adverse effects include sedation, drowsiness, dizziness, and impaired coordination. Cognitive impairment and anterograde amnesia may occur. Respiratory depression can occur, especially when combined with other CNS depressants such as opioids or alcohol. Long-term use can lead to tolerance, dependence, and withdrawal symptoms upon discontinuation. Elderly patients are particularly susceptible to falls and confusion. Overdose can result in severe CNS depression but is generally less dangerous than barbiturate overdose when used alone.
Comparative Analysis
| Feature | Lorazepam | Diazepam | Midazolam |
|---|---|---|---|
| Class | Benzodiazepine | Benzodiazepine | Benzodiazepine |
| Duration | Intermediate | Long | Short |
| Metabolism | Direct conjugation | Hepatic oxidation (active metabolites) | Hepatic metabolism |
| Use in liver disease | Safer | Less preferred | Caution |
| Common use | Anxiety, seizures | Anxiety, muscle spasm | Procedural sedation |
| Onset (IV) | Moderate | Rapid | Very rapid |
Lorazepam is preferred over diazepam in patients with liver impairment because it undergoes direct conjugation rather than oxidative metabolism. Compared to midazolam, lorazepam has a longer duration of action, making it more suitable for sustained anticonvulsant and anxiolytic effects.
MCQs
- Lorazepam belongs to which class of drugs?
a) Antipsychotics
b) Benzodiazepines
c) Barbiturates
d) Antidepressants
Answer: b) Benzodiazepines
- Lorazepam acts on which receptor?
a) NMDA receptor
b) GABA-A receptor
c) Dopamine receptor
d) Serotonin receptor
Answer: b) GABA-A receptor
- Lorazepam enhances the effect of:
a) Dopamine
b) GABA
c) Serotonin
d) Acetylcholine
Answer: b) GABA
- Benzodiazepines increase:
a) Duration of chloride channel opening
b) Frequency of chloride channel opening
c) Sodium influx
d) Calcium influx
Answer: b) Frequency of chloride channel opening
- The result of lorazepam action is:
a) Depolarization
b) Hyperpolarization
c) Increased excitation
d) Calcium release
Answer: b) Hyperpolarization
- Lorazepam is commonly used in:
a) Hypertension
b) Status epilepticus
c) Diabetes
d) Asthma
Answer: b) Status epilepticus
- Which effect is NOT associated with lorazepam?
a) Sedation
b) Anxiolysis
c) Anticonvulsant effect
d) Antibiotic action
Answer: d) Antibiotic action
- Lorazepam metabolism occurs via:
a) CYP450 oxidation
b) Direct conjugation
c) Renal metabolism
d) Plasma enzymes
Answer: b) Direct conjugation
- A major risk of long-term use is:
a) Hyperglycemia
b) Dependence
c) Hypertension
d) Kidney stones
Answer: b) Dependence
- Respiratory depression risk increases with:
a) Food intake
b) Combination with opioids
c) Exercise
d) Vitamins
Answer: b) Combination with opioids
- Compared to diazepam, lorazepam is:
a) More hepatotoxic
b) Safer in liver disease
c) Shorter acting
d) Less effective
Answer: b) Safer in liver disease
- Lorazepam causes neuronal inhibition by:
a) Increasing sodium entry
b) Increasing chloride entry
c) Blocking potassium
d) Increasing calcium
Answer: b) Increasing chloride entry
FAQs
What is the mechanism of action of lorazepam?
It enhances GABA-A receptor activity, increasing chloride influx and causing neuronal inhibition.
Why is lorazepam safer in liver disease?
It undergoes direct conjugation rather than oxidative metabolism.
What is the difference between benzodiazepines and barbiturates?
Benzodiazepines increase the frequency of chloride channel opening, while barbiturates increase the duration.
Why is lorazepam used in status epilepticus?
It has a rapid onset and effective anticonvulsant activity.
Can lorazepam cause dependence?
Yes, long-term use can lead to tolerance and dependence.
What are common side effects of lorazepam?
Sedation, dizziness, impaired coordination, and memory impairment.
References
Goodman & Gilman’s The Pharmacological Basis of Therapeutics – Sedative-Hypnotics
https://accessmedicine.mhmedical.com/book.aspx?bookid=3191
Katzung: Basic and Clinical Pharmacology – Benzodiazepines
https://accessmedicine.mhmedical.com/content.aspx?bookid=3382
Tripathi: Essentials of Medical Pharmacology – Sedative-Hypnotics
https://www.jaypeedigital.com
Harrison’s Principles of Internal Medicine – Anxiety Disorders
https://accessmedicine.mhmedical.com