Table of Contents
Introduction
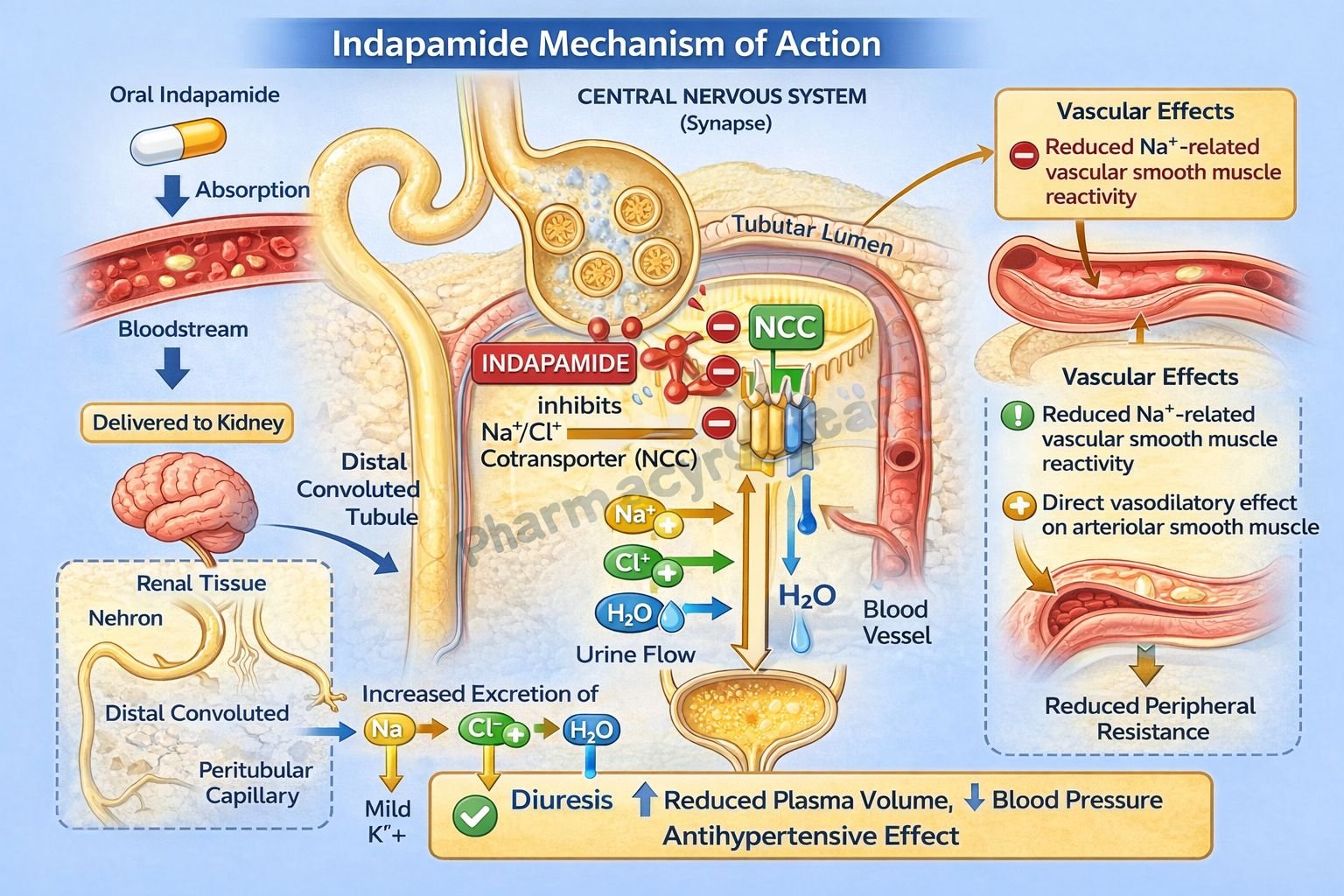
Indapamide is a thiazide-like diuretic commonly used in the management of hypertension and edema. Although structurally different from classic thiazides, it shares similar pharmacological properties. Indapamide is particularly valued for its dual action, combining diuretic effects with direct vasodilatory activity, making it effective in long-term blood pressure control.
Mechanism of Action (Step-wise)
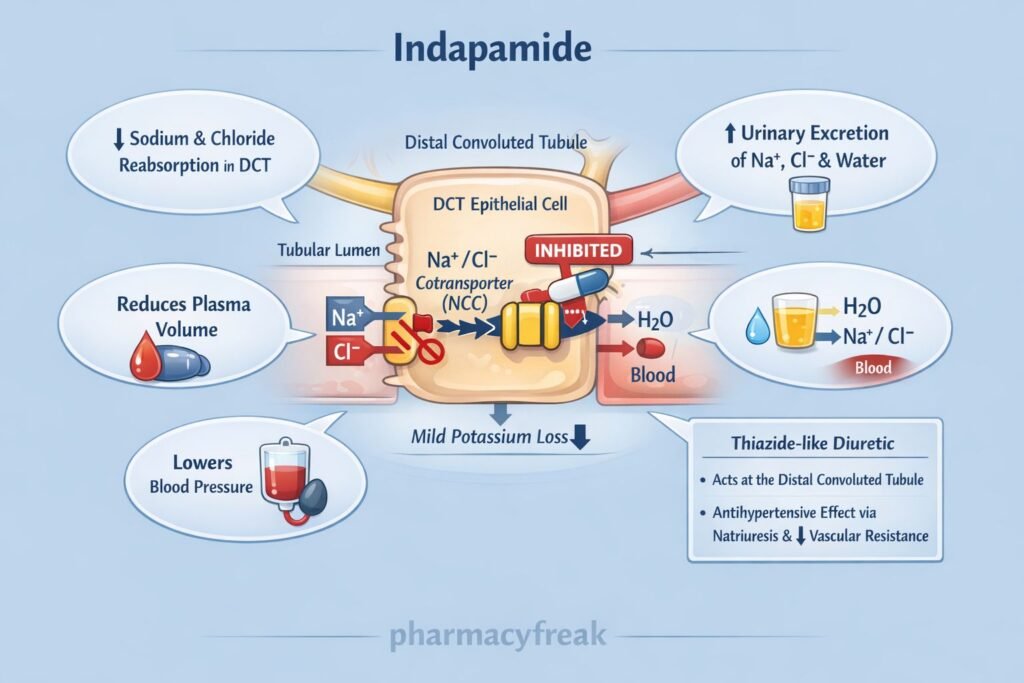
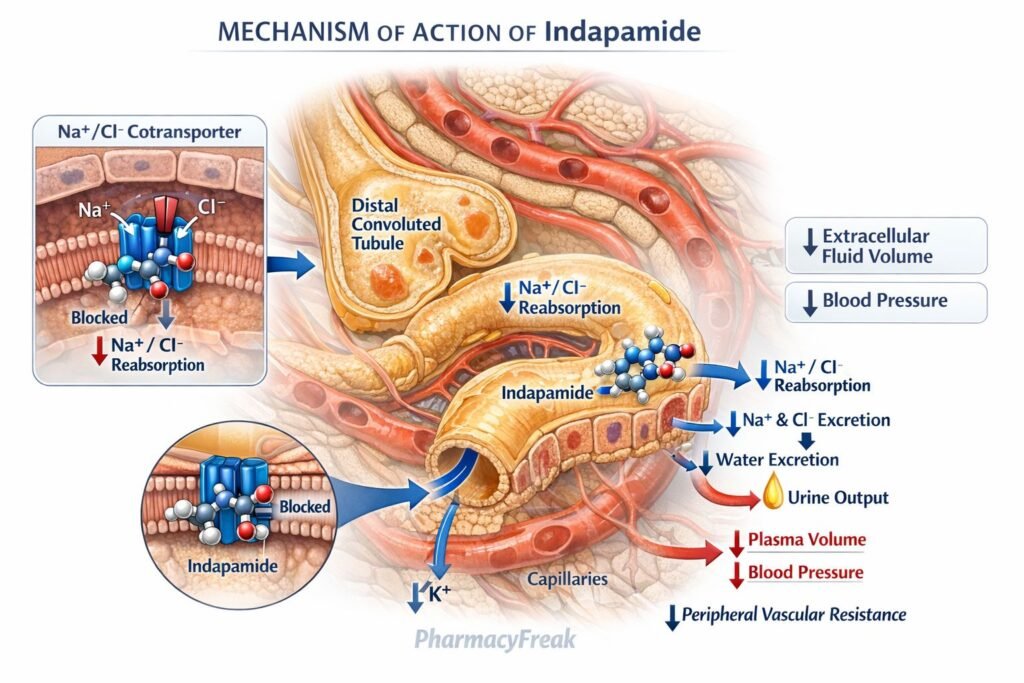
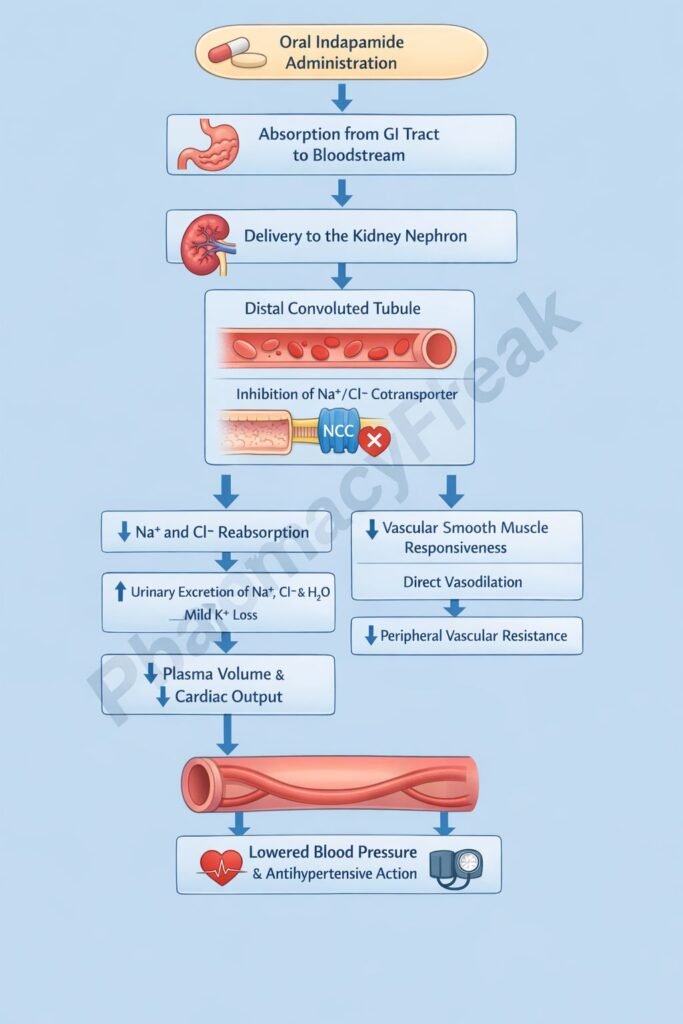
- Inhibition of Na⁺/Cl⁻ Cotransporter (NCC)
Indapamide inhibits the sodium-chloride cotransporter in the distal convoluted tubule (DCT) of the nephron. - Increased Sodium and Water Excretion
Blocking NCC reduces sodium reabsorption, leading to increased excretion of sodium and water (natriuresis and diuresis). - Reduction in Plasma Volume
Initial diuretic effect decreases plasma volume, reducing cardiac output and lowering blood pressure. - Decrease in Peripheral Vascular Resistance
With chronic use, indapamide exerts a direct vasodilatory effect on arterioles, reducing systemic vascular resistance. - Calcium Channel Modulation
It may reduce calcium influx into vascular smooth muscle cells, contributing to vasodilation. - Enhanced Prostaglandin Synthesis
Indapamide may increase vasodilatory prostaglandins, further aiding blood pressure reduction. - Sustained Antihypertensive Effect
Long-term blood pressure control is mainly due to decreased peripheral resistance rather than diuresis alone.
Pharmacokinetics
- Absorption: Well absorbed orally
- Bioavailability: High
- Protein Binding: Approximately 70–80%
- Metabolism: Hepatic metabolism
- Half-life: Long (≈14–18 hours)
- Excretion: Primarily renal (as metabolites)
Clinical Uses
- Hypertension (first-line or combination therapy)
- Edema associated with heart failure
- Prevention of cardiovascular events in hypertensive patients
Adverse Effects
- Hypokalemia
- Hyponatremia
- Hyperuricemia (may precipitate gout)
- Hyperglycemia
- Dizziness and orthostatic hypotension
- Dehydration
Comparative Analysis
| Feature | Indapamide | Hydrochlorothiazide | Furosemide |
|---|---|---|---|
| Class | Thiazide-like | Thiazide | Loop diuretic |
| Site of Action | DCT | DCT | Loop of Henle |
| Diuretic potency | Moderate | Moderate | High |
| Vasodilatory effect | Present | Minimal | Minimal |
| Duration of action | Long | Intermediate | Short |
| Use in hypertension | Yes (preferred) | Yes | Less preferred |
Indapamide differs from classical thiazides by having a stronger and sustained antihypertensive effect due to its additional vasodilatory action. Compared to loop diuretics like furosemide, it has a milder diuretic effect but is better suited for long-term blood pressure management.
MCQs
- Indapamide acts primarily on which part of the nephron?
a) Proximal tubule
b) Loop of Henle
c) Distal convoluted tubule
d) Collecting duct
Answer: c) Distal convoluted tubule - Which transporter is inhibited by indapamide?
a) Na⁺/K⁺ ATPase
b) Na⁺/Cl⁻ cotransporter
c) Na⁺/H⁺ exchanger
d) Ca²⁺ channel
Answer: b) Na⁺/Cl⁻ cotransporter - Main antihypertensive mechanism of long-term use:
a) Increased cardiac output
b) Vasodilation
c) Increased blood volume
d) Increased heart rate
Answer: b) Vasodilation - Common electrolyte imbalance:
a) Hyperkalemia
b) Hypokalemia
c) Hypercalcemia
d) Hypernatremia
Answer: b) Hypokalemia - Indapamide belongs to which class?
a) Loop diuretic
b) Potassium-sparing diuretic
c) Thiazide-like diuretic
d) Carbonic anhydrase inhibitor
Answer: c) Thiazide-like diuretic - Chronic use reduces:
a) Cardiac output
b) Peripheral resistance
c) Blood glucose
d) Platelet count
Answer: b) Peripheral resistance - Which condition may worsen with indapamide?
a) Hypotension
b) Gout
c) Asthma
d) Epilepsy
Answer: b) Gout - Indapamide increases excretion of:
a) Calcium
b) Sodium
c) Potassium retention
d) Glucose
Answer: b) Sodium - Major benefit over loop diuretics:
a) Stronger diuresis
b) Longer antihypertensive effect
c) Faster onset
d) No electrolyte imbalance
Answer: b) Longer antihypertensive effect - Mechanism includes:
a) ACE inhibition
b) Beta-blockade
c) Calcium channel modulation
d) Insulin release
Answer: c) Calcium channel modulation
FAQs
- What is the primary mechanism of action of indapamide?
It inhibits the Na⁺/Cl⁻ cotransporter in the distal convoluted tubule. - Is indapamide a true thiazide?
No, it is a thiazide-like diuretic with similar effects. - Why is indapamide effective in hypertension?
It reduces both plasma volume and peripheral vascular resistance. - Does indapamide cause hypokalemia?
Yes, due to increased potassium loss in urine. - Can indapamide cause gout?
Yes, it can increase uric acid levels. - What makes indapamide unique among diuretics?
Its additional direct vasodilatory action.