Table of Contents
Introduction
Buprenorphine is a semi-synthetic opioid derived from thebaine, widely used in both pain management and opioid dependence treatment. Its unique receptor profile—acting as a partial agonist at μ-opioid receptors—gives it a favorable safety and efficacy profile compared to full agonists.

Mechanism of Action (Stepwise Points)
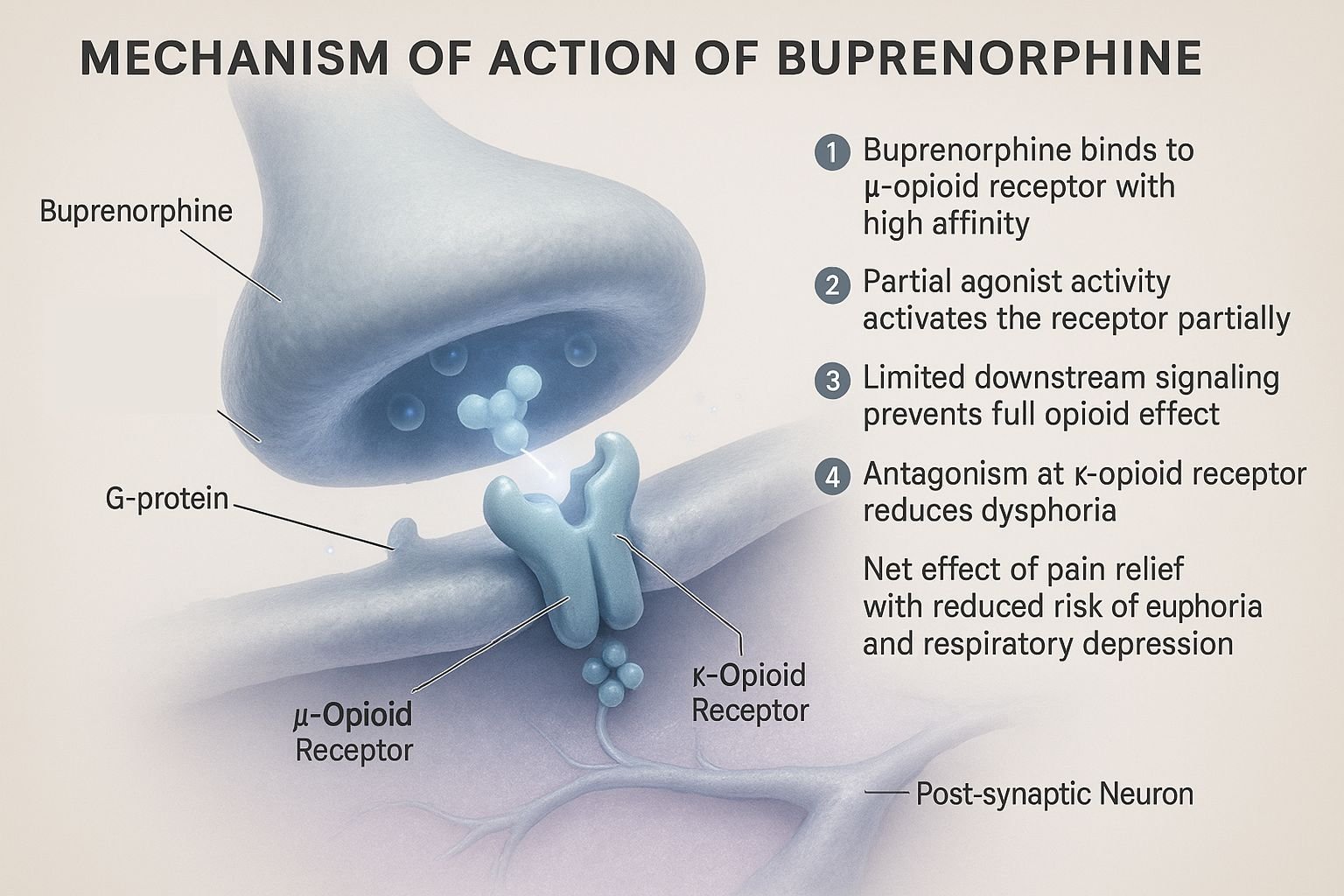
- Partial Agonist at μ-Opioid Receptors
Buprenorphine binds with high affinity but low intrinsic activity at μ-opioid receptors, resulting in moderate analgesia and ceiling effects for respiratory depression. - Antagonist at κ-Opioid Receptors
It blocks κ-receptors, reducing dysphoria and psychotomimetic effects often seen with full agonists. - Weak Antagonist at δ-Opioid Receptors
Shows minimal interaction at δ-receptors, contributing little to overall pharmacological action. - Slow Dissociation from μ-Receptors
Buprenorphine dissociates slowly, leading to prolonged effects and decreased potential for abuse. - Opioid Withdrawal Prevention
In opioid dependence, it displaces full agonists from μ-receptors, minimizing withdrawal symptoms without producing strong euphoria.


Pharmacokinetics
- Absorption: Poor oral bioavailability; well absorbed sublingually, buccally, and via transdermal patches.
- Distribution: Highly lipophilic, extensively distributed in tissues; high protein binding (~96%).
- Metabolism: Primarily hepatic via CYP3A4 to norbuprenorphine (active).
- Half-life: 24–60 hours (longer than most opioids).
- Elimination: Fecal (major route) and renal excretion.
Clinical Uses
- Opioid dependence (maintenance therapy)
- Moderate to severe chronic pain
- Perioperative analgesia (as part of multimodal approach)
- Neonatal abstinence syndrome (off-label)
Adverse Effects
- Sedation and dizziness
- Constipation
- Headache
- Nausea and vomiting
- Respiratory depression (less than full agonists)
- Precipitated withdrawal in opioid-dependent patients
- QT prolongation (with high doses)
Comparative Analysis
| Feature | Buprenorphine | Methadone | Morphine |
|---|---|---|---|
| μ-Receptor Activity | Partial agonist | Full agonist | Full agonist |
| Abuse Potential | Lower | Higher | High |
| Respiratory Depression | Ceiling effect | Dose-dependent | Dose-dependent |
| Use in Dependence | Yes | Yes | No |
| Duration of Action | Long (24–60 hrs) | Long (variable) | Short |
Explanation: Buprenorphine’s partial agonism and high receptor affinity make it an effective option for maintenance therapy with a lower risk of respiratory depression and overdose.
Multiple Choice Questions (MCQs)
- Buprenorphine is a partial agonist at which receptor?
a) NMDA
b) μ-opioid receptor
c) κ-opioid receptor
d) δ-opioid receptor - Buprenorphine’s slow dissociation from μ-receptors leads to:
a) Immediate withdrawal
b) Prolonged action
c) Faster onset
d) Antagonist effects - Which receptor does buprenorphine antagonize?
a) μ
b) κ
c) NMDA
d) GABA - What is the primary use of buprenorphine in addiction medicine?
a) Euphoria induction
b) Opioid maintenance therapy
c) Rapid detox
d) Sleep aid - Buprenorphine is metabolized by which enzyme?
a) CYP2D6
b) CYP3A4
c) CYP1A2
d) CYP2C9 - Which metabolite of buprenorphine is active?
a) Morphine
b) Norbuprenorphine
c) Codeine
d) Naloxone - Why is buprenorphine preferred over full agonists in opioid dependence?
a) Cost-effectiveness
b) Lower overdose risk
c) Rapid onset
d) High euphoria - Which side effect is less likely with buprenorphine compared to morphine?
a) Constipation
b) Respiratory depression
c) Drowsiness
d) Nausea - Buprenorphine’s activity at δ-opioid receptors is:
a) Full agonist
b) Weak antagonist
c) Inverse agonist
d) None - The sublingual route is preferred for buprenorphine because:
a) Faster metabolism
b) Cost-effectiveness
c) Avoids poor oral bioavailability
d) Enhances renal clearance
FAQs
Q1: Can buprenorphine cause withdrawal symptoms?
A1: Yes, especially if administered too soon after full opioid agonists.
Q2: Is naloxone always combined with buprenorphine?
A2: Often yes, to deter IV misuse, as in the combination product buprenorphine/naloxone (Suboxone).
Q3: Can buprenorphine be used in pregnancy?
A3: Yes, it is preferred over methadone in some cases due to better neonatal outcomes.
Q4: Does buprenorphine affect the QT interval?
A4: Yes, at higher doses, QT prolongation is possible.
References
- Goodman & Gilman’s The Pharmacological Basis of Therapeutics, 12th Edition
- KD Tripathi, Essentials of Medical Pharmacology, 7th Edition
- Pharmacological Screening Methods & Toxicology by Avanapu Srinivasa Rao
- Biopharmaceutics & Pharmacokinetics by Thakur Publication