Table of Contents
Introduction
Ketorolac is a potent nonsteroidal anti-inflammatory drug (NSAID) primarily used for short-term management of moderate to severe pain, especially postoperative pain. It is often considered an alternative to opioids due to its strong analgesic effect without causing respiratory depression. Ketorolac belongs to the acetic acid class of NSAIDs and is known for its significant analgesic and anti-inflammatory properties.
Mechanism of Action (Step-wise)
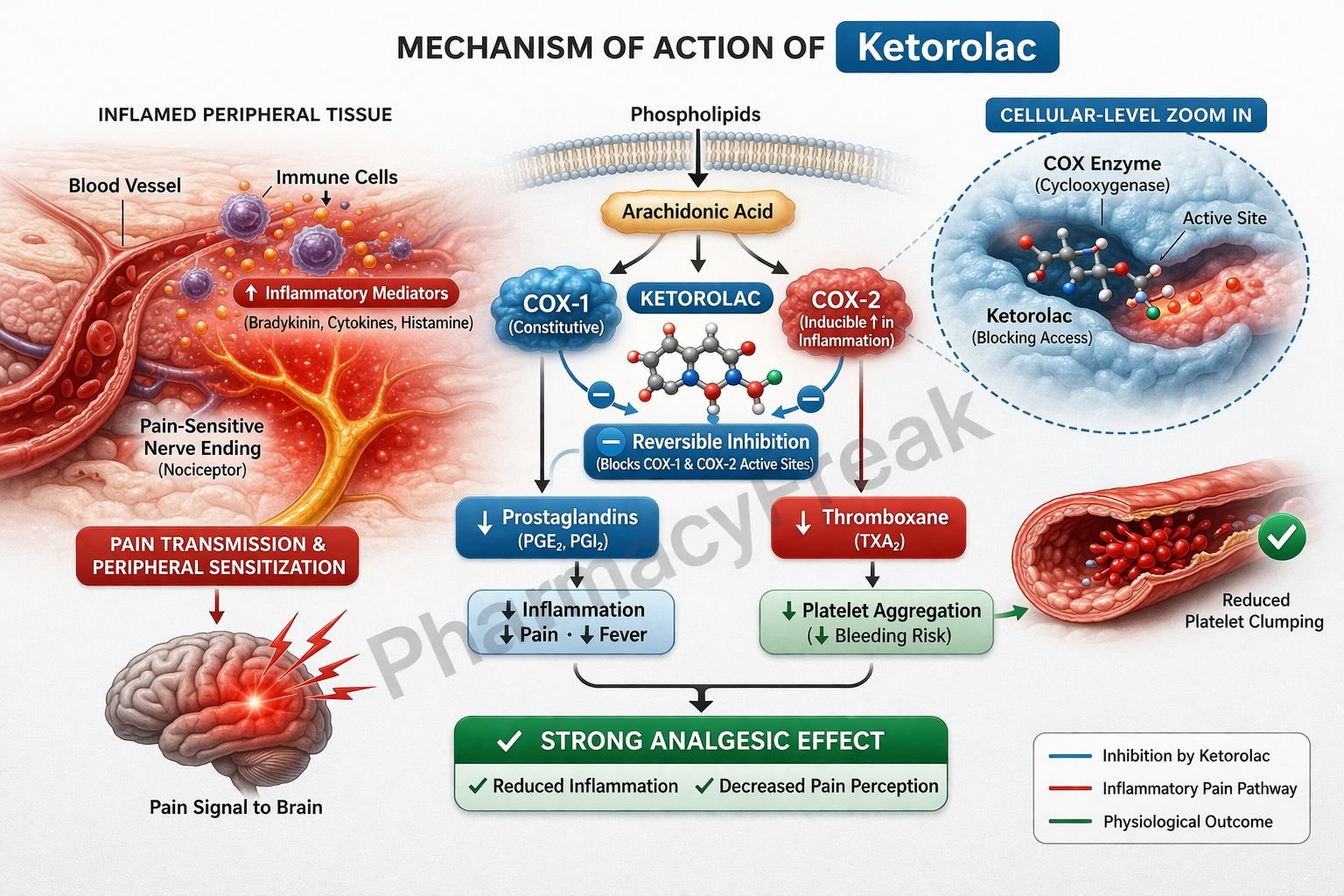
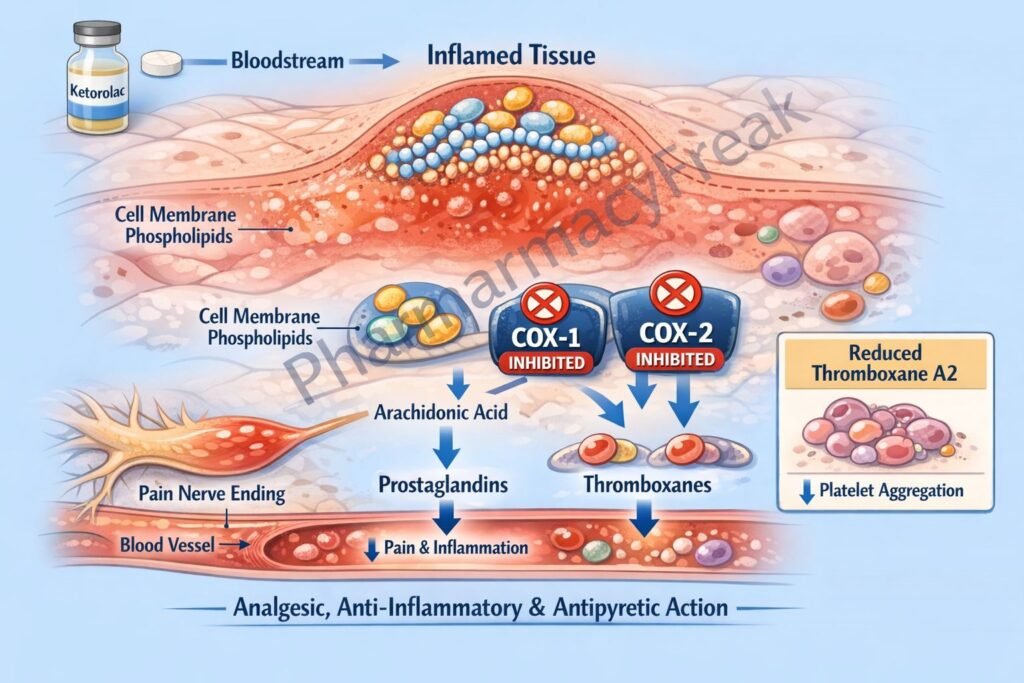
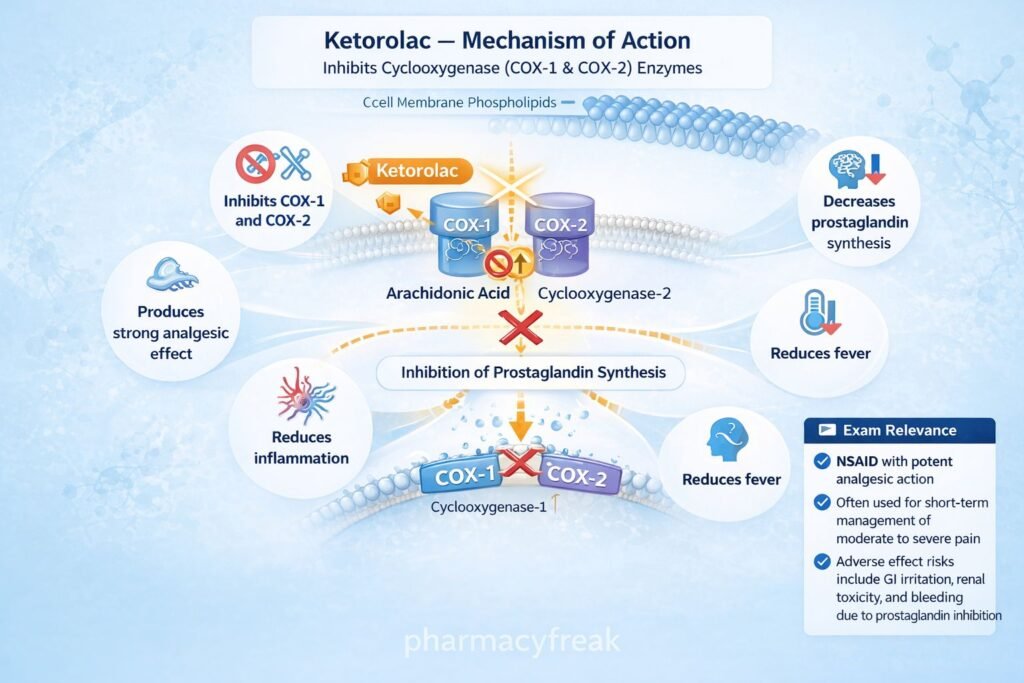
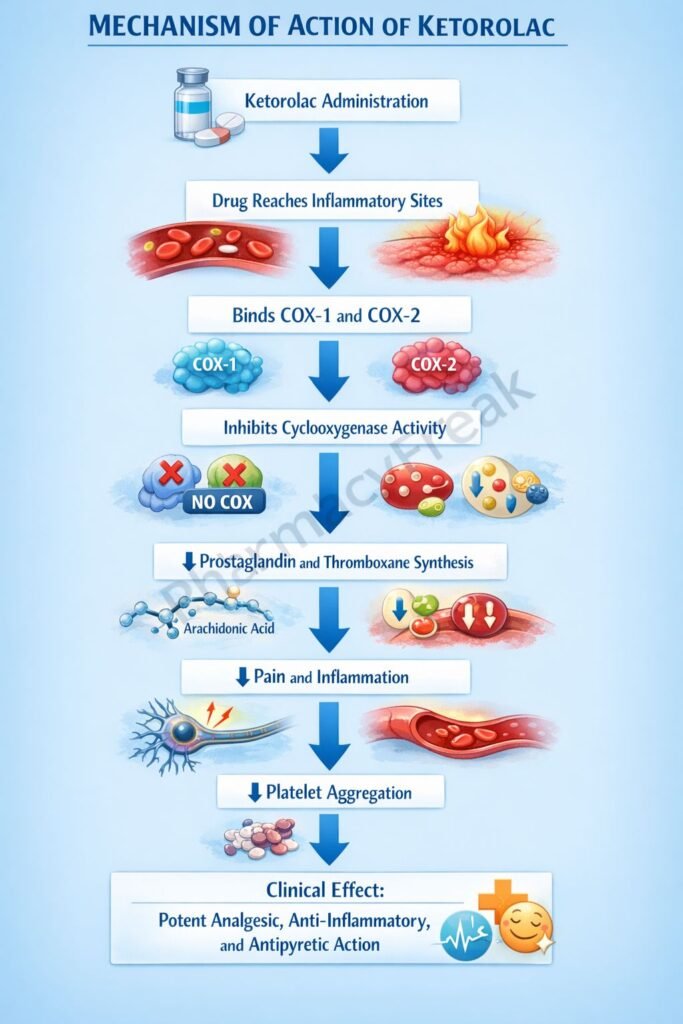
- Non-selective Cyclooxygenase (COX) Inhibition
Ketorolac inhibits both COX-1 and COX-2 enzymes. - Blockade of Arachidonic Acid Conversion
COX enzymes normally convert arachidonic acid into prostaglandins and thromboxanes. Ketorolac blocks this pathway. - Reduction in Prostaglandin Synthesis
Decreased production of prostaglandins (especially PGE2) reduces inflammation, pain, and fever. - Analgesic Effect
Lower prostaglandin levels decrease sensitization of peripheral nociceptors, leading to strong pain relief. - Anti-inflammatory Effect
Reduction in prostaglandins leads to decreased vasodilation, edema, and inflammatory response. - Antipyretic Effect
In the hypothalamus, reduced prostaglandin levels help lower elevated body temperature. - Platelet Function Inhibition
By inhibiting COX-1, ketorolac decreases thromboxane A2 (TXA2), impairing platelet aggregation (reversible effect).
Pharmacokinetics
- Administration: Oral, intramuscular, intravenous
- Absorption: Rapid and complete
- Protein Binding: High (~99%)
- Metabolism: Hepatic
- Half-life: ~5–6 hours
- Excretion: Renal (primarily as metabolites)
Clinical Uses
- Short-term management of moderate to severe pain
- Postoperative pain
- Renal colic
- Musculoskeletal pain
- Adjunct to reduce opioid requirement
Adverse Effects
- Gastrointestinal irritation, ulcers, bleeding
- Renal impairment
- Increased bleeding risk (due to platelet inhibition)
- Nausea and vomiting
- Headache and dizziness
Comparative Analysis
| Feature | Ketorolac | Ibuprofen | Morphine |
|---|---|---|---|
| Class | NSAID | NSAID | Opioid |
| Mechanism | COX inhibition | COX inhibition | μ-opioid receptor agonist |
| Analgesic potency | High (near opioid level) | Moderate | Very high |
| Anti-inflammatory | Yes | Yes | No |
| Respiratory depression | No | No | Yes |
| Risk of bleeding | High | Moderate | Low |
Ketorolac is one of the most potent NSAIDs and is often used as an opioid-sparing analgesic. Unlike opioids, it does not cause respiratory depression but carries a higher risk of gastrointestinal bleeding and renal toxicity.
MCQs
- Ketorolac primarily inhibits which enzyme?
a) Lipoxygenase
b) Cyclooxygenase
c) Phospholipase A2
d) Adenylate cyclase
Answer: b) Cyclooxygenase - Ketorolac belongs to which class?
a) Opioid
b) NSAID
c) Steroid
d) Antibiotic
Answer: b) NSAID - Main analgesic mechanism:
a) Sodium channel blockade
b) Prostaglandin inhibition
c) Dopamine increase
d) GABA activation
Answer: b) Prostaglandin inhibition - Which prostaglandin is mainly reduced?
a) PGE2
b) PGF2α
c) TXA2
d) PGD2
Answer: a) PGE2 - Platelet aggregation is affected due to:
a) Increased TXA2
b) Decreased TXA2
c) Increased prostacyclin
d) Increased serotonin
Answer: b) Decreased TXA2 - Ketorolac is commonly used for:
a) Chronic hypertension
b) Severe pain
c) Diabetes
d) Asthma
Answer: b) Severe pain - Major adverse effect:
a) Hepatotoxicity
b) GI bleeding
c) Ototoxicity
d) Neurotoxicity
Answer: b) GI bleeding - Ketorolac differs from opioids because it:
a) Causes addiction
b) Causes respiratory depression
c) Does not cause respiratory depression
d) Acts on μ receptors
Answer: c) Does not cause respiratory depression - Route NOT commonly used:
a) Oral
b) IV
c) IM
d) Inhalation
Answer: d) Inhalation - Duration of therapy should be:
a) Long-term
b) Short-term only
c) Lifelong
d) Intermittent only
Answer: b) Short-term only
FAQs
- What is the mechanism of action of ketorolac?
It inhibits COX enzymes, reducing prostaglandin synthesis and producing analgesic effects. - Why is ketorolac considered potent?
Because it provides strong analgesia comparable to opioids. - Can ketorolac cause bleeding?
Yes, due to inhibition of platelet aggregation. - Why is ketorolac used short-term only?
Because of high risk of GI and renal toxicity. - Does ketorolac cause respiratory depression?
No, unlike opioids. - Is ketorolac anti-inflammatory?
Yes, it has anti-inflammatory properties.