Mechanism of Buccal Permeation MCQs With Answer is designed to help M. Pharm students master the mechanistic principles governing drug transport across the buccal mucosa. This concise quiz blog covers passive pathways (transcellular and paracellular diffusion), physicochemical determinants (pKa, ionization, lipophilicity, molecular size), the role of mucus and intercellular lipids, and the impact of formulation variables such as mucoadhesion, permeation enhancers, and supersaturation. It also touches on advanced strategies like iontophoresis and biochemical modulation (enzyme inhibitors, calcium chelation). By linking each concept to Fick’s law and buccal anatomy/physiology, these MCQs aim to sharpen understanding for design and evaluation of buccal drug delivery systems, while emphasizing safe, reversible enhancement of permeability and avoidance of first-pass metabolism.
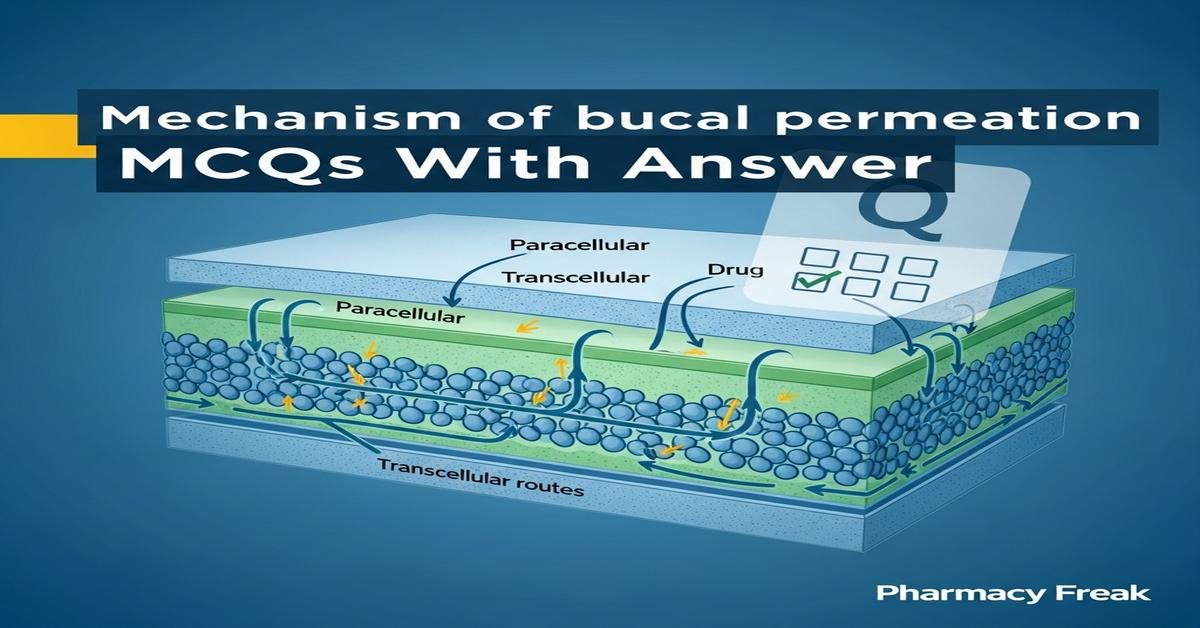
Q1. What are the two principal passive pathways for drug permeation across the buccal epithelium?
- Transcellular and paracellular diffusion
- Endocytosis via salivary ducts
- Active transport by P-glycoprotein
- Follicular penetration through appendages
Correct Answer: Transcellular and paracellular diffusion
Q2. Which surface order correctly reflects permeability among oral sites?
- Sublingual > Buccal > Palatal
- Palatal > Buccal > Sublingual
- Buccal > Palatal > Sublingual
- Palatal > Sublingual > Buccal
Correct Answer: Sublingual > Buccal > Palatal
Q3. According to Fick’s law, what is the effect of doubling epithelial thickness (h) on steady-state flux under identical donor concentration?
- Flux is halved
- Flux is doubled
- No change in flux
- Only lag time increases, not steady-state flux
Correct Answer: Flux is halved
Q4. Which physicochemical property most favors transcellular diffusion across buccal mucosa?
- Predominantly unionized at mucosal pH with logP ~1–3
- Strongly ionized at mucosal pH with logP < 0
- Highly hydrophilic (logP < −1) with MW > 1000 Da
- Amphoteric zwitterion with high crystallinity
Correct Answer: Predominantly unionized at mucosal pH with logP ~1–3
Q5. The primary barrier to paracellular transport in buccal epithelium is associated with which structural feature?
- Intercellular lipid domains rich in ceramides, cholesterol, and fatty acids
- Abundant hair follicles and sebaceous glands
- Highly vascular lamina propria
- High density of tight helical collagen in muscle
Correct Answer: Intercellular lipid domains rich in ceramides, cholesterol, and fatty acids
Q6. Which expression best describes steady-state flux (J) across buccal epithelium under sink conditions?
- J = (D × K × ΔC) / h
- J = (h × ΔC) / (D × K)
- J = K × h / (D × ΔC)
- J = D × h × K × ΔC
Correct Answer: J = (D × K × ΔC) / h
Q7. Bile salts (e.g., sodium deoxycholate) enhance buccal permeation primarily by:
- Fluidizing/extracting membrane lipids to increase K and D
- Forming covalent prodrugs in situ
- Stimulating active transcytosis via receptor mediation
- Increasing saliva flow to maintain sink conditions
Correct Answer: Fluidizing/extracting membrane lipids to increase K and D
Q8. Chitosan enhances buccal permeability mainly through which mechanism?
- Electrostatic interaction with mucins and transient widening of intercellular pathways
- Permanent dissolution of epithelial lipids
- Irreversible protein denaturation in cell membranes
- Activation of active peptide transporters
Correct Answer: Electrostatic interaction with mucins and transient widening of intercellular pathways
Q9. Calcium chelators (e.g., EDTA) promote permeation primarily by:
- Disrupting calcium-dependent cell–cell adhesion to increase paracellular transport
- Increasing drug lipophilicity via complexation
- Thickening the mucus layer to slow clearance
- Inhibiting salivary amylase to protect peptides
Correct Answer: Disrupting calcium-dependent cell–cell adhesion to increase paracellular transport
Q10. Which statement best describes the role of the mucus layer in buccal permeation?
- Negatively charged, viscoelastic barrier that can trap cationic macromolecules and slow diffusion
- Hydrophobic barrier that accelerates passage of polar drugs
- Primary site of active transport for small molecules
- Devoid of turnover, forming a static layer for hours
Correct Answer: Negatively charged, viscoelastic barrier that can trap cationic macromolecules and slow diffusion
Q11. Mucoadhesive buccal patches enhance permeation predominantly by:
- Maintaining intimate contact to increase effective ΔC and residence time at the epithelial surface
- Decreasing membrane thickness (h) by chemical erosion
- Increasing drug metabolism in the epithelium
- Reducing drug solubility to limit dose dumping
Correct Answer: Maintaining intimate contact to increase effective ΔC and residence time at the epithelial surface
Q12. Which profile is most suitable for passive buccal absorption?
- MW < 500 Da, logP 1–3, unionized at pH 6–7
- MW ~1500 Da, logP −2, fully ionized
- MW ~800 Da, logP 6, crystalline and poorly soluble
- Highly hydrophilic peptide without any enhancer
Correct Answer: MW < 500 Da, logP 1–3, unionized at pH 6–7
Q13. Increased salivary flow during dosing typically:
- Reduces residence time and concentration at the mucosa, lowering absorption
- Increases ΔC at the surface, enhancing absorption
- Opens intercellular pathways via mechanical stress
- Inhibits buccal enzymes to protect peptides
Correct Answer: Reduces residence time and concentration at the mucosa, lowering absorption
Q14. A key biochemical barrier for peptide drugs in the buccal route is:
- Proteolytic activity in saliva and epithelial layers
- Lack of blood supply in lamina propria
- High density of efflux transporters in mucus
- Presence of hair follicles acting as sinks
Correct Answer: Proteolytic activity in saliva and epithelial layers
Q15. For a weak base (pKa 8) dosed in the buccal cavity (pH ~6.5), which formulation change can improve transcellular permeation?
- Include an alkalizing agent to increase unionized fraction
- Add an acidifying agent to increase ionization
- Decrease drug solubility to reduce ΔC
- Inhibit saliva to reduce hydration
Correct Answer: Include an alkalizing agent to increase unionized fraction
Q16. Iontophoresis across buccal mucosa enhances transport primarily via:
- Electromigration of charged species and electroosmosis of neutrals
- Photochemical activation of drug molecules
- Formation of permanent pores in epithelium
- Thermal denaturation of mucins
Correct Answer: Electromigration of charged species and electroosmosis of neutrals
Q17. Which statement about keratinization and buccal permeability is accurate?
- Non-keratinized buccal mucosa is more permeable than keratinized palatal mucosa
- Keratinized palatal mucosa is more permeable than sublingual mucosa
- Keratinization has no effect on permeability
- Buccal mucosa is fully keratinized in healthy adults
Correct Answer: Non-keratinized buccal mucosa is more permeable than keratinized palatal mucosa
Q18. Increasing the thermodynamic activity of a drug at the buccal surface (e.g., via supersaturation) primarily:
- Increases the driving force (ΔC), raising flux
- Decreases K by reducing lipophilicity
- Increases h by dehydrating the membrane
- Eliminates the need for mucoadhesion
Correct Answer: Increases the driving force (ΔC), raising flux
Q19. The rate-limiting barrier for many small molecules across non-keratinized buccal mucosa is best attributed to:
- Intercellular lipid organization in the superficial epithelial layers
- Vascular resistance in submucosa
- Muscle layer thickness beneath lamina propria
- Salivary gland ducts providing rapid shunts
Correct Answer: Intercellular lipid organization in the superficial epithelial layers
Q20. Why does buccal administration help bypass hepatic first-pass metabolism?
- Venous drainage from buccal mucosa enters systemic circulation directly (e.g., via jugular), not the portal vein
- Drugs are converted to inactive metabolites before absorption
- Buccal mucosa lacks enzymes entirely
- All absorbed drug is stored in mucus before release
Correct Answer: Venous drainage from buccal mucosa enters systemic circulation directly (e.g., via jugular), not the portal vein

I am a Registered Pharmacist under the Pharmacy Act, 1948, and the founder of PharmacyFreak.com. I hold a Bachelor of Pharmacy degree from Rungta College of Pharmaceutical Science and Research. With a strong academic foundation and practical knowledge, I am committed to providing accurate, easy-to-understand content to support pharmacy students and professionals. My aim is to make complex pharmaceutical concepts accessible and useful for real-world application.
Mail- Sachin@pharmacyfreak.com